Purpose
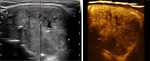
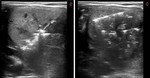
Image-guided ablations have been increasingly using as an alternative treatment to surgery in the management of clinically relevant benign thyroid nodules.The two most widely used techniques for benign nodule image guided thermal ablation areradiofrequency ablation (RFA) and laser ablation (LA).
The purpose of this study was to compare our results in the treatment of benign thyroid nodules withRFA and with LA.
Methods and materials
From 2011,
63 patients (12 males,
41 females) underwent percutaneous thermal ablation for a benign thyroid nodule.
32 (4 males,
28 females) underwent treatment with RFA (,
and 31 (8 males,
23 females) underwent PLA under ultrasound guidance.
We used an internally cooled electrode with 17-18 gauge calibre and 0.5-1.5-cm active tip (AMICA,
HS Hospital Service,
Aprilia,
Italy) and the moving-shot technique for RFA ablation.
We used a continuous-wave Nd-YAG laser operating at 1.064 mm (EchoLaser X4©,
Esaote,
Genoa,
Italy) for LA.
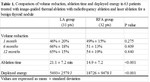
Mean nodule volume...
Results
Mean nodule volume before ablation was 19.2 ± 17.1 ml (mean ± standard deviation) in PLA group vs 35.1 ± 22.2 ml in RFA group (p = 0.002).
Mean time for ablation was significantly longer in PLA (21.1 ± 7.2 min vs 14.9 ± 7.2; p<0.001),
while mean energy deployment was significantly higher in RFA group (18726 ± 9478 J vs 5493± 2579 J; p< 0.001).
Mean volume reduction at 1-2 months was 46% ± 20% in PLA group compared with 49% ± 15% in...
Conclusion
PLA and RFA offers similar results in terms of volume reduction at 1-2 months and 6 months.
PLA requires significantly longer times and lower energy deployment than RFA
References
Baek,
J.
H.,
Kim,
Y.
S.,
Lee,
D.,
Huh,
J.
Y.,
& Lee,
J.
H.
(2010).
Benign predominantly solid thyroid nodules: prospective study of efficacy of sonographically guided radiofrequency ablation versus control condition.
AJR.
American Journal of Roentgenology,
194(4),
1137–42.
doi:10.2214/AJR.09.3372
Goldberg,
S.
N.,
Gazelle,
G.
S.,
Solbiati,
L.,
Rittman,
W.
J.,
& Mueller,
P.
R.
(1996).
Radiofrequency tissue ablation: increased lesion diameter with a perfusion electrode.
Academic Radiology,
3(8),
636–44.
Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/8796727
Lim,
H.
K.,
Lee,
J.
H.,
Ha,
E.
J.,
Sung,
J....