Learning objectives
The hip evaluation scheme is based on a series of specific tests,
which must be performed on the basis of the anamnesis,
for a complete evaluation of its functionality,
the integrity of the tendons,
muscles,
joint capsule,
nerve structuresand of the remaining soft tissues.
The present work aims to provide the Radiologist with the essential tools for a quick and accurate clinical diagnosis,
to be associated with dynamic ultrasound imaging.
Background
Hip is a complex system,
and the understanding of its biomechanics and its pathological changes is fundamental for a correct interpretation of ultrasound imaging.
Findings and procedure details
CLINICAL "FLOW-CHART"
The clinical "flowchart" consists of a series of tests for the evaluation of: coxo-femoral joint motility,
integrity of tendon (degenerative tendinopathies,
inflammatory pathologies,
traumatic injuries) and muscles fibers (traumatic and non-traumatic lesions),
nerve structures integrity,
and the presence of bursitis (iliopsoas and trochanteric bursitis).
COXO-FEMURAL JOINT MOTILITY
Range of motion (ROM)
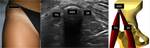
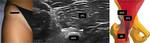
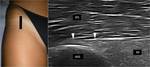
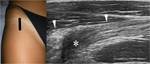
The hip is evaluated firstly in a 90° flexed position,
followed by internal rotation,
external rotation and extension manouvers (Fig.1-4).
Femoro-acetabular impingement (FAI)
FAI is defined as the outcome of a series...
Conclusion
The integrated clinical-instrumental approach is a valuable tool in the hands of the Radiologist and allows him to interact with other Specialists in a more appropriate way.
References
Musculoskeletal Ultrasound Technical Guidelines - IV Hip,
European Society of MusculoSkeletal Radiology.
E.
Silvestri et al.
(2015),
Ultrasound Anatomy of Lower Limb Muscles: A Practical Guide,
Springer International Publishing Switzerland
McNally EG (2014),
Practical musculoskeletal ultrasound - 2nd edition.
Elsevier,
Philadelphia
O’Neill J (2008),
Musculoskeletal ultrasound: anatomy and technique.
Springer,
New York
Martinoli C,
Bianchi S (2007),
Ultrasound of the musculo-skeletal system.
Springer,
New York
Martinoli C.
Musculoskeletal ultrasound: technical guidelines.
Insights Imaging 2010;1(3):99–141.
Michael P Reiman,Richard C Mather III,Chad E Cook,
Physical examination tests...