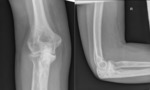
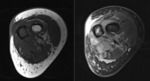
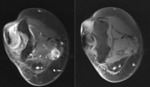
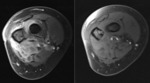
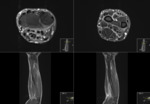
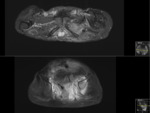
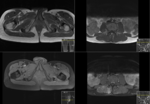
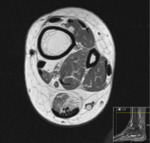
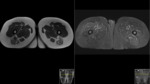
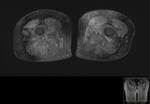
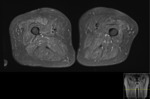
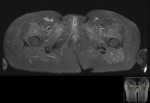
Purpose
Skeletal myositis is a rare condition.
It presents with muscle aches and pains,
progressive weakness and raised serum creatinine levels.
Implications can be debilitating and include renal failure,
recurrent falls,
declining independence levels,
recurrent infections and death.
Understanding the spectrum of conditions that can cause myositis is important for swift diagnosis,
management of patients to cure or delay disease progression,
improve outcomes and save lives.
Methods and Materials
309 consecutive patients who presented to our institution over a 3 year period between January 2015 & 2018,
with variable degrees of muscle weakness and pain were analysed.
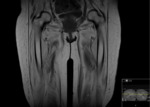
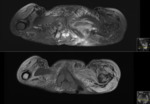
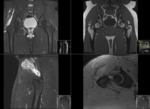
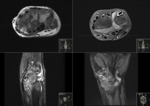
This included all imaging performed,
both at presentation and over a 3 year follow up period: MRI(+/- contrast),
US (including B-mode,
SMI,
Doppler,
power Doppler & elastography) plain radiographs,
CT,
DEXA,
& PET-CT.
Clinical,
histological,
serological and genetic results were correlated.
Results
All 309 patients were clinically managed in our institution,
a tertiary muscle disease unit.Causes for myositis based on our experience included:
-Autoimmune: Graft versus host disease,
Grave’s and Crohn’s disease.
-Infection: Bacterial,
fungal,
parasitic and viral.
Cases included HIV,
pyomyositis and necrotising fasciitis.
-Drug-induced:
1.
Recreational substance abuse such as cocaine or steroid
2.
Iatrogenic: Statins,
rituximab,
anti-retrovirals,
autoimmune therapy.
-Post traumatic: rhabdomyolysis,
myositis ossificans and haematomas of variable chronicity
-Nerve entrapments
-Demyelinating disease
-Neuromuscular inherited disorders such as Duchene muscle dystrophy
-Tumours: Myosarcoma,
lymphoma,...
Conclusion
Myositis can be a diagnostic enigma.
Accuracy and timely diagnosis is key to patient survival and improving outcomes.
Assessment of symmetry,
distribution,
progression as well as any relevant drug and clinical history is mandatory to analysing findings seen on imaging.
Multimodality imaging offers various ways of assessing the underlying structures,
including architectural,
vascular and functional changes.
Awareness of possible pitfalls (transient reactive changes,
associated avulsion injuries and mimics like eosinophilic fasciitis and postoperative changes,
technical artefacts,
inadequate imaging) provide means for overcoming or avoiding these....
References
1.Furst DE,
Amato AA,
Iorga SR,
Gajria K,
Fernandes AW.
Epidemiology of adult idiopathic inflammatory myopathies in a U.S.
managed care plan.Muscle Nerve.2012;45:676–683.
2.Martin N,
Li CK,
Wedderburn LR.
Juvenile dermatomyositis: new insights and new treatment strategies.Ther Adv Musculoskelet Dis.2012;4:41–50.
3.Salajegheh M,
Kong SK,
Pinkus JL,
et al.
Interferon-stimulated gene 15 (ISG15) conjugates proteins in dermatomyositis muscle with perifascicular atrophy.Ann Neurol.2010;67:53–63.
4.
WalczakBE,
JohnsonCN,
HoweBM.Myositis ossificans.
J Am Acad Orthop Surg.2015; 23:612–622.
5.Lilleker JB,
Vencovsky J,
Wang G,
et al.
The EuroMyositis registry: an international...
Personal Information
Dr Danoob Dalili
Specialist Registrar Clinical Radiology,
Imperial College London,
UK
Research fellow,
Guy's & St Thomas' NHS Foundation Trust,
London,
UK
Mr Mohit Bansal
Specialist Registrar Orthopaedic Surgeon,
Guy's & St Thomas' NHS Foundation Trust,
London,
UK
Dr Amanda Isaac
Consultant Musculoskeletal Radiologist,
Guy's & St Thomas' NHS Foundation Trust,
London,
UK
Hon Senior Clinical Lecturer,
Kings College London,
UK