Keywords:
Cardiac, CT, MR, Ablation procedures, Outcomes
Authors:
M. Salel1, H. Cochet2, F. Laurent2, M. Montaudon2, O. Corneloup2, V. Latrabe2, A.-A. Tassadit3, H. Nivet3, G. Chevreau3; 1Vigoulet-Auzil/FR, 2Pessac/FR, 3Bordeaux/FR
Methods and Materials
Population
Fifty-eight consecutive patients with sustained post-infarction ventricular tachycardia were included (54 men,
63±11 years).
Real-time image integration had been used in the 26 most recent patients (Group A),
but not in the previous 32 patients (Group B).
Imaging
All patients from group A underwent cardiac imaging with either MDCT (N=15),
MRI (N=3),
or both (N=8).
When using MDCT,
myocardial structural substrate was defined on contrast-enhanced first pass images as either wall thinning <5mm,
or myocardial hypodensity <0HU.
When using MRI,
myocardial structural substrate was defined on inversion-recovery prepared and respiratory navigated 3D gradient echo images as areas of enhancement >35% of maximum myocardial signal intensity.
Dedicated image post processing software (Music software,
IHU Liryc,
Bordeaux / Inria,
Sophia Antipolis,
France) was used to compute from the images 3D meshes of cardiac anatomy and myocardial structural substrate.
VT ablation procedure
In both group,
patients underwent endocardial contact mapping via either a trans-septal or a retrograde aortic approach, ± epicardial mapping via a subxyphoid approach.
Catheter ablation aimed at eliminating LAVA during sinus rhythm,
as well as any inducible VT.
The procedural endpoint was complete LAVA elimination and non-inducibility.
In group A,
image integration was performed after the acquisition of ventricular geometry,
and the substrate derived from imaging was used to focalize high-density mapping.
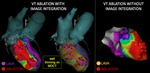
Procedures with and without image integration are illustrated in Figure 1.
Patients were followed at 1,
3,
6,
12 months over the first year,
and then every 6 months,
the primary endpoint being all-cause death or VT recurrence.
Statistical analysis
Baseline,
procedural and follow-up characteristics were compared between the 2 groups using parametric and non-parametric tests,
as appropriate.
Logistic regression was used to identify clinical characteristics associated with VT recurrence.
Event-free survival plots were made by the Kaplan-Meier method and compared with log-rank tests.
P < 0.05 indicated statistical significance.