Learning objectives
Understand the imaging findings in both quiescent and recurrent Paget’s disease
Review the radiographic features in recrudescence of Paget’s and how to differentiate this from osteomyelitis
Background
Paget’s disease (osteitis deformans) is a common,
chronic condition characterised by abnormal and excessive bone remodelling.
Over the age of 40 it is reported to affect 3-4% of the population,
rising to approximately 10% over the age of 801. Given this background incidence it is not uncommon for a surgical patient to be diagnosed with Paget’s as an unrelated co-morbidity.
Post-traumatic postoperative osteolysis is a rare but recognised feature in the recrudescence of osteitis deformans,
whereby previously quiescent Paget’s is seen to recur following an...
Imaging findings OR Procedure Details
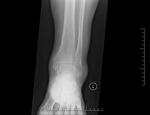
Three phases are classically described in Paget’s disease:
1) Lytic (incipient active) - active phase in which osteoclastic activity dominates
2) Mixed (active)- osteoblastic activity occurs alongside osteoclasts
3) Sclerotic (late inactive)- results in disorganised,
thickened bone
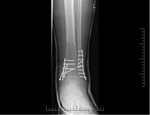
Recrudescence of Paget’s can be seen in the post-operative setting,
where a patient with a history of stable disease has a non-related surgical intervention.
This will typically involve the insertion of metalwork,
commonly post trauma or arthroplasty.
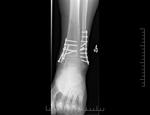
The findings of a rapid,
new postoperative osteolysis can be alarming...
Conclusion
Recognition of this rare but important entity is essential to avoid the potential misdiagnosis of postoperative infection,
which can lead to significant and adverse changes to clinical management.
References
1.
Smith SE et-al.
From the archives of the AFIP.
Radiologic spectrum of Paget disease of bone and its complications with pathologic correlation.
Radiographics.
22 (5): 1191-216.
2.
Lawrence GD et-al.
Immobilization hypercalcemia.
Some new aspects of diagnosis and treatment.
J Bone Joint Surg Am.
1973;55:87-94.
3.
Khurjekar KS et-al.
Spontaneous rapid osteolysis in Paget’s disease after internal fixation of subtrochanteric femoral fracture.
Singapore Med J.
2006;47:897-900.