Purpose
Magnetic Resonance Imaging (MRI) is a powerful imaging technique to evaluate prostate cancer [1].
Combining morphological with metabolic data provided by three-dimensional Magnetic Resonance Spectroscopy (MRS) may improve specificity and accuracy,
but it requires a more difficult and time-consuming image interpretation [2].
Some reports have demonstrated that MRI accuracy significantly improves with radiologist’s experience [3],
in relation to interpreted exams number.
Our purpose was to evaluate the learning curve of a young unexperienced radiologist in the study of prostate cancer with 1.5 T MRI/MRS.
Methods and Materials
We performed Magnetic Resonance Imaging/Spectroscopy (MRI/MRS) with a 1.5 T scanner in 115 consecutive patients (mean age and SD: 67.8 ± 7.1,
from September 2009 to July 2010) with PSA values from 2.5 to 10 ng/ml,
before they underwent a 12-cores sampling primary TRUS biopsy.
In 20 patients endorectal coil was not used. MRI included high resolution transverse,
coronal,
and sagittal T2-weighted sequences.
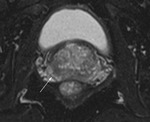
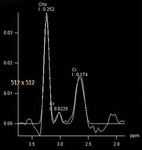
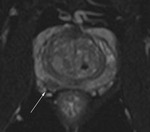
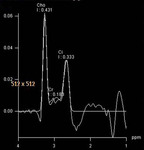
Spectroscopy data were acquired by a 3D chemical shift imaging pulse sequence.
Peripheral areas with a low signal on T2-w images and...
Results
All values showed a positive trend from the first to the third group of patients (tab.1). Young radiologist performance in the first group of patients was the following: SEN 0.57; SPE 0.52; NPV 0.65; PPV 0.44; ACC 0.54.
Young radiologist performance in the second group was the following: SEN 0.73; SPE 0.50; NPV 0.80; PPV 0.40; ACC 0.57.
Young radiologist performance in the third group was the following: SEN 0.77; SPE 0.68; NPV 0.83; PPV 0.59; ACC 0.71.
Conclusion
According to our data,
young radiologist improves his performance in MRI/MRS interpretation after a relatively short number of exams.
Sensibility and NPV significantly improve from the first group to the second group of patients,
while specificity,
PPV and accuracy only significantly increase in the third group of patients.
After reviewing the first group of patients at the light of biopsies results,
false negatives reduce,
with a better ability to recognize tumours.
A slight further improvement in sensibility also occurs in the third group.
On the...
References
Choi YJ,
Kim JK,
Kim N,
Kim KW,
Choi EK,
Cho KS.Functional MR imaging of prostate cancer.
Radiographics 2007;27:63-75.
Cirillo S,
Petracchini M,
Della Monica P,
et al.
Value of endorectal MRI and MRS in patients with elevated prostate-specific antigen levels and previous negative biopsies to localize peripheral zone tumours.
Clin Radiol 2008;63:871–9.
Latchamsetty KC,
Borden LS Jr,
Porter CR,
et al.
Experience improves staging accuracy of endorectal magnetic resonance imaging in prostate cancer: what is the learning curve? Can J Urol 2007;14:3429-34.
Umbehr M,...
Personal Information
drs.
Antonella Petrillo,
INT "G.
Pascale",
Via Mariano Semmola,
Naples,
Italy.
[email protected]