Learning objectives
Review the typical anatomy of the thoracic duct.
Outline the causes of thoracic duct injury and the indications for thoracic duct embolization.
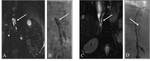
Review thoracic duct embolization pre-procedural imaging such asmagnetic resonance ductography andlymphangiography.
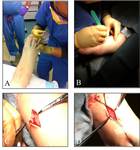
Describe thoracic duct embolization intra-procedural techniques including: cut-down,
lymphatic duct isolation,
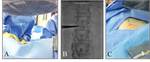
and pedallymphangiography,lowerextremity lymphangiography,
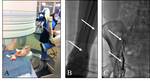
cisterna chyli access and cannulization,thoracic duct lymphangiography,
and thoracic duct embolization.
Discuss thoracic duct embolization procedural success and complications.
Background
The thoracic duct is the largest lymphatic conduit,
draining upwards of seventy-five percent of lymphatic fluid,
and extending from the cisterna chyli to the left jugulovenous angle.
The lengthy course of the thoracic duct predisposes it to injury from a variety of iatrogenic causes including: thoracic,
cardiac,
and head and neck surgeries as well as spontaneous benign or malignant lymphatic obstructions.
Disruption of the thoracic duct frequently results in chylothoraces that subsequently cause an immunocompromised state,
result in nutritional depletion,
and impair respiratory function,
but...
Findings and procedure details
Anatomy of the Thoracic Duct:
Tubular structure extending from cisterna chyli at the the second lumbar vertebral bodyto the junction of the left subclavian and left interval jugular veins [1,2].
Originates at the abdominal cisterna chyli,
extends along the posterior aspect of the aorta and right diaphragmatic crus,
and enters the thorax between the aorta and azygos vein.
Courses through the posterior mediastinum deep to the esophagus and pericardium.
Enters the superior mediastinum at the fifth thoracic vertebral body and extends posterior to the aortic...
Conclusion
The thoracic duct may be injured in a variety of surgical procedures as well as obstructing processes,
predisposing individuals to chylothoraces,
chylopericardium,
andpostoperative chylous wound leakages,
leading tonutritional depletion and impaired respiratory function.Knowledge of thoracic duct anatomy coupled with awareness of appropriate thoracic duct embolization techniques allows highly successful treatment with minimal morbidity or mortality.
Personal information
Jeffrey Forris Beecham Chick,
MD,
MPH
PGY V Department of Radiology
Brigham and Women's Hospital
Harvard Medical School
[email protected]
Nikunj Rashmikant Chauhan,
MD
PGY V Department of Radiology
Brigham and Women's Hospital
Harvard Medical School
[email protected]
Alisa Siziki Han,
MD
Instructor of Radiology
Brigham and Women's Hospital
Harvard Medical School
[email protected]
References
[1] Skandalakis JE,
Skandalakis LJ,
Skandalakis PN.
Anatomy of the lymphatics.
Surg Oncol Clin N Am.
2007;16(1):1-16.
[2] Agur AMR,
Dalley AF,
Grant JCB.
Grant's Atlas of Anatomy.
11th ed.
Philadelphia: Lippincott Williams & Wilkins; 2005.
[3] Dunn RP.
Primary chylopericardium: a review of the literature and an illustrated case.
Am Heart J.
1975;89(3):369-377.
[4] Itkin M,
Swe NM,
Shapiro SE,
Shrager JB.
Spontaneous chylopericardium: delineation of the underlying anatomic pathology by CT lymphangiography.
Ann Thorac Surg.
2009;87(5):1595-1597.
[5] Doerr CH,
Allen MS,
Nichols FC,...