Learning objectives
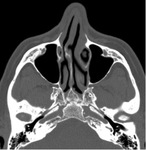
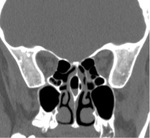
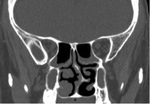
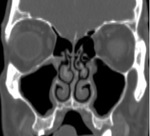
In this exhibit we will discuss the role of multidetector computed tomography (MDCT) in the evaluation of anatomical variations of the paranasal sinuses,
focusing on the main findings radiologists should bring to the attention of clinicians for their potential correlation with pathological conditions.
Background
The nasal cavity and paranasal sinuses constitute an anatomical and functional unit covered by the same mucosa.
They communicate via small openings and narrow ducts that allow both aeration and sinus drainage.
Paranasal sinuses develop in a certain sense as "diverticula of the nose”.
Pneumatization is preceded by the formation of "yellow bone marrow" and then by fluid-like content.
The lack of pneumatization is normal before 1 year.
At birth,
maxillary and ethmoid sinuses may contain a little amount of air; the sphenoid sinus pneumatizes...
Findings and procedure details
PROCEDURE DETAILS
CT has replaced conventional radiographs in recent years for the high-resolution sectional images less than 1 mm thick obtained out within a few seconds.
Additionally,
the primary scans provide data sets for the computer generation of reconstructed image planes called multiplanar reconstructions (MPRs),
without subjecting the patient to additional radiation exposure and with the advantage of the elimination of metallic artifacts.
Axial slices can thus be supplemented by coronal and sagittal image planes for a better understanding of regional anatomy.
This is particularly...
Conclusion
There is a wide variability of the MDCT appearance of the paranasal sinuses anatomy.
In this setting,
radiologists should get familiar with MDCT imaging findings to give clinicians the right advice in order to avoid therapeutic failure and/or iatrogenic complications.
References
1. Pérez-Piñas,Sabaté J,Carmona A,Catalina-Herrera CJ,Jiménez-Castellanos J.
Anatomicalvariationsin thehumanparanasal sinusregionstudiedbyCT.
J Anat.
2000 Aug;197 (Pt 2):221-7.
2. Kantarci M,Karasen RM,Alper F,Onbas O,Okur A,Karaman A.
Remarkableanatomicvariationsinparanasalsinusregionand theirclinicalimportance.
Eur J Radiol.2004 Jun;50(3):296-302.
3. Bayram M,Sirikci A,Bayazit YA.
Importantanatomicvariationsof the sinonasal anatomy in light of endoscopic surgery: apictorial review.
Eur Radiol.
2001;11(10):1991-7
4. Leunig A,Sommer B,Betz CS,Sommer F.
Surgicalanatomyof thefrontalrecess--is there abenefitinmultiplanarCT reconstruction? Rhinology.2008 Sep;46(3): 188-94.
5. Becker SS,O'Malley BB.
Evaluationof sinus computed tomography scans: a collaborative approach between radiology and otolaryngology.
Curr Opin Otolaryngol Head Neck Surg.2013 Feb;21(1):69-73....