Learning objectives
To describe the mechanisms of abusive head trauma.
To review the use and clinical indications of the neuroimaging techniques for the diagnosis of abusive head trauma.
To describe the typical and atypical manifestations of abusive head injury
Background
AHT is the leading cause of fatal head injuries in children younger than 2 years and is responsible for 53% of serious or fatal traumatic brain injury cases. AHT fatality rates are more than 20%.
These patients often develop severely impairing sequelae that include developmental delays,
seizures,
para- or tetraplegia,
ventilation dependence,
deafness,
blindness,
or behavioral abnormalities.
Outcomes are shown to be worse in patients with AHT than in those with accidental trauma.
Although these numbers likely underrepresent the true incidence,
however,
because of the...
Findings and procedure details
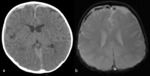
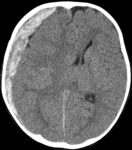
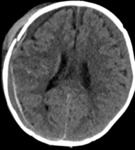
In most institutions unenhanced CT is the initial examination for children with suspected AHT.
Initial CT should include soft tissue and bone settings.
Volume-rendered CT images and multiplanar reformatting can increase the conspicuity of subtle fracture lines.
CT of the head should be performed in all children who present signs of abuse in combination with signs of possible neurotrauma or intraocular haemorrhages.
MRI is not the first imaging tool in AHT.
The most important reason is a lower sensitivity for acute haemorrhage compared to CT....
Conclusion
AHT is the current most appropriate and inclusive diagnostic term for infants and young children who suffer from inflicted intracranial and spinal injuries.
No single lesion is diagnostic of AHT.
Rather,
the multiplicity of findings,
including evidence of intracranial and spinal involvement,
complex retinal hemorrhages,
ribs and other fractures incompatible with the mechanism of trauma provided,
as well as the severity and age of the findings,
provide clues to the diagnosis.
The radiologist plays an important role in the detection and diagnosis of AHT due...
References
1.1.Choudhary AK,
Servaes S,
Slovis TL,
Palusci VJ,
Hedlund GL,
Narang Sk,
et al.
Consensus statement on abusive head trauma in infants and young children.
Pediatric Radiology https://doi.org/10.1007/s00247-018-4149-1.
2.
2.
Shaahinfar A,
Whitelaw KD,
Mansour KM.
Update on abusive head trauma.
Curr Opin Pediatr 2015,
27:308–314.
DOI:10.1097/MOP.0000000000000207
3 3.
Greeley CS.
Abusive Head Trauma: A Review of the Evidence Base.
AJR 2015; 204:967–973.
DOI:10.2214/AJR.14.14191.
4.
Wright JN.
CNS Injuries in Abusive Head Trauma.
AJR 2017; 208:991–1001.
DOI:10.2214/AJR.16.1760
5.
Kemp AM.
Abusive head trauma: recognition and...