Learning objectives
To describe the most relevant radiologic manifestations of pulmonary paracoccidioidomycosis.
To understand the clinical and epidemiologic features of paracoccidioidomycosis.
To perform a proper differential diagnosis in order to establish the best possible therapeutic approach.
Background
Etiologic agent and pathogenesis
Paracoccidioidomycosis is caused by Paracoccidioides brasiliensis and Paracoccidioides lutzii,
thermally dimorphic fungi believed to be soil saprophytes.
In its mycelial form,
Paracoccidioides spp produces infectious propagules known as microconidia that reach the alveoli after being inhaled; once in the lungs,
they interact with pulmonary macrophages and convert into a yeast form[1].
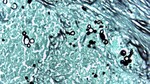
The latter form produces the appearance typically described in histopathological studies as a “pilot’s wheel”,
consisting of a mother cell surrounded by multiple blastoconidia (Fig.
1).
The infection usually produces...
Findings and procedure details
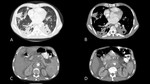
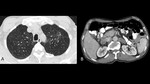
Radiological findings in patients with the chronic form of paracoccidioidomycosis are very diverse and there is frequently a combination of patterns such as reticular and nodular opacities,
airspace consolidation,
cavities and fibrotic lesions showing a tendency for bilateral and symmetrical distribution[6]and usually involving more than one third of the lungs (Fig.
2); however,
pleural effusion and pulmonary calcifications are seldom observed.
A discrete predominance in the middle lung zones has been reported and its association with lower lobe emphysema could suggest the diagnosis when found...
Conclusion
Paracoccidioidomycosis is the most common systemic mycosis in Latin America.
Although lungs are the primary target of this disease,
its polymorphic presentation represents a challenge both for clinicians and radiologists; however,
proper recognition of imaging patterns along with identification of epidemiological risk factors may allow to reach a correct diagnosis.
Accordingly,
radiologists play a very important role in the management of these patients since an early diagnosis facilitates a better therapeutic approach with subsequent improvement in morbidity and mortality.
Personal information
Dr.
Jhonathan Reina
Resident in training.Department of Radiology,
Universidad de Antioquia.
Medellín,
colombia.
Email:
[email protected]
Dr.
Maria Fernanda Saldarriaga
Resident in training.Department of Radiology,
Universidad de Antioquia.
Medellín,
colombia.
Email:
[email protected]
Dr.
Tatiana Suárez
Radiology assistant professor.Department of Radiology,
Universidad de Antioquia.
Medellín,
colombia.
Email:
[email protected]
References
Queiroz-Telles F,
Escuissato D.
Pulmonary Paracoccidioidomycosis.
Semin Respir Crit Care Med [Internet].
2011 Dec 13 [cited 2018 Jan 12];32(6):764–74.
Available from: http://www.thieme-connect.de/DOI/DOI?10.1055/s-0031-1295724
Restrepo A,
Benard G,
de Castro C,
Agudelo C,
Tobón A.
Pulmonary Paracoccidioidomycosis.
Semin Respir Crit Care Med [Internet].
2008 Apr [cited 2018 Jan 12];29(2):182–97.
Available from: http://www.ncbi.nlm.nih.gov/pubmed/18366000
Calle D,
Rosero DS,
Orozco LC,
Camargo D,
Castañeda E,
Restrepo A.
Paracoccidioidomycosis in Colombia: an ecological study.
Epidemiol Infect [Internet].
2001 Apr [cited 2018 Jan 12];126(2):309–15.
Available from: http://www.ncbi.nlm.nih.gov/pubmed/11349982
Brummer E,
Castaneda E,
Restrepo...