Keywords:
Cardiac, MR, Biopsy, Contrast agent-other, Diagnostic procedure, Inflammation
Authors:
E. Gupalo, O. Stukalova, N. Mironova, T. Malkina, P. Chumachenko, S. K. Ternovoy; Moscow/RU
Methods and Materials
There were included 30 pts with conduction disturbances (CD) and structurally normal heart and 25 pts with clinical syndrome of dilated cardiomyopathy (DCMP).
Baseline charecteristics are presented in Table 1.
In DCMP pts coronary angiography excluded coronary artery disease.
For morphological evaluation endomyocardial biopsy (EMB) in all DCMP pts was performed.
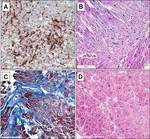
EMB confirmed active inflammation in 16 (64%) DCMP patients (Figure 1 A,B).
In 4(16%) pts EMB revealed resolved myocarditis with huge areas of fibrosis (Figure 1C).
In 5 cases (25%) the sighs of active inflammation were not detected and the morphological changes were determined as idiopathic DCMP (Figure 1D).
Table 1. Baseline clinical patient charecteristics
|
|
CD pts
(n= 30)
|
DCMP pts
(n = 25
|
|
Age,
years
|
40,7±11,4 |
39,5±11,3 |
|
Sex,
(mae %)
|
13 (43,3) |
12 (48) |
|
Duration of the disease
|
from 7 days |
15[9;54] months |
|
Heart failure,
functional class (NYHA)
|
0 |
2,4±1,44 |
| Echocardiography findings |
Left ventricular ejection fraction (%)
|
63,2±3,4 |
34,7±9,7% |
|
Left ventricular end diastolic diameter (sm)
|
4,8±0,46 |
7,3±1,3 |
|
Left ventricular end sistolic diameter (см)
|
3,5±0,54 |
5,5±1,5 |
|
Right ventricular dilatation – n (%)
|
- |
13 (52%) |
|
Systolic pulmonary artery pressure (mmHg)
|
25,7±2,3 |
35,0[21,5;50] |
| ECG data |
Atrioventricular block – n (%)
|
15 (50 %) |
4(16%) |
|
Left bundle branch block – n (%)
|
9 (30 %) |
11 |
|
Right bundle branch block – n (%)
|
6 (20 %) |
0 |
| Endomyocardial biopsy data |
Active myocarditis
|
- |
16 (64%) |
|
Resolved myocarditis with areas of fibrosis
|
- |
4 (16%) |
|
Idiopathic dilated cardiomyopathy
|
- |
5(25) |
| Therapy |
ACEi/BAR – n (%)
|
- |
23 (92%) |
|
Beta-blockers– n (%)
|
- |
20 (80%) |
|
Diuretics– n (%)
|
- |
18 (72%) |
|
Amiodarone – n (%)
|
- |
0 |
|
Digoxin – n (%)
|
- |
0 |
All pts underwent CMR with assessment of myocardial edema (ME),
early gadolinium enhancement (EGE) and late gadolinium enhancement (LGE).