Purpose
Liver Transplantation (LT) is the preferred treatment for selected patients with hepatocellular carcinoma (HCC),
however a debate still exists over which patients should be considered for LT.
The Milan criteria,
first described in 1996 (1) and widely adopted,
have been recently considered too restrictive and expanded selection criteria have been proposed (2).
Anyhow,
with the prognostic relevance of tumor size and number of lesion,
preoperative staging is crucial for patient selection based on the above-mentioned criteria and organ allocation.
Both contrast-enhanced dynamic multidetector Computed Tomography...
Methods and Materials
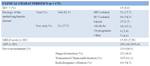
Patients.
Between October 2004 and November 2011,
a total of 183 consecutive patients with HCC underwent LT at our hospital.
Of them,
8 patients were excluded because of a short follow up period (≤2 months),
as a result of perioperative mortality.
The remaining 175 patients (151 men,
24 women),
who had a follow-up period longer than 2 months and had undergone dymanic-imaging evaluation at least 3 months before transplantation,
were included.
Previous treatment,
including surgical resection and loco-regional therapies had been undertaken in 119 patients....
Results
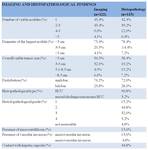
Imaging and histopathological data.
Of the 175 patients who were included,
122 (69,7%) patients had evidence of viable tumor on imaging examination,
79 of them having undergone treatment before LT.
The remaining 53 patients had no evidence of viable tumor and 40 of them had undergone treatment before LT.
On histopathology,
125 patients (71,4%) had evidence of viable tumor,
while there were no viable HCCs present on the explanted liver in 50 patients.
The other collected imaging and histopathological features are summarized in table 2....
Conclusion
According to our results,
contrast-enhanced imaging can be considered accurate in pretransplantation staging of HCC as a high radiologic-pathologic correlation was found in the detection of viable tumor and in the assessment of parameters such as number of nodules or diameter of the larger nodule,
which are crucial for HCC staging.
The association between imaging and histopathology in the detection of viable tumor remained also when pretransplantation treatment and in particular TACE (p<0,001) and RITA (p=0,006) had been undertaken before LT.
This result is remarkable...
References
Mazzaferro V,
Regalia E,
Doci R et al.
Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis.
N Engl J Med.
1996 Mar 14;334(11):693-9.
Yao FY,
Ferrell L,
Bass NM et al.
Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival.
Hepatology.
2001 Jun;33(6):1394-403.
Noguchi Y,
Murakami T,
Kim T et al.
Detection of hepatocellular carcinoma: comparison of dynamic MR imaging with dynamic double arterial phase helical CT.
AJR Am J Roentgenol.
2003 Feb;180(2):455-60....