Learning objectives
Illustrate regular anatomy and US appearence of the common peroneal nerve and its two terminal branch: deep peroneal nerve and superficial peroneal nerve.
Describe a correct and systematic technique for US evaluation of these structures.
Produce anatomical schemes with didactic purpose and show correlation with US imaging.
Background
Ultrasonography (US) is an established method for peripheral nerves imaging.
In the short axis,
the nerve has a honeycomb-like appearance,
with multiple rounded hypoechoic areas in a homogeneous hyperechoic background.
In the long axis,
it has a striated appearance composed of multiple parallel hypoechoic and hyperechoic bands.
This image resembles that of an electric cable.
This type of US appearance can be defined as fascicular structure.
The transverse image (short axis) is much more frequently used in clinical practice,
as it allows for the nerve...
Imaging findings OR Procedure Details
We will provide,
for each of these structures,
a dedicated US image compared with a detailed anatomic scheme,
and a practical guide on “how we do” a US scan of commonperoneal nerve,
deep peroneal nerve and superficial peroneal nerve.
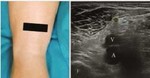
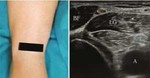
With the patient supine,
for the study of common peroneal nerve,
place the transducer in the transverse plane at the proximal popliteal fossa to visualize the distal part of the sciatic nerve,
which branches into the common peroneal nerve laterally and the tibial nerve medially.
(Fig2)...
Conclusion
US provides a quick,
dynamic and real time images for the evaluation of peripheral nerve,
with greater sensitivity than MRI.
In addition is very important the possibility to compare ultrasonography findings against the controlateral side.To carry out ultrasonography of peripheral nerve is essential to know the perfect anatomy of each nerve,
paying attention to anatomic landmarks and common sites of injury.
References
Bianchi S,
Martinoli C,
editors.
Ultrasound of the musculoskeletal system.
Milan,
Italy: Springer Verlag; 2009.
Chiou HJ,
Chou YH,
Chiou SY,
Liu JB,
Chang CY.
Peripheral nerve lesions: role of high-resolution US.
Radiographics.
2003;23:15.8.
Martinoli C.
Imaging of the peripheral nerves.
Semin Musculoskelet Radiol.
2010;14:461–2.
Peer S,
Kovacs P,
Harpf C,
Bodner G.
High-resolution sonography of lower extremity peripheral nerves: anatomic correlation and spectrum of disease.
J Ultrasound Med.
2002;21:315–22.