Learning objectives
To describe the anatomy of the sacroiliac joints (SIJ)
To learn the inflammatory or structural lesions found in spondyloarthritis and how to differentiate them from mecanical lesions
To identify other processes that may simulate spondyloarthritis (SpA).
Background
In 2009 the criteria for axial SpA were stablished,
giving rise to a high demand od sacroiliac joint studies Fig. 1 .
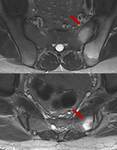
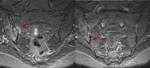
Bone Marrow Edema (BME) was stablished as the hallmark of sacroiliitis,is a marker of inflammation and needs to be significant in degree before a diagnosis of sacroiliitis can be made.
BME needs to be visible on at least two contiguous MR images,
or at two separate locations on the same image before it can be considered significant.
The recognition of inflammatory-type low back...
Imaging findings OR Procedure Details
Anatomy andBiomechanics
The main portion of the SIJ joint is surrounded by a complex capsule and lined with cartilage (diarthrosis).
Its shape is auricular,
and ‘opens’ posteriorly.
The sacrum and ilia have an extracapsular,
dorsally located articulation (synarthrosis),
which is augmented by vastligaments that provides internal stability.
If the sacroiliac joint is craniocaudally divided into thirds,
it is widely admited that all of the inferior one-third is a true synovial-cartilaginous joint.
The posterior part of the middle one-third is syndesmotic while the anterior part is...
Conclusion
-BME is common to both inflammatory and non inflammatory conditions.
-SIJ edema is common in asymptomatic patiens and should not be misinterpreted as inflammatory.
-It is important for radiologist to be familar with the anatomy and biomechanics of the SIJ to make the right diagnosis.
- Lesion distribution is key when dealing with small BME foci especially in young active individuals since middle and upper third is a weight bearing area and highly susceptible to mechanical damage.
-The associated findings (erosions being,
by far,
the...
References
1.-A.
Vleeming,
M.
D.
Schuenke,
A.
T.
Masi,
J.
E.
Carreiro,
L.
Danneels,
and F.
H.
Willard,
“The sacroiliac joint: An overview of its anatomy,
function and potential clinical implications,”Journal of Anatomy,
vol.
221,
no.
6,
pp.
537–567,
2012.
2.-Tsoi C,Griffith JF,Lee RKL,Wong PCH,Tam LS.Imaging of sacroiliitis: Current status,
limitations and pitfalls.Quant Imaging Med Surg.2019 Feb;9(2):318-335.
3.-Berthelot JM,
le Goff B,
Maugars Y,
Laredo JD.
Sacroiliac joint edema by MRI: Far more often mechanical than inflammatory? Joint Bone Spine 2016;83:3-5
4.-Berthelot JM,
Le Goff B,...
Personal Information
HU Basurto.
Bilbao.
Spain