Learning objectives
To review characteristics,
physiopathology and epidemiologic details of small bowel diverticulosis.
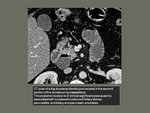
To describe imaging techniques used in diagnosis of small bowel diverticulosis and evaluation of acute complications.
To describe and illustrate radiological features of uncomplicated and complicated diverticula.
Background
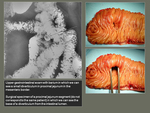
A diverticulum is a sacular protrusion of the mucosa through the muscular intestinal wall in any portion of the gastrointestinal tract.
The presence of multiple diverticula is called diverticulosis.
These herniations occur in weakened points of the intestinal wall where the vascular structures enter into the muscle layer.
Except the Meckel´s diverticulum,
unique true diverticulum composed of all of the intestine´s layers,
the rest are false diverticula o pseudodiverticula,
composed of mucosa and submucosa covered of serosa.
Small intestine diverticular disease is much less common...
Findings and procedure details
ETIOLOGY
The cause of this condition is unknown.
It is believed that the diverticula develop as the result of abnormalities in peristalsis,
intestinal dyskinesis and high segmental intraluminal pressures.
Risk factors related with small bowel diverticulosis is low-fiber and high-fat diet,
advanced age,
systemic sclerosis,
visceral myopathy and neuropathy.
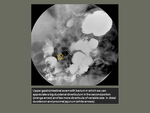
The diverticula emerge on the mesenteric border of the small bowel,
in weakened points of the intestinal wall where mesenteric vessels penetrate in the muscular layer.
Fig. 1
EPIDEMIOLOGY
The real incidence is unknown because they...
Conclusion
Diagnosis of small bowel diverticulosis is difficult and is often missed or delayed although is quite frequent entity (about 5%).
Complicated small bowel diverticulosis can present as acute abdominal pain and should always be considered in the differential diagnosis of acute abdominal findings on examination or cross-sectional imaging.
Personal information
Authors would like to thank the contribution of the Service of Surgery,
notably Dr.
García-Ureña,
head of Service of Hospital Universitario del Henares.