The most common reaction of the pericardium against any aggression is the fluid production.
Other more infrequent reactions are thickening of their layers,
calcification,
nodules or masses.
1.- ANATOMY Fig.1
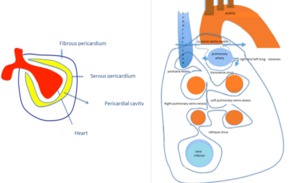
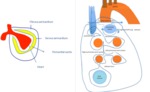
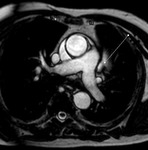
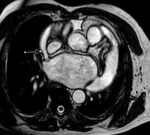
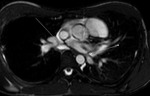
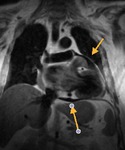
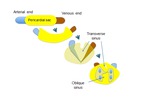
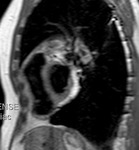
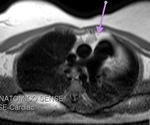
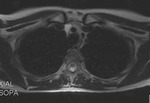
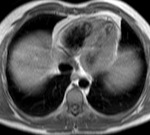
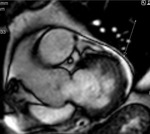
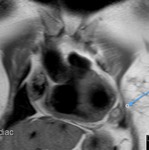
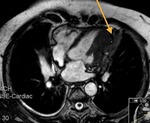
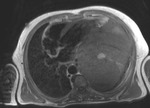
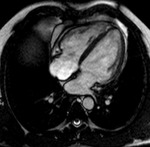
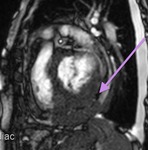
Fig. 1: a) The pericardium is formed by two layers, the fibrous outer layer and the inner serous layer, which folds on itself forming virtual pericardial cavity.
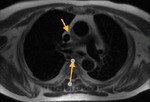
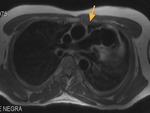
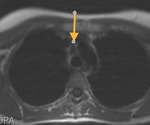
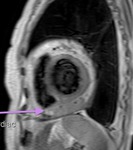
b)The transverse sinus is located behind the ascending aorta and pulmonary trunk and in front of the left atria and the superior vena cava.
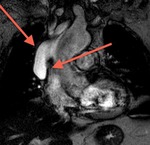
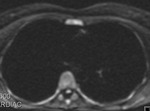
The oblique sinus is an inverted U-shaped pericardial reflection located behind the left atrium.Pericardial recesses are sacculations of the pericardial cavity
The pericardium is an anatomically simple structure that can be affected by multiple processes.
- The outer layer it is fibrous pericardium,
hard and fibrous,
that binds to the adyacent structures that anchor the heart:
- Joins the central tendon of the diaphragm by the pericardiophrenic ligament.
Fig.
2
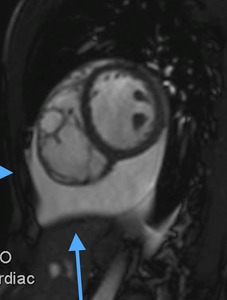
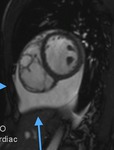
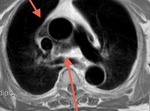
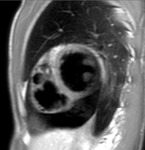
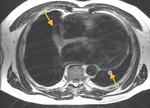
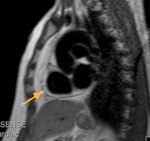
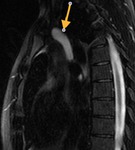
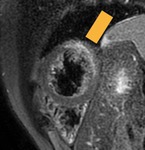
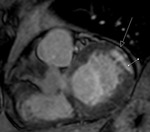
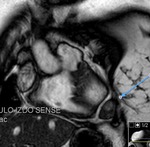
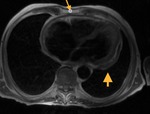
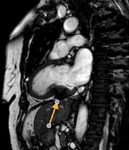
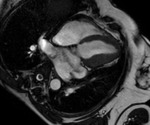
Fig. 2: Cine MR Image, short axis. Peripheral severe pericardial effusion. Trasudate hyperintense on T2-weighted image. The arrows indicate the anchors of the pericardium to the sternum and diaphragm
- On the front face it is inserted into the sternum by (highly variable) pericardiophrenic ligaments.
- On the back it is attached to the posterior mediastinum by loose fibrous connective tissue.
- It binds to the adventitia of large vessels.
The ascending aorta pulls the pericardium to the level of the sternal angle.
Fig.
3
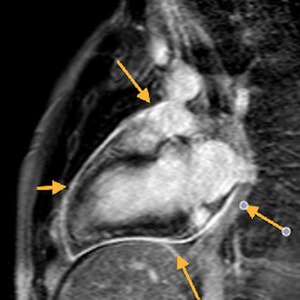
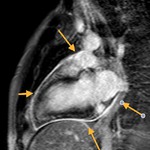
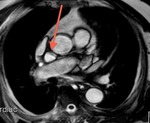
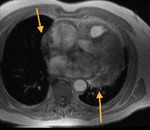
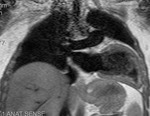
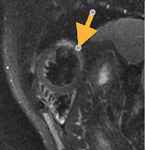
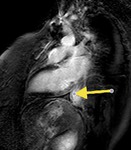
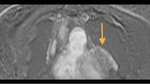
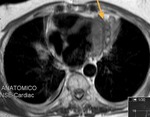
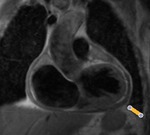
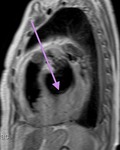
Fig. 3: Long axis of the left ventricle, viability sequence, after IV gadolinium administration . Pericardium diffuse uptake is observed . The upper extension of the pericardium on the aorta is identified . There were no signs of constriction .
The fibrous pericardium is very rigid and protects the heart from a sharp filling,
acts as a barrier to inflammation,
infection or tumors.
- The inner layer,
serous pericardium,
is essentially formed by mesothelium and has an outer parietal layer and inner visceral layer.
The parietal layer lines the inner surface of the fibrous pericardium to which it adheres,
whereas the visceral layer envelops the epicardial
surface of the heart,
separated from it only by a layer of epicardial fat that contains the coronary vessels.
Thus,
it forms a sack with two layers: visceral and parietal.
This bag contains a virtual space called the pericardial cavity,
containing a small liquid film which allows cardiac motion without friction.
Fig.
4
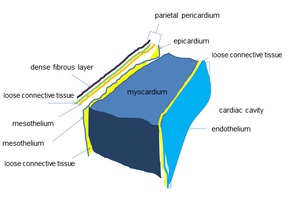
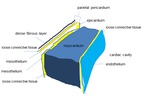
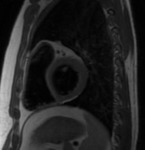
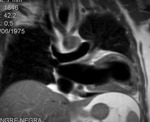
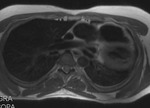
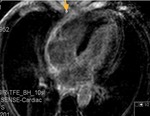
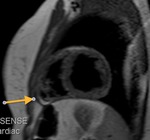
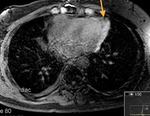
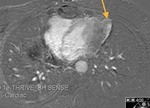
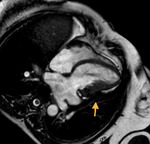
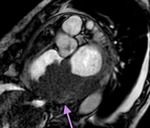
Fig. 4
The parietal layer of the serous pericardium is attached to the fibrous pericardium.
The visceral layer of the serous pericardium is attached to the heart and forms the epicardium.
The visceral serous pericardium is reflected forming two tubular structures,
the first from the heart and great vessels to continuous with the parietal pericardium at the root of the aorta and the main pulmonary artery,
and the second tubular structure how to enter the heart of the superior and inferior vena cava veins and pulmonary veins.
Fig.
1 and Fig.
3.
The transverse sinus is located behind the ascending aorta and pulmonary trunk and in front of the left atria and the superior vena cava.
The oblique sinus is an inverted U-shaped pericardial reflection located behind the left atrium.
Mediastinal fat helps identify the pericardium and pericardial recesses.
Pericardial recesses are sacculations of the pericardial cavity,
main recesses are:
• Superior aortic recess surrounds the aortic root,
except except at the level of the pulmonary artery.
It is divided into anterior,
right lateral,
between the superior vena cava and the aorta and posterior.
Fig.
5,
Fig.
6 and Fig.
7.
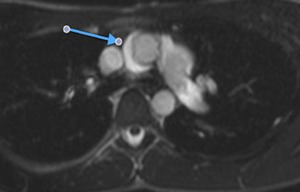
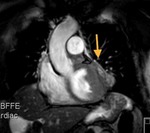
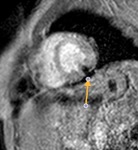
Fig. 5: STIR, axial . The arrow shows the superior aortic recess
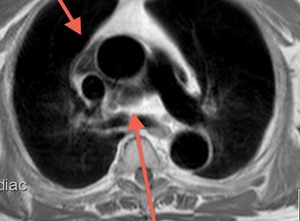
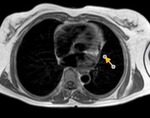
Fig. 6: Black-blood T1-weighted image, axial. Patient with cystic lesion isointense to fluid in all sequences located between the superior vena cava and the aorta. Superior aortic recess
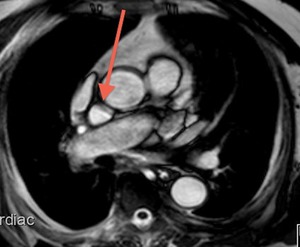
Fig. 7: Superior aortic recess between the superior vena cava and the aorta. Axial T2-weighted image.
• Right and left pulmonary artery recess Fig.
8 and Fig.
9.
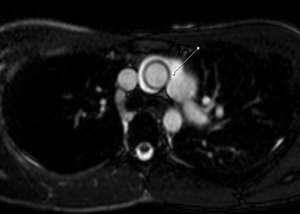
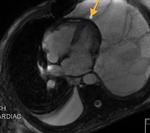
Fig. 8: Cine MR Image. Patient with epicardial efussion. The arrow points to the right pulmonary artery pericardial recess.
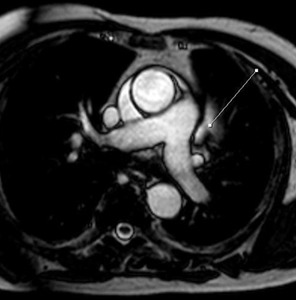
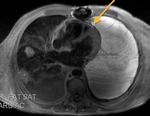
Fig. 9: Cine MR image, axial. The arrow points to the left pulmonary artery recess.
• Postcava recess.
Fig.
10.
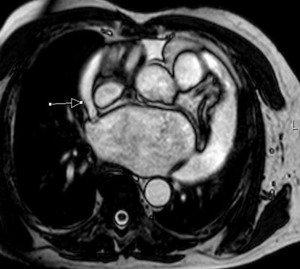
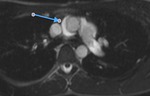
Fig. 10: Cine MR image. Patient with pericardial effusion. The line shows the recess of the superior vena cava.
• Right pulmonary veins recess.
Fig.
11.
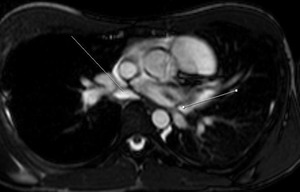
Fig. 11: Cine MR image in a patient with pericardial effusion. The lines indicate the recesses of right and left pericardial veins.
• Left pulmonary veins recess.
Fig.
12 and Fig.
13.
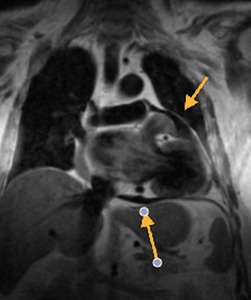
Fig. 12: Black blood T1-weighted, coronal. Hypointense pericardial effusion in T1. The upper arrow indicates the recess of the left pulmonary veins.
• Transverse sinus.
Fig.
13.
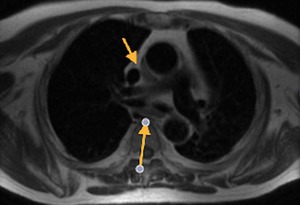
Fig. 13: Black blood T1-weighted, axial. Anterior arrow points to the superior aortic recess. Posterior arrow indicates the transverse sinus.
• Oblique sinus.
Fig.1.
Knowledge of these recesses and sinuses is essential to avoid misinterpreting these normal structures as lymph nodes,
mediastinal masses or dissection.
The main irrigation is through the pericardiacophrenic artery,
it is a long slender branch of the internal thoracic artery.
Other arterial branches are:
- Musculophrenic artery,
terminal branch of the internal thoracic artery.
- Bronchial,
esophageal and superior phrenic,
branches of the thoracic aorta
- Coronary arteries: Visceral pericardium is supplied by coronary arteries (only the visceral layer).
The venous drainage:
-Pericardiacophrenic veins tributaries of the brachiocephalic veins or internal thoracic.
- Tributaries to the azigos venous systems
The innervation is:
-Sensitive: phrenic nerves.
The painful sensation is often in the ipsilateral supraclavicular region of the skin.
-Vagus nerves.
-Vasomotor sympathetic trunks.
Lymphatic drainage is through mediastinal lymph.
The pericardium serves various functions:
- It fixes the position of the heart within the mediastinum.
- Decreases the friction of cardiac movements,
and limits the spread of diseases to the heart from adjacent structures.
- Respiratory variations of intrathoracic pressure are transmitted to the pericardial cavity and subsequently to the cardiac chambers and are more pronounced on the thin-walled right ventricle.
Atrial filling is supported by the negative systolic pericardial pressure.
The pericardium limits the acute cardiac chamber dilatation during diastole,
particularly of the thin-walled right atrium and right ventricle,
and prevents ventriculoatrial reflux when end-diastolic pressure is elevated.
- The pericardium plays an important role in the adaptation of the right ventricular stroke volume to the left ventricular stroke volume when systemic vascular resistance is elevated and equalizing compliance between the thin-walled right and thick-walled left ventricles,
resulting in interdependence of left and right ventricular filling (ventricular coupling).
2.- EMBRIOLOGY
Pericardial sinuses are formed during heart development.
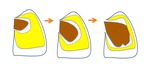
The pericardic sac covers the primitive heart tube.
When the pericardial sac folds,
both ends are joined: venous and arterial,
the fold that forms is the transverse pericardial sinus Fig.
14 and Fig.
15.
When the veins of the heart are formed and developed,
pericardial reflection that surrounds them,
form the oblique sinus.
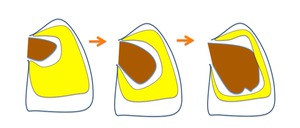
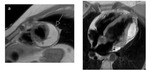
Fig. 14: Development of the pericardial cavity. The heart develops invaginating the serous pericardium wall, the serous pericardium forms a sack with two layers: visceral and parietal. This bag contains a virtual space called the pericardial cavity.
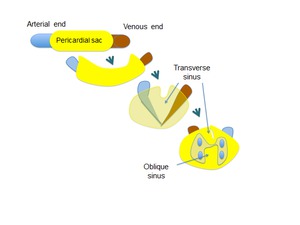
Fig. 15
3- Pericardium MRI study
With MRI we can study and correctly diagnose pericardial diseases.
MRI allows identifying the effusion,
quantify,
define its nature and its clinical repercussion.
• The transudate is usually hipointense on T1 and hyperintense on T2.
Fig.
2 and Fig.
16.
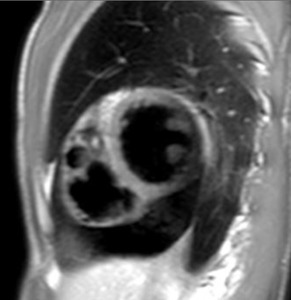
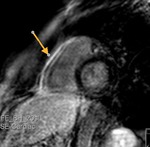
Fig. 16: Black-blood T1-weighted short axis image, shows severe peripheral effusion and the pericardium insertions into the sternum and the diaphragm.
•The isointense liquid in T1 is usually transudate.
•The acute-subacute hematic fluid is hyperintense on T1 and hypointense in T2* sequences.
Chronic hemopericardium is heterointense on T1 and T2 Fig.
17 and Fig.
18.
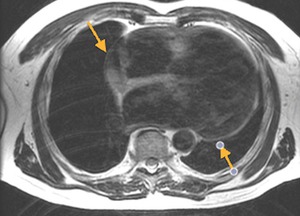
Fig. 17: Black-blood T1-weighted MR image,axial. Hematic pericardial effusion. Liquid-liquid level (above arrow), partially hyperintense on T1.
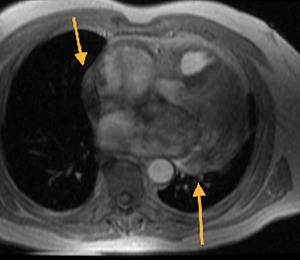
Fig. 18: Gradient-echo (GE) image, axial. Hematic pericardial effusion, arrows, showing hypointense signal (the paramagnetic effect of hemosiderin)
The pathology of the pericardium may be focal,
so the multiplanar orientation guarantees assesing all the pericardium,
including recesses.
The best plane to the evaluation is perpendicular to the pathology.
-Anatomical sequences SE T1 and T2 allow assesment of morphology and to detect the pericardial effusion.
-Cine MR GE and Steady-State Free Precession Imaging allows to evaluate the pericardial movement and its relationship to the adjacent structures.
-Phase contrast flow sequences to the flow measurement to show the clinical repercussion of the pericardial diseases.
-The Images after intravenous administration of gadolinium help identify the inflammation of the pericardium and distinguish better between the layers of the pericardium and fluid.
-The combination of morphological and functional techniques can identify anomalies and assess their functional impact.
-The pericardic study preferably be performed with cardiac and respiratory synchroniscm (apnea).
4.- Patology
4.1.
Congenital anomalies:
4.1.1 Pericardial defect. Fig.
19 and Fig.
20.
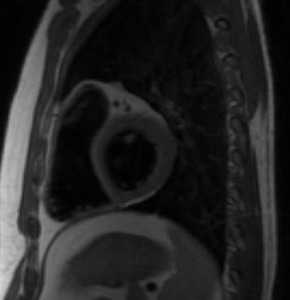
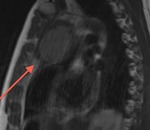
Fig. 19: Black-blood T1-weighted MR image, sagittal. Complete agenesis of the left pericardium.
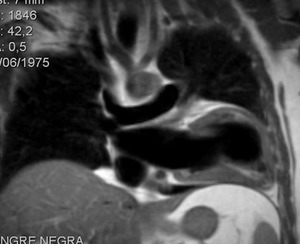
Fig. 20: Black-blood T1-weighted MR image. Complete agenesis of the left pericardium , that causes levodisplacement of the heart; the interventricular septum is disposed horizontally.
It is an extremely rare anomaly with a broad spectrum of abnormalities from a small to total partial defect.
The most common is the partial defect of the left pericardium and it is due to a deficit of intrauterine vascularization. Fig.
21 and Fig.
22.
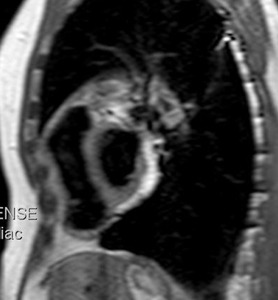
Fig. 21: T1-weighted, short axis. Patient with partial agenesis of the left pericardium. The epicardial fat contacts with mediastinal fat.
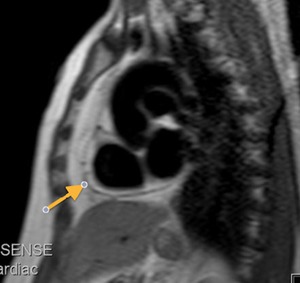
Fig. 22: Partial agenesis of the pericardium. Same patient as in the previous image. T1-weighted image, short axis. The arrow indicates the remaining thinned pericardium. Pericardium can be seen on the aortic root.
Congenital anomalies are usually asymptomatic and are discovered incidentally on chest radiograph or nonspecific chest pain,
symptoms may arises when cardiac structures are transiently entrapped or incarcerated in the defect,
when this happens,
often herniate left atrial appendage although it may be the ventricle.
There are reported cases of myocardial incarceration with sudden death.
The 30% of the pericardial defect are associated with other cardiac or extracardiac malformations.
The most common are a left-sided pericardial defect,
that determines an abnormality in the heart's position, levodisplacement of the heart and aortic knob in chest radiograph (Fig.
23) and rotates (Fig.
24) so that,
the interventricular septum is disposed horizontally in the axial plane.
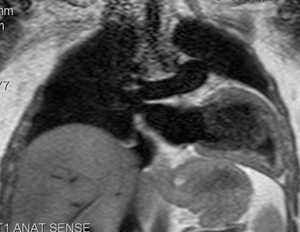
Fig. 23: T1-weighted image, coronal. Partial agenesis of the pericardium. The heart is located in the left chest, rotated and disposed horizontally.
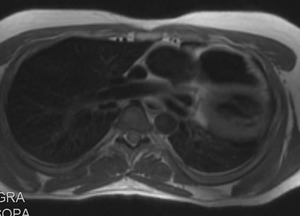
Fig. 24: Complete agenesis of the left pericardium.
Black-blood T1-weighted MR image, axial, shows levoposition of the heart and posterior location of the apex,the interventricular septum is disposed horizontally.
The main pulmonary artery bulges in the left lung and epicardial fat contact with the mediastinal pleura.
Fig.
25 and Fig.
26.
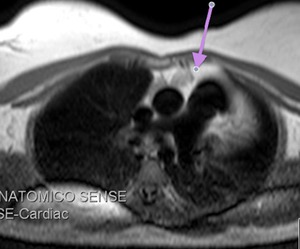
Fig. 26: Partial agenesis of the pericardium.
Black-blood T1-weighted MR image, axial. In this case there is no lung between the aortic and pulmonary root because there are pericardial remain overlying the aortic root.
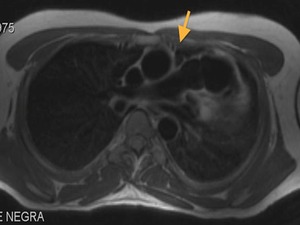
Fig. 25: Partial agenesis of the pericardium. Black-blood T1-weighted MR image, axial. In this case there is lung between the aortic and pulmonary root.
4.1.2 Pericardial Cyst and Diverticulum: Fig.
27 andFig.
28
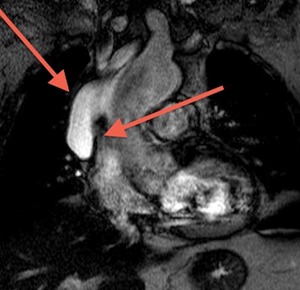
Fig. 27: Superior aortic recess between aorta and the superior cava.
T2-weighted MR image, coronal.
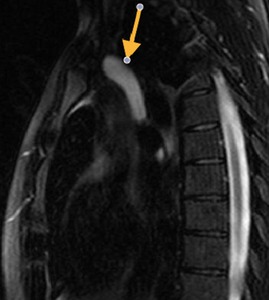
Fig. 28: Fluid located in the superior aortic recess that persisted in the same location on subsequent controls, which raised the differential diagnosis of pericardial cyst. T2-weighted image, sagital. Lesion with isointense contect (similar to CSF).
Pericardial cyst and pericardial diverticulum are rare congenital abnormalities and account for 7% of all mediastinal masses.
These parapericardial or pericardial mass rarely produce symptoms by compressing cardiac structures,
such as obstruction of the outflow tract of right ventricle.
They are more common in the right cardiophrenic angle,
which helps distinguish them from other cystic lesions such as bronchogenic or thymic cysts.
They can occur anywhere in the mediastinum.
Generally rounded,
unilocular,
can be pedunculated and / or calcified.
Diverticulum can be differentiated from a congenital cyst by the presence of direct communication with the pericardial cavity.
The diverticulum usually contents transudate and so are thin wall lesions thath have a homogeneous signal intensity,
isointense to CSF on T2-weighted sequences and often in T1,
sometimes may have a high protein content and in these cases the diverticula will be hyperintense on T1. Fig.
29,
Fig.
30 and Fig.
31.
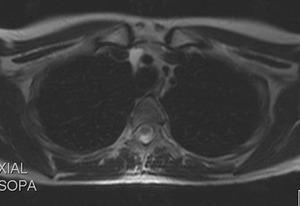
Fig. 29: Liquid located in the superior aortic recess that persisted in the same location on subsequent controls, which raised the differential diagnosis of pericardial cyst. T2-weighted MR image, axial, at the level of the supra-aortic trunks output. The lesion is isointense to CSF and continued until the supraaortic trunks output.
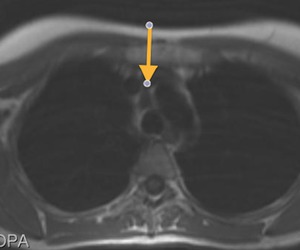
Fig. 30: Liquid located in the superior aortic recess that persisted in the same location on subsequent controls, which raised the differential diagnosis of pericardial cyst.
Black-blood T1-weighted MR image, axial.
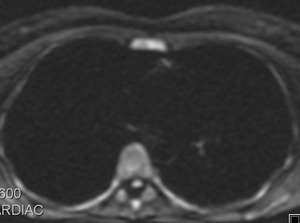
Fig. 31: Liquid located in the superior aortic recess, with not diffusion restriction, as befits the liquid, that persisted in the same location on subsequent controls, which raised the differential diagnosis of pericardial cyst.
4.2. Inflammatory and infectious pathology:
Acute pericarditis
Clinical syndrome secondary to inflammation of the pericardium,
in the acute phase is characterized by granulation tissue highly vascularized and fibrin.
Clinical manifestations: pain,
pericardial friction in the physical
exploration and electrocardiographic changes.
MR Image
-Pericardial thickening.
Fig.
32.
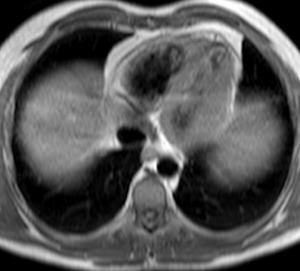
Fig. 32: Recurrent pericarditis. Black-blood T1-weighted MR image, axial.
Moderate diffuse pericardial thickening is observed. There were no signs of constrición.
-Gadolinium enhancement Fig.
33.
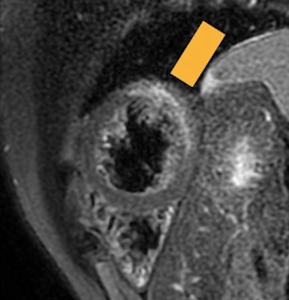
Fig. 33: Myopericarditis, Triple-IR T1-weighted, after IV gadolinium administration. Epicardial and myocardial uptake is observed.
-Alteration of the signal intensity of the pericardium,
hyperintense on T2-weighted sequences with fat suppression and STIR.
Fig.
34.
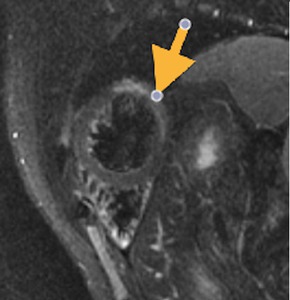
Fig. 34: Myopericarditis. STIR short axis image. Increased signal in the subepicardial, myocardial and pericardial.
Etiology
-By systemic diseases: Lupus,
rheumatoid arthritis,
scleroderma...Fig 35 and Fig 36.
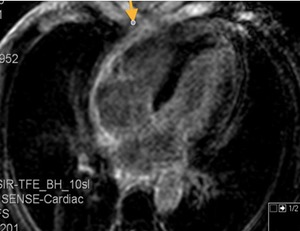
Fig. 35: Patient with SLE and repeated episodes of pericarditis. 4-chambers viability study image, after administration of IV gadolinium. Pericardial thickening and enhancement.
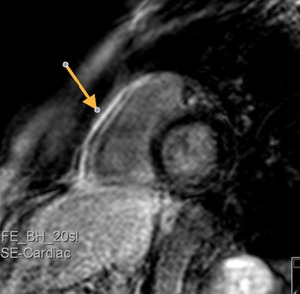
Fig. 36: Patient with SLE and repeated episodes of pericarditis. Viability study image, after administration of IV gadolinium, short axis. Pericardial thickening and enhancement.
-Secondary to pathology of adjacent structures such as myocardial infarction.
Fig.
37 and Fig.
38.
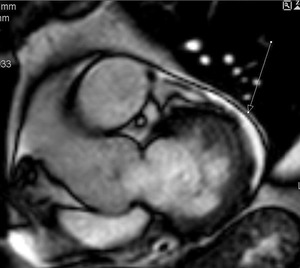
Fig. 37: Patient with AMI. Cine T2 image, short axis. The arrow indicates small pericardial effusion.
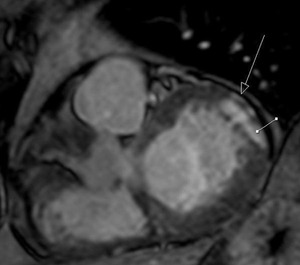
Fig. 38: Viability study image, short axis. Patient with acute myocardial infarction with pericardial enhancement.The line shows the infarcted myocardium enhancement.
-Postradiation.
Fig.
39 and Fig.
40.
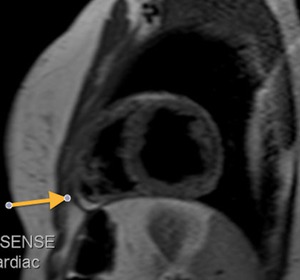
Fig. 39: Patient with a lymphoma treated with radiotherapy.
Black-blood T1-weighted MR image, short axis. The arrow shows the diffuse thickening of the pericardium.
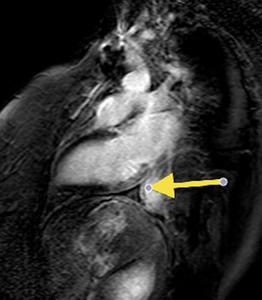
Fig. 40: Patient with a lymphoma treated with radiotherapy. Viability study image, after administration of IV gadolinium, short axis.
The arrow shows the diffuse thickening of the pericardium
-Neoplasic.
-Posttraumatic.
-Idiopathic...
Cardiac tamponade
Complication of pericardial effusion secondary to cardiac compression that prevents the normal filling of the cavities.
Often associated with moderate-severe effusion,
although the fast accumulation of a small amount of fluid can cause a substantial elevation in pericardial pressure and causes tamponade,
a slow accumulation of a considerable amount of fluid (up to 2 L or more) may have relatively unremarkable effects on ventricular filling.
It is a common complication in neoplasic pericardial effusion,
tuberculosis or purulent.
The most common effusions are viral or idiopathic because these are the most common cause of tamponade.
Nonspecific clinical presentation may be accompanied by shortness of breath,
chest pain and syncope.
Should be suspected if there are:
-jugular engorgement.
-paradoxical pulse.
The paradoxial pulse is abnormal decrease in systolic pressure and pulse amplitude during inspiration.
A negative intrathoracic pressure is created during inspiration,
which results in a decreased amount of blood leaving the heart that is manifested by a decrease in the amplitude of the arterial pulse greater than 20 mm Hg.
It is an urgent pathology so MRI is not usually done.
When the MRI study is done,
it is possible to determine the etiology of effusion and see signs of cardiac compression and abnormality movement of the interventricular septum.
The treatment is pericardiocentesis.
Chronic pericarditis
Chronic inflammation of the pericardium is characterized by progressive sclerosing pericarditis with fibroblasts,
collagen and by less fibrin deposition.
Fig.
41 y Fig.
42.
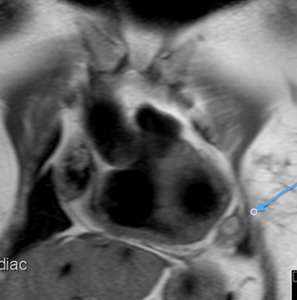
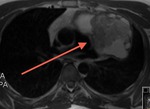
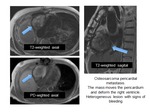
Fig. 41: Patient with operated congenital heart disease. T1-weighted image, coronal. Postoperative chronic pericarditis with pericardial hematoma. Focal pericardial thickening with fusiform lesion with hyperintense center on T1-weighted images and hypointense on T2-weighted images.
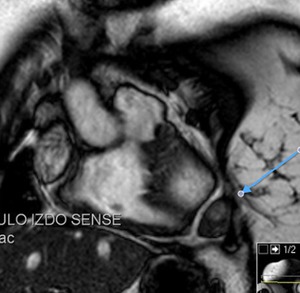
Fig. 42: Patient with operated congenital heart disease. T1-weighted image, coronal. Postoperative chronic pericarditis with pericardial hematoma. Fusiform lesion with hyperintense center on T1-weighted images and hypointense on T2-weighted images.
In the final stage it is formed chronic fibrosing pericarditis with fibroblasts and collagen.
Fig.
43,
Fig.
44,
Fig.
45,
Fig.
46,
Fig.
47 and Fig.
48.
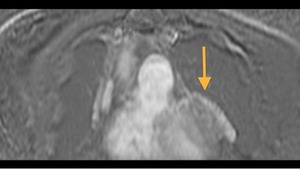
Fig. 43: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T1 subtraction image with and without IV gadolinium, coronal. Pericardial focal fusiform lesion with marked irregular peripheral enhancement, thicker in the periphery. Mass effect on the myocardium. Unchanged in size during 5 years of follow up. Pericardial hematoma associated with fibrosis (secondary changes to treatment)
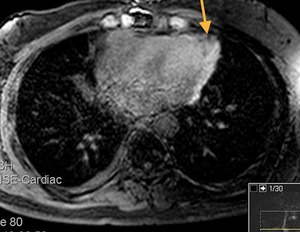
Fig. 44: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T1-weighted image with fat suppression, axial.
Fusiform pericardial focal lesion, hyperintense and well defined. Mass effect on the myocardium.
Unchanged in size during 5 years of follow up.
Pericardial hematoma associated with fibrosis (secondary changes to treatment)
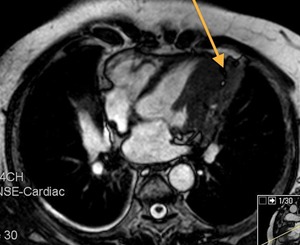
Fig. 45: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T2-weighted image, axial. Fusiform pericardial focal lesion, heterointense and well defined with mass effect on the myocardium. Unchanged in size during 5 years of follow up. Pericardial hematoma associated with fibrosis (secondary changes to treatment)
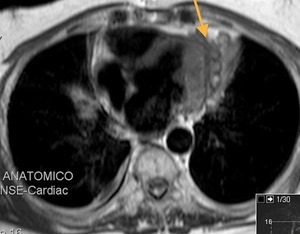
Fig. 46: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T1-weighted image, axial.
Fusiform pericardial focal lesion, hetereointense, with hyperintense foci, well defined and with mass effect on the myocardium. Unchanged in size during 5 years of follow up. Pericardial hematoma associated with fibrosis (secondary changes to treatment)
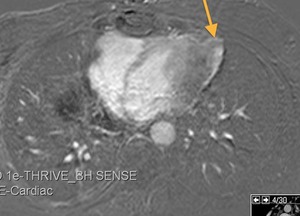
Fig. 47: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T1-weighted subtraction image with and without IV gadolinium, axial. Fusiform pericardial focal lesion with peripheral enhancement, more marked in the outer edge, with mass effect on the myocardium. Unchanged in size during 5 years of follow up. Pericardial hematoma associated with fibrosis (secondary changes to treatment)
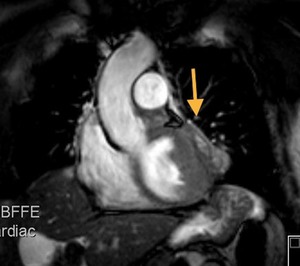
Fig. 48: Patient with a history of thymoma treated with surgery and radiotherapy 11 years ago. T2-weighted image, axial. Fusiform pericardial focal lesion, heterointense and well defined with mass effect on the myocardium. Unchanged in size during 5 years of follow up. Pericardial hematoma associated with fibrosis (secondary changes to treatment)
The main event of this final stage is a rigid pericardium with constriction of the heart.
Fig.
49,
Fig.
50
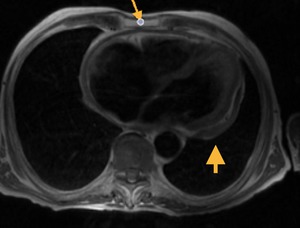
Fig. 49: T1-weighted MR image, axial. Marked pericardial thickening in patient with a history of pericarditis.
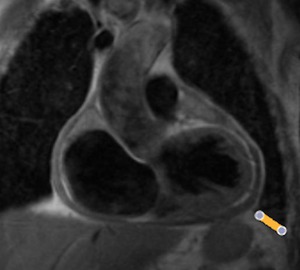
Fig. 50: T1-weighted MR image,coronal. Marked pericardial thickening in patient with a history of pericarditis.
Constrictive pericarditis
It's an uncommon condition,
secondary to chronic inflammation of the pericardium.
Thickening,
fibrotic and / or calcified pericardium,
that attaches to the myocardium,
which may result in impaired ventricular filling,
severe diastolic dysfunction,
and right heart failure.
Fig.
51,
Fig.
52,
Fig.
53 and Fig.
54.
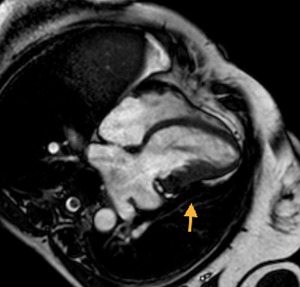
Fig. 51: Chronic constrictive pericarditis. Pericardial thickening with calcifications. The function study showed signs of constrictive pericarditis. Cine T2-weighted, 4 chambers. Arrow points to pericardial thickening with severe hypointense calcification of the pericardium that deforms the left ventricle.
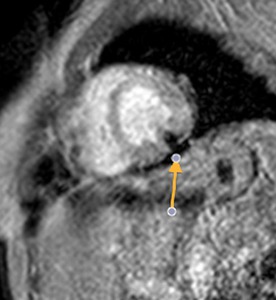
Fig. 52: Chronic constrictive pericarditis. Pericardial thickening with calcifications. The function study showed signs of constrictive pericarditis. T2-weighted Gradient-echo images, short axis. Arrow points to pericardial thickening with severe hypointense that represents calcification of the pericardium .
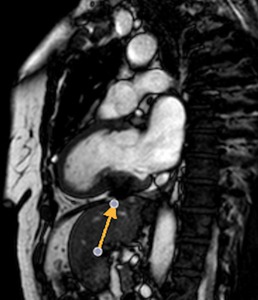
Fig. 53: Chronic constrictive pericarditis. Pericardial thickening with calcifications. The function study showed signs of constrictive pericarditis. Cine T2-weighted, sagital. Arrow points to pericardial thickening with severe hypointense calcification of the pericardium that deforms the left ventricle.
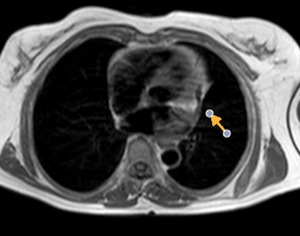
Fig. 54: Chronic constrictive pericarditis. Pericardial thickening with calcifications. The function study showed signs of constrictive pericarditis. T2-weighted image, axial. Arrow points to pericardial thickening with severe hypointense calcification of the pericardium that deforms the left ventricle.
Pericardial thickening is not always associated with constriction and constriction can occur with normal pericardial thickness.
Fig.
32.
MR is the proper technique to assess thickening of the pericardium presented hypointense on both T1 and T2-weighted sequences,
with suboptimal characterization of calcifications by this technique.
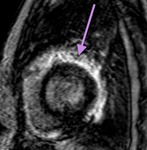
A focal pericardial thickening may condition constriction if it occurs in certain areas like in the atrioventricular groove.
Fig.
51.
Signs of constriction:
• Tubular ventricles especially the right.
Fig.
51.
• Vena cava and hepatic veins congestion.
• Pleural effusion.
• Both atrial dilation.
Fig.
58.
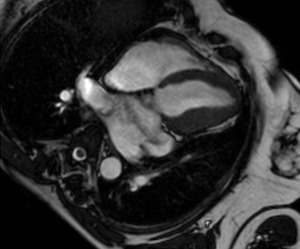
Fig. 58: Cine T2-weighted image, 4 chambers. Marked dilatation of the atria. Marked dilatation of the left atrial appendage.
•Rigidity of the pericardium in cine MRI sequences.
Fig.
55.
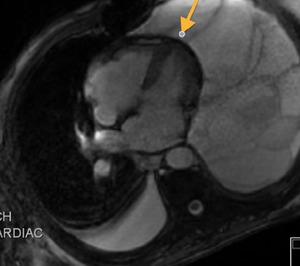
Fig. 55: Constrictive pericarditis. Pericardial thickening with calcifications.
Patient with left postneumonectomía and pericardial sheep plastia. MRI was performed in patients with poor ultrasound window by left heart failure. T2-weighted image, axial shows pericardial thickening with marked hipointensity, moderate dilatation of both atria with mild reduction in systolic function of both ventricles and diastolic dysfunction. Presented sigmoid interventricular septal motion. Reduction in diastolic volumes of both ventricles. Right pleural effusion, and no pericardial effusion. In surgery the plastia was attached and calcified.
•Paradoxical movement of the interventricular septum.
Fig.
59.
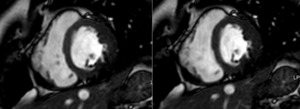
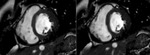
Fig. 59: T2-weighted cine, short axis. Patient with constrictive pericarditis. Paradoxical movement of the interventricular septum.
The association of pericardial thickening and septal bounce or paradoxical motion of interventricular septum ,
gives a very high sensitivity in the diagnosis of constrictive pericarditis.
,
gives a very high sensitivity in the diagnosis of constrictive pericarditis.
Morphological abnormalities:
• Pericardial thickening.
Fig.
50.
• Fibrosis and calcification: low signal on T1 and T2. Fig.
51,
Fig.
52 and Fig.
53.
• Normal pericardium thickness less than 2 mm.
If greater than 4 mm suggests constriction,
a value greater than 6.5 mm has a high specificity of constriction.
Fig.
50 and Fig.
53.
The diagnosis of constrictive pericarditis may not be based only on pericardial changes.
Function alteration:
1.
Diastolic function alteration: the maximum filling / ventricular pressure,
it is reached fast in diastole.
The E waveform is high and pointed and early and there is no A waveform,
that is,
the atrial contraction is not effective in ventricular filling.
Fig.
60.
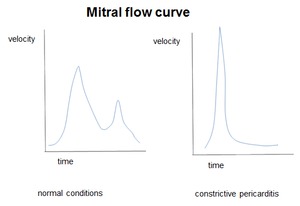
Fig. 60
2.
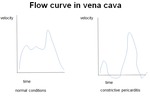
The venous flow curve shows decreased or absent systolic peak by increased pressure in the atria.
A similar pattern can be seen in restrictive myocardiopathy.
To distinguish both should be considered the venous flow in inspiration and expiration:
• In normal inspiration decreases the intrathoracic pressure and increases the systemic venous flow and increases the right ventricular filling and decreases left ventricular filling because increases the capacity of the pulmonary venous system.
Otherwise on expiration.
•In constrictive pericarditis this pattern is increased by the rigid pericardium,
in the restrictive myocarditis the pattern is normal or reduced.
3.
Paradoxical motion of interventricular septum,
that it’s convex towards the VI at the end of diastole when the right ventricular filling begins by the increase pressure in the right ventricle,
unable to relax.
This increases during the inspiration by the different behavior of arterial and systemic venous system.
Fig.
59.
MRI is the technique of choice to distinguish constrictive pericarditis from restrictive myocardiopathy.
Both have similar symptoms but a different treatment:
• The constrictive pericarditis is treated with pericardiectomy Fig.
56 and Fig.
57.
• Restrictive cardiomyopathy with medical treatment.
4.3 Tumor Pathology
Primary tumors are very rare,
much rarer than metastasis.
Mesothelioma is the most common malignant and is often associated with hemopericardium.
Primary:
• Benign: teratoma,
lipoma Fig 63,
fibroma,
hemangioma,
lymphangioma.
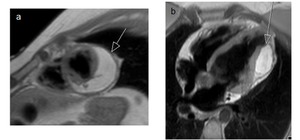
Fig. 63: Black-blood T1-weighted MR image a)short axis, b)four chamber.
Pericardial lipoma with infiltration of the pericardium.
Isointense mass, similar to fat in all sequences, replacing the visceral pericardium and partially the myocardium, that displaces the parietal pericardium and deforms the ventricle.
• Malignant: mesothelioma,
primary lymphoma,
sarcoma.
Teratoma is uncommon,
generally in pediatric patients,
can cause cardiac tamponade.
In the MRI image present fat / calcifications signal.
Treatment: surgical resection.
Mesothelioma: 50% of pericardial malignancies and 1% of all mesotheliomas.
Clinical presentation similar to pericarditis without / with cardiac tamponade presentation.
MRI is presented as homogenous masses on T1 and heterogeneous on T2,
with important gadolinium enhancement.
Surgical treatment with chemotherapy and radiotherapy.
If the tumors are infiltrating at the time of diagnosis have a poor prognosis.
Pericardial metastases are present in 10-20% of the cancer patients autopsies according to reports.
Fig.
64,
Fig.
65,
Fig.
66,
Fig.
67 Fig.
68 and Fig.
69.
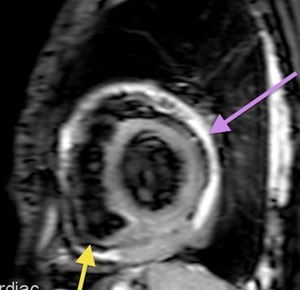
Fig. 64: Lymphoma. Black-blood T1-weighted with fat suppression after gadolinium IV administration, short axis. Diffuse enhancement of the pericardium.
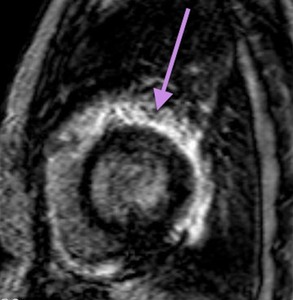
Fig. 65: Lymphoma. Viability image, short axis. Diffuse enhancement of the epicardium.
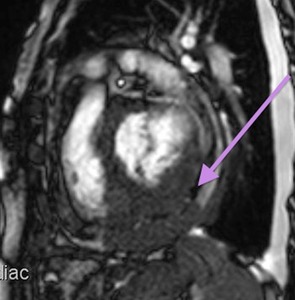
Fig. 66: Lymphoma. T2-weighted cine, short axis. Mass infiltrating the myocardium, epicardial fat and epicardium with mediastinal extension.
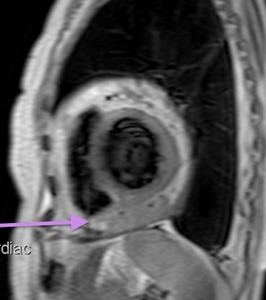
Fig. 67: Lymphoma. Black-blood T1-weighted MR image, short axis. Mass isointense to myocardium infiltrating epicardial fat and the epicardium.
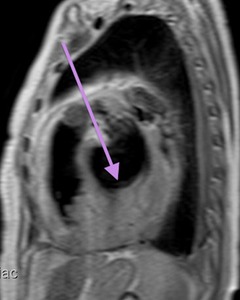
Fig. 68: Lymphoma. Black-blood T1-weighted MR image, short axis. Mass infiltrating the myocardium, epicardial fat and epicardium.
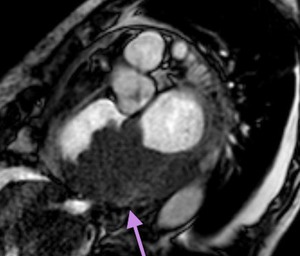
Fig. 69: Lymphoma. T2-weight cine, at the level of the heart valves. Hypointense mass that infiltrates the myocardium, epicardial fat, epicardium and mediastinal extension.
Access roads to the heart tumors are:
1.
Lymphatic (retrograde).
2.
Direct Extension Fig.
70,
Fig.
71 and Fig.
72.
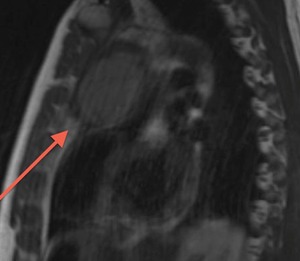
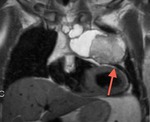
Fig. 70: T1-weighted image, sagittal. Mediastinal mass with pericardial invasion. AP: germ cell tumor with extensive infiltration of the pericardium
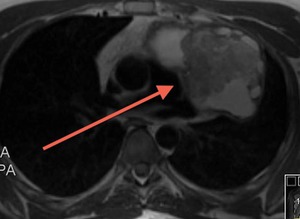
Fig. 71: T2-weighted image, sagittal. Mediastinal mass with pericardial invasion. AP: germ cell tumor with extensive infiltration of the pericardium
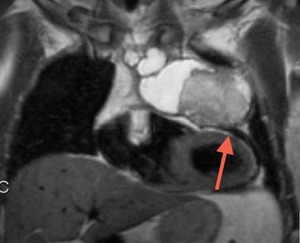
Fig. 72: T2-weighted image, coronal. Mediastinal mass with pericardial invasion. AP: germ cell tumor with extensive infiltration of the pericardium.
3.
Venous.
4.
Arterial hematogenous spread.
Fig.
73.
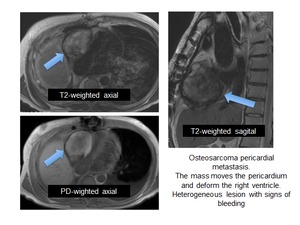
Fig. 73: Osteosarcoma pericardial metastasis
They are presented in advanced stages of the disease and are very rare as debut of the disease.
The primary tumors that most frequently metastasize to the pericardium are lung Fig.
74,
Fig.
75 and Fig.
76,
breast,
leukemia,
melanoma and lymphoma Fig.
69 and Fig.
68.
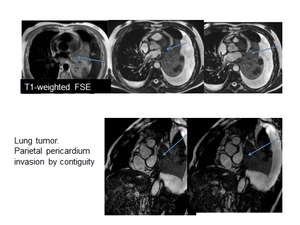
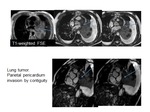
Fig. 74: Patient with lung tumor with invasion of the parietal pleura without invasion of the visceral pleura or myocardium.
Cine MR images, short axis.
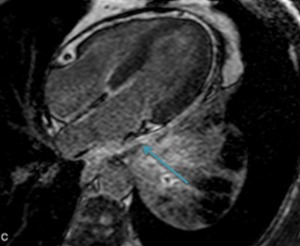
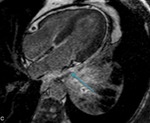
Fig. 75: Viability image, 4-chambers shows marked contrast enhancement. Patient with lung tumor with invasion of the parietal pericardium (blue arrow).
There are invasion of the parietal pleura without invasion of the visceral pleura and pericardium.
There is no contrast enhancement.
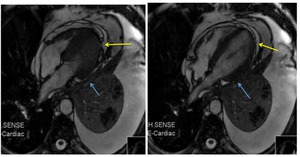
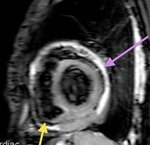
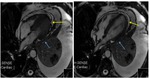
Fig. 76: T2-weigth cine images, 4-chambers. Patient with pulmonary tumor and invasion of the parietal pericardium. In the cine sequence the myorcardium movement is independent from pleural tumor.
Pulmonary neoplasia infiltrating the parietal pericardium. T2-weigth cine, axial. Mass (blue arrow) infiltrating the parietal pericardium. Pericardial effusion separates the visceral pericardium from the mass (yellow arrow)
Metastases usually present with pericardial effusion,
disproportionate to the mass.
Pericardial effusion with or without pericardial thickening,
nodules or masses.
They usually are asymptomatic.
MRI is superior to other imaging techniques because defining the mass between the effusion signal and pericardial fat and adds information over adjacent structures such as myocardial wall or great vessels.
Clinical presentation: dyspnea,
chest pain or coughing.
The effusion are presented as intermediate signal on T1 and T2-weighted sequences.
Melanoma can be hyperintense on T1-weighted sequences.
Differential Diagnosis in patients with neoplasic pericardial effusion:
• Metastases .
• Post Treatment secondary to radiation or drugs.
• Idiopathic.