Learning objectives
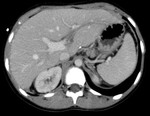
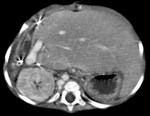
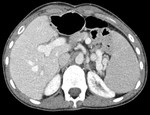
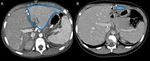
The objective of this pictorial essay is to describe and illustrate the role of imaging in detecting early and late complications after pediatric liver transplantation (LT) and their possible percutaneous treatments using a case series collected in our institution (Radiology Unit - Department of Medicine - University Hospital of Padova).
Background
Liver transplantation (LT) represents the treatment of choice in end-stage liver disease; the main indications [1,
5] are:
cholestatic diseases: biliary atresia (about 46% of all pediatric LTs),
Alagille syndrome,
sclerosing cholangitis,
Caroli disease,
etc.
metabolic diseases: maple syrup urine disease,
α1-antitripsin deficiency,
tyrosinemia,
Wilson's disease,
etc.
liver tumors: hepatoblastoma,
hemangioendothelioma
acute liver failure (very rare in children).
Surgical techniques [1,
3]:
whole-LT: performed as in adults,
with classic (inferior vena cava replacement) or piggyback (preservation of the native inferior vena cava) technique;
reduced size-LT:...
Findings and procedure details
Imaging modalities [2,
5,
6]:
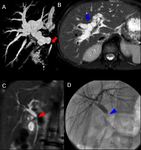
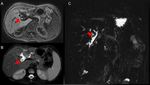
- US/DopplerUS is the first imaging modality for the evaluation of liver graft dysfunction in vascular as well as in biliary complications;
- MR is a problem solving modality,
especially thanks to its angiographic and cholangiographic sequences and the lack of ionizing radiations;
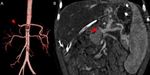
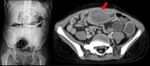
- CT is the imaging technique of choice in emergency,
it can also be used as a guide to percutaneous aspiration and fluid collection drainage;
- interventional radiology techniques allow the detection and treatment of vascular and...
Conclusion
Complications are frequent after pediatric LT [1].
Biliary complications are the most frequent,
while vascular complications are the most dangerous for graft survival [2].
The early detection of post-operative complications allows their prompt treatment,
avoiding graft failure and improving patient survival [1,
2,
5].
Different imaging modalities help in the detection of early and late complications of LT,
as well as in long-term follow-up to assess transplant viability [1,
4].
Interventional radiology has an increasing role in the management of postoperative complications [4].
Personal information
Annachiara Cavaliere,MD,Radiology resident
Silvia Karem Janet Flores Quispe, MD,Radiology resident
Alessia Varotto,
MD,Radiology resident
Caterina Dengo,
MD,
Radiology resident
Veronica De Lorenzo,
MD,
Radiology resident
Caterina Zivelonghi,
MD,
Radiology resident
Monica Zuliani,
MD,
Radiologist
Tiziana Toffolutti,
MD,
Radiologist
Roberto Stramare,
Professor,
Radiologist
Radiology Uniti - Departement of Medicine - University of Padova
Via N.
Giustiniani,
2 - 35128,
Padova - Italy
[email protected]
[email protected]
References
Spada M,
Riva S,
Maggiore G,
Cintorino D,
Gridelli B,
Pediatric liver transplantation.
World Gastroenterol 2009; 15(6): 648-674
Berrocal T, Parròn M, A’lvarez-Luque A,
Prieto C,
Lòpez Santamarìa M.
Pediatric Liver Transplantation: A Pictorial Essay of Early and Late Complications. Radiographics,
2006 Jul-Aug:26(4):1187-209.
Broelsch CE,
Emond JC,
Whitington PF,
Thistlethwaite JR,
Baker AL,
Lichtor JL.
Application of reduced-size liver transplants as split grafts,
auxiliary orthotopic grafts,
and living related segmental transplants. Ann Surg.
1990 Sep;212(3):368-75.
Miraglia R,
Maruzzelli L,
Caruso S,
Marrone G,
Carollo V,...