Learning objectives
To familiarize the radiologist with a spectrum of radiographic manifestations of “Langerhans cell histiocytosis" (LCH),
on radiography,
computed tomography (CT) or magnetic resonance imaging.
Background
•LCH is a rare disorder of unknown etiology.
•Appears in childhood and early adulthood and is attributed to abnormal proliferation of histiocytes in various tissues.
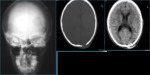
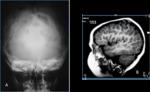
•Bone involvement is common; a wide spectrum of imaging appearances may be seen ranging from a typical solitary osteolytic lesion of the skull to a permeative abnormality of the long bones that imitates a Ewing sarcoma or osteomyelitis.
•Imaging is based predominantly on radiography.
•Computed tomography (CT) or magnetic resonance imaging (MRI) can assess the degree of trabecular andcortical bone...
Imaging findings OR Procedure Details
•From the Archives of our Department we reviewed the imaging studies (X-ray,
MRI and/or CT ) of twelve patients,
aged from 2 to 26 yrs,
with histologically proven LCH.
•Nine patients received chemotherapy and three patients underwent intralesional injection of corticosteroid.
Repeat imaging studies were available in eight patients.
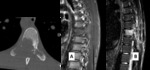
•Involvement of flat bones (cranial vault and ileum) was seen in four patients; spinal involvement was seen in five patients whereas long bone involvement was found in two patients.
Conclusion
Histiocytosis,
though rare,
should be considered in the differential diagnosis of lytic bone lesions presented either with discrete margins or with a permeative pattern of bone destruction,
in children,
adolescents and young adults.
Radiographic features are variable,
from a suggestive appearance to a more aggressive one,
which may mimic malignancy.
The final diagnosis should be confirmed on histology.
References
Normal 0 false false false EL X-NONE X-NONE
Abu‑Bonsrah N,
Goodwin CR,
Crane GM,
Abiola G,
Sciubba DM (2016) Langerhans cell histiocytosis of the cervical spine.
Spine J 16(1).
Azouz EM,
Saigal G,
Rodriguez MM,
Podda A (2005) Langerhans’ cell histiocytosis: pathology,
imaging and treatment of skeletal involvement.
Pediatr Radiol 35(2):103–115.
Bavbek M,
Atalay B,
Altinors N,
Caner H (2004) Spontaneous resolution of lumbar vertebral eosinophilic granuloma.
Acta Neurochir (Wien) 146(2):165–
Beltran J,
Aparisi F,
Bonmati LM,
Rosenberg ZS,
Present D,
Steiner GC (1993) Eosinophilic...