Learning objectives
Infiltrative cardiomyopathy is a generic term for cardiac related conditions such as myocarditis,
amyloidosis,
sarcoidosis,
haemochromatosis,
iron overload cardiomyopathy and Fabry disease.
Cardiac MR (CMR) offers non-invasive assessment of biventricular function,
myocardial odema or fibrosis and allows quantitative tissue mapping.
The characteristic features of each infiltrative cardiomyopathy are described in this educational exhibit.
Background
Infiltrative cardiomyopathies are a diverse group of cardiac diseases caused by the deposition of abnormal cells or substances within the myocardium.
CMR combines good spatial resolution,
lack of radiation,
non-invasiveness,
and three-dimensional imaging with highly reproducible measurements of the ventricular function.
The CMR protocol used in cases of infiltrative cardiomyopathies includes a general basic set of imaging sequences (Fig. 1) with additional sequences depending on the specific type of clinically suspected cardiomyopathy.
Scout images allow the correct positioning of the heart at the center of...
Findings and procedure details
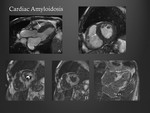
Cardiac amyloidosis
Disease related to the interstitial deposition of extracellular insoluble fibrillary proteins (amyloid) within the myocardium which leads to oxidative stress,
mechanical disruption,
and tissue damage.
It is classified into primary Amyloid Light chain (AL),
hereditary transthyretin-derived (ATTR),
senile systemic (SSA),
secondary (AA) amyloidosis [2].
AL is the most aggressive form and is caused by the deposition of immunoglobulin light chains secondary to an underlying plasma cell dyscrasia.
Cardiac involvement occurs in about 50% of cases (median survival as low as 4 months),
patients...
Conclusion
Imaging and diagnosis of infiltrative cardiomyopathies can be challenging.
Understanding the pathophysiology,
the classic features and differential diagnosis is crucial in the imaging of these conditions.
Personal information
Contact details:
Miss Rebecca Taylor
Specialist Radiographer.
Department of Radiology,
Royal Papworth NHS Foundation Trust,
Papworth Everard,
Cambridge,
CB23 3RE,
United Kingdom.
Email:
[email protected]
Mrs Tracy Horn
Lead MRI Radiographer.
Department of Radiology,
Royal Papworth NHS Foundation Trust,
Papworth Everard,
Cambridge,
CB23 3RE,
United Kingdom.
Email:
[email protected]
Dr Alessandro Ruggiero
Consultant Radiologist.
Department of Radiology,Royal Papworth NHS Foundation Trust,
Papworth Everard,
Cambridge,
CB23 3RE,
United Kingdom.
Email:
[email protected]
References
1.
Huber AM,Schoenberg SO,Hayes C,
Spannagl B,
Engelmann MG,
Franz WM,
et al.
Phase-sensitive inversion-recovery MR imaging in the detection of myocardial infarction.Radiology2005;237(3):854–860
2.
Kwong RY,Falk RH.Cardiovascular magnetic resonance in cardiac amyloidosis.Circulation2005;111(2):122–124
3.
Dispenzieri A,
Gertz MA,
Kyle RA,
Lacy MQ,
Burritt MF,
Therneau,
et al.
Serum cardiac troponins and N-terminal pro-brain natriuretic peptide: a staging system for primary systemic amyloidosis.
J Clin Oncol.
2004;22(18):3751–7
4.
Giesbrandt KJ,
Bolan CW,
Shapiro BP,
Edwards WD,
Mergo PJ.
Diffuse diseases of the myocardium: MRI-pathologic review of cardiomyopathies...