Learning objectives
Intra-osseous lesions of the patella are rare and there is little published literature.
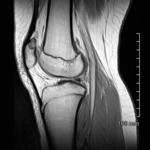
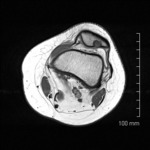
We describe MRI features of the most common patellar tumours and tumour-like lesionsalong with theirhistopathological diagnoses.
Background
The patella is an uncommon location for tumours.
It is involved in 1 to 4 out of 1000 cases of bone tumours.
Intra-osseous lesions of the patella present with non-specific symptoms such as pain,
swelling,
reduced range of movement,
mass or pathological fracture.
A tumourous condition should be suspected in cases with resistant night pain.
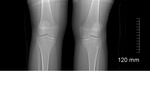
Pre-operative diagnosis is often difficult because radiographs only allow evaluation of aggressiveness and not the histological diagnosis.
Imaging with the use of CT and MRI plays an important part in...
Imaging findings OR Procedure Details
All cases of tumours and tumour-like lesions of the patella diagnosed in the department of Radiology at the Royal National Orthopaedic Hospital between 2008 and 2015 were reviewed.
The clinical and surgical records,
radiological findings and histopatholgy of 10 cases with 11 patellar lesions were reviewed.
There were 5 male and 5 female patients with age range 14 to 68 years.
The presenting symptom was knee pain in all cases.
The most common patellar intraosseous lesion in our series were benign tumours (4 cases).The most...
Conclusion
MRI imaging features,
in conjunction with other radiographic features on plain radiographs or CT,
may help narrow the differential of tumours and tumour-like lesions of the patella.
Imaging may obviate the need for tissue diagnosis in some cases.If there is a suspicion of malignancy,
histological diagnosis should be obtained before definitive treatment.
References
1.
Primary tumors of the patella.
Song M,
Zhang Z,
Ma K,
Lu M.
World Journal of Surgical Oncology (2015) 13:163
2.
Tumours of the patella.
Mercuri M,
Casadei R,
Ferraro A,
Cristofaro R,
Balladelli A,
Picci P.
International Orthopaedics (1991) 15:115-120.
3.
Tumours and tumour-like lesions of the patella: A report of eight cases.
Saglik Y,
Yildiz Y,
Basarir K,
Guner D.
Acta Orthop.Belg.,2008,74,391-396.
4.
Giant cell tumour of the patella:An uncommon cause of anterior knee pain.
Shibata T,
Matsunaga T,
Aoki M,
Iwasaki...
Personal Information
Dr Alok Arya
Musculoskeletal Radiology Fellow,
Royal National Orthopaedic Hospital,
Stanmore,
London
United Kingdom
Dr Philippa Tyler
Consultant Radiologist
Royal National Orthopaedic Hospital,
Stanmore,
London
United Kingdom