Learning objectives
The purpose of our educational exhibit is to:
1.
Illustrate the normal anatomy and normal ultrasound (US) appearance of the saphenous nerve;
2.
Describe a systematic technique for US evaluation of such structure;
3.
Produce anatomical schemes with didactic purpose and show correlations with sonographic imaging
Background
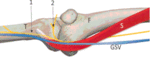
The saphenous nerve is the longest terminal branch of the posterior division of the femoral nerve and the only one below the knee that is not derived from the sciatic nerve.
After its origin in the femoural triangle,
it descends laterally to the femoral vessels and deep to the sartorius muscle to enter in the adductor or Hunter’s canal.
In the distal third of the adductor magnus muscle,
the saphenous nerve crosses over the femoral vessels to lie on their medial side and,
just above...
Imaging findings OR Procedure Details
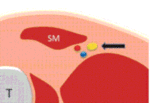
For the US examination of the saphenous nerve it is necessary to use transverse images (short axis) and apply the so-called elevator technique which consists of finding landmarks and ‘tracking it’ distally or prossimally.
In this way,
it is possible to assess the nerve as a small round hyperechoic structure,
visualize its surface area and the vasculature; the longitudinal view become important if an abnormality is seen.
A detailed ultrasound approach is:
1.
Place the transducer in a transverse plane at the middle third of...
Conclusion
US exam is a quick,
real-time and dynamic imaging and offers the possibility to compare the US findings against the contralateral side.
To perform ultrasonography of the saphenous nerve it is important to know the course,
paying attention to anatomic landmarks and common sites of injury and entrapment.
References
Bianchi S,
Martinoli C,
editors.
Ultrasound of the musculoskeletal system.
Milan,
Italy: Springer Verlag; 2009.
Gray H.
Anatomy descriptive and applied.
London: Longman’s,
Green and CO; 1935.
Mercer D,
Morrell NT,
Fitzpatrick J,
et al.
The course of the distal saphenous nerve: a cadaveric investigation and clinical implications.
Iowa Orthop J.
2011;31:231–5.