Aims and objectives
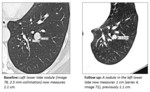
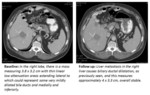
Tumor response to anticancer therapy is frequently determined by a change in the cumulative sizes of target lesions as measured on serial imaging examinations.
Formal measurement of tumors began in 1979 with the World Health Organization’s criteria employing bi-dimensional measurements (1).
In 2000,
the Response Evaluation Criteria In Solid Tumors (RECIST) criteria emerged to simplify tumor assessment with uni-dimensional measurements of selected target lesions,
and this was later refined in 2009 with a reduction in the number of required target lesions as well as guidance...
Methods and materials
Institutional Review Board approval was granted for this retrospective review.
We analyzed the baseline and subsequent radiology reports from 97 patients with advanced cancer treated in three Phase I clinical trials at our institution to determine if radiologists performed the following:
Reported tumor measurements
Saved relevant annotated images containing measurements in the institution’s picture archiving and communication system (PACS) for later recall
Reported on the same baseline lesions during subsequent follow up examinations.
Results
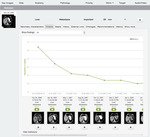
We analyzed the baseline and subsequent radiology reports from 97 consecutive patients enrolled in clinical trials (194 total reports) which revealed that radiologists reported tumor measurements in 92% of all examinations but saved relevant annotated images in the PACS system in only 34% of baseline and 42% of follow up examinations.
A total of 314 target lesions were measured and reported from the baseline examinations,
but only 113 (36%) of those were commented upon again during the subsequent examinations.
Conclusion
Our study revealed that radiologists at an NCI-designated cancer center failedto consistently report on the same lesions in serial examinations which hinders the performance of RECIST and other forms of tumor response assessment.
Radiologists frequently reported a set of lesions on baseline examinations,
but different radiologists reporting on subsequent examinations described different sets of findings that did not correlate directly with those in the baseline examinations.
Potential solutions to this problem of discontinuity in radiology reporting include the following:
Educating radiologists about the importance and...
Personal information
David J.
Vining,
MD,
is a Professor of Diagnostic Radiology at the University of Texas MD Anderson Cancer Center in Houston,
Texas,
where he also serves as the Medical Director of the Image Processing and Visualization Laboratory.
Email:
[email protected]
References
Miller A,
Hoogstraten B,
Staquet M,
et al.
Reporting results of cancer treatment.
Cancer.
Jan 1,
1981;47(1):207–214.
Therasse P,
Arbuck SG,
Eisenhauer EA,
et al.
New guidelines to evaluate the response to treatment in solid tumors (RECIST Guidelines).
J Natl Cancer Inst 2000;92:205–216.
Eisenhauer E,
Therasse P,
Bogaerts J.,
et al.
New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1).
Eur J Cancer.
Jan.2009;45(2):228-247.
Sketching a new reality: What will the radiology report of the future look like? http://www.nxtbook.com/nxtbooks/acr/acrbulletin_201203/index.php?startid=14.
Accessed January 6,...