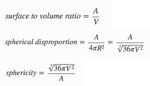Aims and objectives
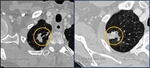
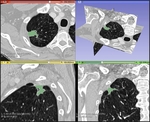
Benign and malignant pulmonary nodules often have very similar computed tomography (CT) imaging visual features (Figure 1).
Therefore,
the conventional inspection currently practiced by radiologists fails to differentiate malignant from benign nodules [1].
To help radiologists,
TheFleischner society pulmonary nodule recommendationsare used for management ofpulmonary nodules [2].
Recent studies have shown promising results of shape and texture analysis in the field of oncology,
primarily tumour assessment for predicting prognosis and treatment response [3,
4,
5].
The purpose of this works is to assess the accuracy...
Methods and materials
We have evaluated 65 CT scans of lungs.
Dataset were randomly extracted from the SPIE-AAPM Lung CT Challenge archive [5,
6,
7,
8].
Studies were obtained on multi-detector CT system (Philips Brilliance).
All CT scans were performed with high resolution convolution kernel and 1 mm reconstruction slice thickness; 18 CT scans were unenhanced,
whereas 47 CT scans were acquired after iodine contrast administration.
All nodules within these scans were classified by an expert radiologist to be either primary lung cancer or benign nodules,
based on...
Results
A total of 70 nodules,
of which 36 benign nodules and 34 primary lung cancers,
met the inclusion criteria.
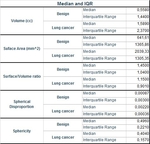
The median and interquartile range (IQR) results for shape features for benign nodules and lung cancers are shown in Figure 4.
Mann-Whitney U test demonstrated significant differences in shape analysis results among benign nodules and lung cancers (P<0.05) for Volume,
Surface area,
Spherical disproportion and Sphericity (Figure 5).
AUCs corresponding to all TA features were greater than 0.5 (Figure 6 and 7).
In particular AUC for...
Conclusion
Our results demonstrated that quantitative shape analysis has the potential to allow CT differentiation between benign and malignant pulmonary nodules.
If data are confirmed from further validation,
shape analysis in combination with texture analysis could be a support to select suspicious nodules for further diagnostic investigations.
It may also be particularly relevant to exclude patients at risk for invasive diagnostic procedures,
when shape and textural features suggest a benign etiology.
Personal information
R.
Casale,
MD
Hospital "San Tommaso dei Battuti" Portogruaro,ULSS 4 Veneto Orientale,
Department of Radiology - Veneto Italia.
Via Piemonte 1
30026 Portogruaro (Ve),
Italia
Phone: +39 3394127134
e-mail:
[email protected]
References
Gould MK,
Donington J,
Lynch WR,
Mazzone PJ,
Midthun DE,
Naidich DP,
Wiener RS.
Evaluation of individuals with pulmonary nodules: when is it lung cancer? Diagnosis and management of lung cancer,
3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines.
Chest.
2013 May;143(5 Suppl):e93S-e120S
MacMahon H,
Naidich DP,
Goo JM,
Lee KS,
Leung ANC,
Mayo JR,
Mehta AC,
Ohno Y,
Powell CA,
Prokop M,
Rubin GD,
Schaefer-Prokop CM,
Travis WD,
Van Schil PE,
Bankier AA.
Guidelines for Management of Incidental Pulmonary Nodules Detected...