Learning objectives
To review the normal anatomy of the ankle and mid-foot ligaments.
To review the ultrasound and MRI techniqueof ankle and mid-foot ligaments.
To correlate the anatomy andthe ultrasound and MRI appearance of these ligaments.
The following ligaments are included in this pictorial essay:
Ankle ligaments: Tibiofibular ligaments,
Bassett ligament,
Anterior talofibular ligament,
Calcaneofibular ligament,
Lateral talocalcaneal ligament,
Medial ligament complex.
Chopart ligaments: Bifurcate ligament,
talonavicular ligament and plantar ligament.
Lisfranc ligaments.
Sinus tarsi ligaments.
Background
Ankle and mid-foot ligaments play an important role in providing stability to the respective joints that they bind.
Injuries of the ankle and foot can disrupt these structures and cause acute and chronic instability of the corresponding joints.
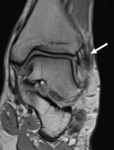
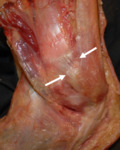
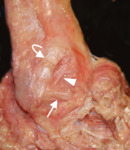
The anatomy of the ligaments around the ankle and foot is quite complex.A detailed knowledge of normal anatomy of these ligaments and their appearance on ultrasound and MRI can be useful in correct diagnosis of traumatic and non-traumatic ligamentous abnormalities.
Imaging findings OR Procedure Details
We have describedthe ligaments systematically on the basis of the joints they stabilize.
Special anatomic features of these ligaments have been emphasized and illustrated with the help of images,
wherever applicable.
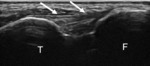
General US features of ankle ligaments:
Ankle ligaments are basically bundles of collagen fibres.
In general,
on ultrasound images they appear as echogenic fibrillar structures similar to those elsewhwere in the body.
Any deviations from this appearance has been mentionedduring the description of the respective ligament.
The ultrasound beam should be as perpendcular as...
Conclusion
Understanding the normal anatomy and normal US and MR imaging features of the ligaments of the ankle and midfoot joint is crucial to accurate diagnosis of pathologies involving these ligaments.
This pictorial essay correlating the anatomical,
US and MR images of normal ankle and midfoot joints ligaments is directed towards serving this purpose.
References
A Few References:
Golano P,
Vega J,
de Leeuw PAJ,
Malagelada F,
Manzanares MC,
GotzensV,
Van Dijk CN.
Anatomy of the ankle ligaments: a pictorial essay.
Knee Surg Sports Traumatol Arthrosoc 2010; 18: 557-569
Sconfienza LM,
orlandi D,
lacelli F,
Serafini G,
Silvestri E.
Dynamic high-resolution US of ankle and midfoot ligament: normal anatomic structure and imaging technique.
Radiographics 2015; 35: 164-78
Precerutti M,
Bonardi M,
Ferrozzi G,
Draghi F.
Sonographic anatomy of the ankle.
J Ultrasound 2013; 17: 79-87
Mengiardi B,
Pinto C,
Zanetti...
Personal Information
Thank you for viewing our exhibit.
We hope you liked it.
For any questions feel free to mail:
[email protected]