Learning objectives
The aim is to illustrate the anatomy and the sonographic aspect of the LFCN and to provide a systematic US-technique of study through anatomical schemes and ultrasound imaging
Background
LFCN is a small pure sensory nerve that arises from the L2 and L3 spinal nerve roots,
travels downward lateral to the psoas muscle,
and then crosses the iliacus muscle.
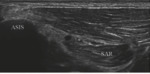
It emerges medially from anterior superior iliac spine (ASIS) below the inguinal ligament,
crosses the sartorius muscle.
(Fig.
1) LFCN has a variable course but,
this is the most common (about 30% cases).
It has a diameter of about 2 mm that become smaller when it passes through the fascia,
about 10 cm inferior to...
Imaging findings OR Procedure Details
A simple and systematic US-tecnique can improve the evalutation of this small nerve:
To patient supine,
should be identified via palpation the ASIS.
The end of the linear probe is applied perpendicular to the long axis of the limb,
at the ASIS bony landmark.
(Fig.
2)
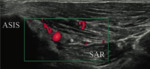
Move the probe in a trasversal plane 2-3 cm distal and medial to confirm the course of LFCN.
The nerve is located in the space between the two fascia layers (fascia lata and the fascia iliaca) above the sartorius...
Conclusion
LFCN is small nerve examinated with neurophysiological studies,
however often these are difficult to perform.
A standardizated and simple US-tecnique allow a morphological and structural valutation of the nerve and identify secondary causes of suffering.
Due to a high variability in the course of the nerve,
US also used in the treatment of meralgia paresthetica with higher success rate because it allow to visualize the nerve and the position of the needle during the procedure.
(Fig.
7-8)
References
Kele H.
Ultrasnography of the peripheral nervous system.
Pers Med.
2012;1:417-21.
Cheatham SW,
Kolber MJ,
Salamh PA.
Meralgia paresthetica: a review of the literature.
Int J Sports Phys Ther.
2013;8(6):883-93.
Ahmed A,
Arora D,
Kochhar AK.
Ultrasound-guided alcohol neurolysis of lateral femoral cutaneous nerve for intractable meralgia paresthetica: a case series.
Br J Pain.
2016;10(4):232.