Learning objectives
Glioblastoma is the most common primary malignant brain tumor in adults and it is associated with a dismal prognosis (median survival time of patients only 3 to 9 months after first recurrence).
Current standard of care is STUPP scheme: surgical resection followed by radiotherapy (RT) and concomitant and adjuvant temozolomide (TMZ) chemotherapy.
What are the main problems of brain tumors?
Infiltrating tumors,
indistinct borders
Difficult to differentiate tumor infiltration,
edema,
gliosis and post-RT changes
Enhancement only reflects blood brain barrier (BBB) permeability
Problems to distinguish...
Background
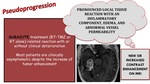
PSEUDOPROGRESSION is a subacute treatment (RT-TMZ or RT alone) related reaction with or without clinical deterioration.
Most patients are clinically asymptomatic despite the increase of tumor enhancement.
There is a pronounced local tissue reaction with an inflammatory componente,
edema and abnormal vessel permeability.
NEW OR INCREASED CONTRAST ENHANCEMENT ON MRI
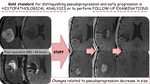
Gold standard for distinguishing pseudoprogression and early progression is histopathological analysis or to perform follow-up examinations.
Pseudoprogression represents an active "inflammatory" response against the tumor and is related to increased survival.
Patients with methylated MGMT...
Findings and procedure details
Problematic analysis of pseudoprogressions:
At conventional imaging:
Pseudoprogression: self-limited enhancing lesions that spontaneously stabilize and resolve without treatment.
True progression. During the first 12 weeks after RT+QT or RT alone:
New enhancement outside radiation field
Pathologic confirmations of progressive disease
Subependymal enhancement
With conventional techniques,
in most cases it is not possible to differentiate pseudoprogression and true progression.
At DWI:
Pseudoprogression: higher ADC values in treatment related changes
True progression: lower ADC values
ADC values may differentiate between true progression and pseudoprogression. Tumor recurrence usually...
Conclusion
Accurate differentiation between pseudoprogression and true progression remains challenging for optimal treatment.
Diffusion and perfusion MRI may demonstrate different diagnostic values for predicting pseudoprogression in treated gliomas.
Personal information
Amaya Hilario
Department of Radiology.
Neuroradiology section.
Universitary Hospital 12 de Octubre,
Madrid,
Spain.
References
1.
Hygino da Cruz Jr LC,
Rodriguez I,
Domingues RC,
Gasparetto EL,
Sorensen AG.
Pseudoprogression and Pseudoresponse: Imaging Challenges in the Assessment of Posttreatment Glioma.
AJNR 2011;32:1978-85
2.
Prager AJ,
Martinez N,
Beal K,
Omuro A,
Zhang Z,
Young RJ.
Diffusion and Perfusion MRI to Differentiate Treatment-Related Changes including Pseudoprogression from Recurrent Tumors in High-Grade Gliomas with Histopathologic Evidence.
AJNR Am J Neuroradiol 2015;36:877-85.
3.
Yun TJ,
Park C-K,
Kim TM,
Lee S-H,
Sohn C-H,
Park S-H.
Glioblastoma treated with Concurrent Radiation Therapy and Temozolomide...