Aims and objectives
To measure response to cancer treatment RECIST (Response Evaluation Criteria in Solid Tumours) is most widely used in clinical practice,
particularly in the scope of clinical trials.
The RECIST system classifies the response into a complete or partial response,
stable or progressive disease,
as displayed schematically inFig. 1 (1).Nowadays radiologists in the Netherlands Cancer Institute measure lesions using RECIST 1.1,
the most recent available version of RECIST.
Radiologists experience this assessment as a time consuming process.
Given the well defined and standardized methodology of the...
Methods and materials
Patient population:
In this retrospective study 32 patients with a variety of cancer-types were included.
Patients were diagnosed with lung,
colorectal,
ovarian,
liver,
urothelial cell,
breast,
head & neck, melanoma and neuroendocrine tumors.
Data acquisition:
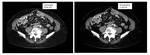
All patients underwent a baseline CT-scan (prior to treatment) and 2 follow-up (FU)-scans for response evaluation according to RECIST1.1 between 2012 and 2015 at our institution.
Average time between CT-scans was 51 days (range 23 to 133 days).
CT-scans were contrast-enhanced acquisitions of the neck,
chest and/or abdomen and were...
Results
In total 89 lesions were analyzed.
The distribution of response categories according to RECIST 1.1 for the two FU moments determined by radiologists is given in Table 1.There were no patients with a complete response after two FU moments.
Table 1.
Response catergories according to RECIST 1.1 by radiologists
Partial response
Stable disease
Progressive disease
FU1
19%
75%
6%
FU2
28%
63%
9%
Kappa values to compare response between radiologists and radiographers are provided in Table 2.
For the first FU-scan,
interobserver agreement was excellent...
Conclusion
The good-excellent agreement between radiographers and radiologists suggests that follow-up RECIST-measurements can be performed by radiographers.
The slightly lower IOA for the second follow-up scan (compared to follow-up 1) can probably be explained because lesions were smaller due to ongoing response.
Radiographers need to be further trained to avoid major and minor interpretation and measurement errors.
Personal information
L.
Molenaar,
radiographer,
Department of Radiology,
Netherlands Cancer Institute.
P.O.
Box 90203,
1006 BE Amsterdam,
the Netherlands Phone: +31205129111 email:
[email protected]
M.
A.
van der Lubbe,
radiographer,
Department of Radiology,
Netherlands Cancer Institute.
P.O.
Box 90203,
1006 BE Amsterdam,
the Netherlands Phone: +31205129111 email:
[email protected]
F.
van der Krieke,
radiographer,
Department of Radiology,
Netherlands Cancer Institute.
P.O.
Box 90203,
1006 BE Amsterdam,
the Netherlands Phone: +31205129111
Dr.
M.
Lahaye,
radiologist,
Department of Radiology,
Netherlands Cancer Institute.
P.O.
Box 90203,
1006 BE Amsterdam,
the Netherlands Phone:...
References
Eisenhauer EA,
Therasse P,
Bogaerts J,
Schwartz LH,
Sargent D,
Ford R,
et al.
New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1).
Eur J Cancer [Internet].
2009 Jan [cited 2017 Dec 20];45(2):228–47.
Available from: http://www.ncbi.nlm.nih.gov/pubmed/19097774
Sailer AM,
Douwes DCE,
Cappendijk VC,
Bakers FC,
Wagemans BAJM,
Wildberger JE,
et al.
RECIST measurements in cancer treatment: is there a role for physician assistants? - A pilot study.
Cancer Imaging [Internet].
2014 Apr 22 [cited 2018 Jan 7];14:12.
Available from: http://www.ncbi.nlm.nih.gov/pubmed/25608556