Learning objectives
The purpose of this essay is to help radiologists:
Review the main non-adenocarcinoma pancreatic lesions,
emphasizing an approach of key cross-sectional imaging features
Distinguish the different types ofneoplastic andnonneoplasticdisorders.
Discuss the management pancreatic lesions based on imaging pattern.
Background
Pancreas imaging assessment usually demonstrates diseases with typical features.
Non-adenocarcinoma disorders show a wide spectrum of imaging features,
ranging from a tumor-like anatomic variant to malignant disease.
In this scenery,
imaging plays a crucial role in the diagnosis and management of pancreatic lesions.
We selected illustrative cases that were collected and classified didactically according to patterns type.
For each case,
we provide clinical and radiology presentations,
differential diagnosis,
and teaching points.
We propose a classification of these cases as follows:
Cystic neoplasm
Serous cystic neoplasm...
Findings and procedure details
CYSTIC NEOPLASM
1.
Serous cystic neoplasm
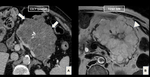
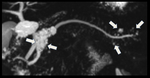
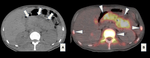
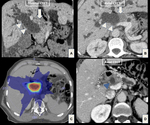
Case: Female patient (83 y.o.) asymptomatic (Fig. 1).
Teaching points:
Serous cystadenomas (SCA) are a benign condition in women (75% x 25%,
F:M)
Age: 6th-7th decades.
They are often diagnosed incidentally.
Slight predominance in the pancreatic head.
Composed of numerous small cysts (< 1 cm),
which are conjoined in a honeycomb-like pattern.
Tips⇒ fibrous portion may enhance after contrast injection (central scar) and central calcified areas may appear (stellate pattern).
CT:the appearance depends on the number of fibrous septa...
Conclusion
Pancreatic lesions have a broad spectrum of imaging findings and some of them may overlap.
Therefore,
the knowledge of relevant clinical informations and key imaging features are important to accurate characterization and differentiation of pancreatic lesions.
Personal information
Contact details:
Fernando Morbeck A.
Coelho
Department of Imaging,Diagnósticos da América S.A.
DASA.
São Paulo,
SP,
Brazil
Av.
República do Líbano,
725 - Moema
CEP 04501-000- São Paulo/SP,
Brazil.
Email:
[email protected]
Author Information:
Fernando Morbeck A.
Coelho (Diagnósticos da América S.A.
DASA.
São Paulo,
SP,
Brazil.
Department of Radiology,
University of São Paulo,
São Paulo,
SP,
Brazil)
References
Karoumpalis I,
Christodoulou DK.
Cystic lesions of the pancreas.
Ann Gastroenterol.
2016;29(2):155–61.
Kalb B,
Sarmiento JM,
Kooby D a,
Adsay NV,
Martin DR.
MR imaging of cystic lesions of the pancreas.
Radiographics.
2009;29(6):1749–65.
Zhang X-P,
Yu Z-X,
Zhao Y-P,
Dai M-H.
Current perspectives on pancreatic serous cystic neoplasms: Diagnosis,
management and beyond.
World J Gastrointest Surg [Internet].
2016;8(3):202.
Available from: http://www.wjgnet.com/1948-9366/full/v8/i3/202.htm
Sandrasegaran K,
Lin C,
Akisik FM,
Tann M.
State-of-the-art pancreatic MRI.
Am J Roentgenol.
2010;195(1):42–53.
Tanaka M,
Fernández-del Castillo C,
Kamisawa T,
Jang JY,...