Learning objectives
To describe and illustrate CT and MRI findings of different faces of pancreatic ductal adenocarcinoma (PDAC).
Background
Pancreatic ductal adenocarcinoma (PDAC) is one of the most malignant cancer forms.
It is fourth most common cause of cancer death worldwide,
with a poor overall 5-year survival rate of only 4 %,
reasonably earning the name “silent killer”.
The treatment depends upon tumour resectability at presentation,
therefore,
radiological imaging is crucial in the management of the disease [2-3].
Currently,
multi-detector computed tomography (MDCT) is the most commonly used,
best-validated imaging modality for the diagnosis and staging of pancreatic cancer.
Modern contrast-enhanced magnetic resonance imaging...
Findings and procedure details
CT protocols in evaluating pancreatic lesions varies from institution to institution,
but typically are multiphasic with thin-section imaging (≤3mm) and with multi-planar reconstructed (MPR) images (coronal and/or sagittal planes).
Despite optimal CT imaging,
PDAC can be falsely considered as locally resectable,
without CT signs of distant metastasis,
since focal areas of micro-metastasis might not be differentiated during CT scan [1].
In such cases MRI becomes essential.
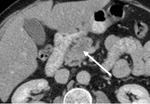
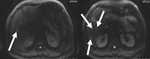
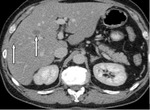
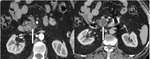
Case 1. 60 year old male with weight loss ~10 kg/6 months and painless jaundice; laboratory tests: slightly elevated...
Conclusion
It is essential to correctly perform radiological imaging to obtain optimal locoregional analysis in patients with PDAC.
It’s important to search for the criteria of locally advanced or metastatic disease,
performing both: CT and MRI.
Close cooperation between the oncologist,
the surgeon and the radiologist is crucial in order to avoid possible mistakes and pitfalls.
References
1.
Jason Alan Pietryga,
Desiree E.
Morgan.
Imaging preoperatively for pancreatic adenocarcinoma.
J Gastrointest.
Oncol.
2015 Aug; 6(4): 343-357.
2.
Evans db,
george B,
Tsai S.
Non metastatic pancreatic cancer: resectable,
borderline resectable,
and locally advanced-definitions of increasing importance for the optimal delivery of multimodality therapy.
Ann SurgOncol.
2015;22 (11):3409-13
3.
Gillen S,
Schuster T,
Meyer ZumBuschenfelde C,
Friess H,
Kleeff J.
Preoperative / neoadjuvant therapy in pancreatic cancer: a systematic review and meta-analysis of response and resection percentages.
PloS Med.
2010;7(4):e1000267
4.
Wong JC,...