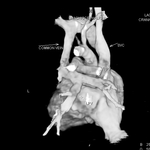
Anomalous Pulmonary Venous Return (APVR) occurs when there is drainage of one or more pulmonary veins outside the left atrium.
APVR is frequent in patients with congenital heart disease and/or heterotaxy.The presentation may range from incidental to conditions that may be lethal very early in life, if untreated. Diagnosis can be difficult or, even missed and made in adulthood with late presentation of clinical symptoms. On these grounds, early and accurate diagnosis of the morphology and type of APVR is of paramount importance for the decision making about treatment.
Although echocardiography is the initial examination when congenital heart disease is suspected, an exact and thorough investigation of the pulmonary venous system is not always achieved. Nowadays, magnetic resonance and/or computed tomography imaging are mandatory for an accurate diagnosis. In the following sections, we will describe the embryogenesis of the pulmonary venous system, the morphology and the classification of the various types of APVR and all these will be illustrated with CT images.
EMBRYOGENESIS
Lung development commences at approximately day 26 of gestation with the lung buds initiating from the foregut. The blood supply comes from the arterial system. The venous drainage is through the splachnic plexus that communicates with the cardinal system via the systemic cardinal and umbilicovitelline veins. From then onwards:
1. A primitive pulmonary vein or common pulmonary vein (CVP) develops as an outpouching from the left atrium and it subsequently begins to communicate with the pulmonary venous component of the splachnic plexus. Ultimately, it gives rise to four separate pulmonary veins, a pair at each side of the left atrium
2. The systemic veins involute:
- The right cardinal venous system develops into the right superior vena cava (SVC)
- The left cardinal venous system either disappears or develops into a left SVC (<1%).
- The umbilicovitelline veins develop into inferior vena cava (IVC), portal venous system and ductus venosus
In this way, the systematic and the pulmonary venous systems get separated.
Failure of any of these processes to occur leads to various anomalies:
1. In failure of separation of the systematic and pulmonary venous systems, some type of Partial or Total Anomalous Pulmonary Vein Return (PAPVR/TAPVR) will occur
2. In failure of incorporation of the main pulmonary vein at the dorsal left atrial wall pulmonary vein stenosis and/or atresia or cor triatum will occur.
1. FAILURE OF SEPARATION OF THE SYSTEMATIC AND PULMONARY VENOUS SYSTEM
1.a. TOTAL ANOMALOUS PULMONARY VENOUS RETURN
In this condition, all four pulmonary veins return to a cardiovascular structure other than the left atrium. It accounts for about 2% of all cardiovascular congenital anomalies and it is frequently seen in patients with heterotaxy syndromes, especially asplenia. It is a lethal condition unless there is shunting from the right heart (pulmonary circulation) to the left heart (systemic circulation). This usually manifests in the form of either an atrial septal defect (ASD)/patent foramen ovale (PFO) or a patent ductus arteriosus (PDA). Newborns present with symptoms of congestive cardiac failure and cyanosis.
Four categories are recognized, depending on the level of drainage:
- Type 1. SUPRACARDIAC LEVEL (45%-55%)
The most common type: all four veins form a confluence to one vertical vein posterior to the left atrium which finally drains into the innominate vein. Rarely, it may drain to SVC (right or left) or the azygous system. Thus, the innominate vein and the SVC are always dilated. Also, the right heart is usually dilated due to volume overload. Fig 1
- Type 2. CARDIAC LEVEL (20%-25%)
At this type, the pulmonary venous confluence drains to the right atrium either directly or through the coronary sinus. The pulmonary veins and the coronary sinus are significantly dilated
- Type 3. INFRACARDIAC LEVEL (25%-30%)
At this type, a descending vein arises from the pulmonary venous confluence, passes through the esophageal hiatus and drains to systemic veins below the diaphragm-usually the portal vein (at he confluence of the splenic and superior mesenteric veins) and, less often, to the ductus venosus, hepatic veins or IVC.
At this type, there is drainage of the pulmonary confluence at more than one levels. Fig 2
1.b. PARTIAL ANOMALOUS PULMONARY VENOUS RETURN
In this condition, at least one pulmonary vein drains to a location other than left atrium. This partially anomalous drainage usually affects the right lung and it results to a left-to-right shunt similar to an ASD/VSD/PDA. It accounts for about 0.4-07% of all cardiovascular congenital anomalies. Patients with PAPVR are typically acyanotic and only mildly symptomatic or asymptomatic and the condition may be diagnosed incidentally during imaging studies. When symptomatic, the CXR is usually normal. Findings that may raise suspicion of PAPVR are:
- An unusual course of a central venous catheter
- Focal mediastinal widening at the left of the aortic arch due to an anomalous left superior pulmonary vein
- A scimitar vein*
- Unusual patterns of pulmonary oedema, isolated in a particular lobe
- Effects of longstanding left-to-right shunts
Two categories are recognized:
- The most common form of PAPVR (80-83%) is drainage of the right superior pulmonary vein (RSPV) to SVC-including drainage to innominate vein or azygos vein. Fig 3
- Other forms include drainage into the coronary sinus, into IVC (scimitar syndrome) or drainage of all right pulmonary veins into the RA. Fig 4,5
* The Scimitar syndrome consists of anomalous drainage of the RLPV most commonly to the IVC, hypoplasia of the right lung (usually lower lobe) and ipsilateral pulmonary artery, dextroposistion and systemic arterial supply to the right lower lobe from either the descending thoracic or upper abdominal aorta. The anomalous vein appears at X-Rays as a semilunar tubular opacity at the right lower lung, lateral to the right heart border, resembling to the famous arabian curved swords. A pseudoscimitar syndrome occurs when the above findings are associated with an anomalous vein that drains into the left atrium
- Less common form of PAPVR (17-20%) is anomalous drainage of the left pulmonary veins to the left brachiocephalic vein, to the hemiazygos vein or the coronary sinus.
2. FAILURE OF INCORPORATION OF THE MAIN PULMONARY VEIN (MPV) AT THE DORSAL LEFT ATRIAL WALL
2.a. ATRESIA OF COMMON PULMONARY VEIN
At this form, there is neither connection of the pulmonary veins to the left atrium nor a major channel returning to the right heart. Thus, the pulmonary veins are usually underdeveloped and collateral channels drain the pulmonary venous blood to systemic venous circulation. The condition manifests with extreme cyanosis immediately after birth and it is lethal.
2.b. CONGENITAL STENOSIS OR ATRESIA OF INDIVIDUAL PULMONARY VEINS
This anomaly may present in isolation, in association with congenital heart disease or post-surgery for repair of anomalous pulmonary veins. Symptoms depend on the number of veins involved and the degree of obstruction.
2.c. COR TRIATUM
This anomaly accounts for up to 0.4% of all CHD and it occurs when normal pulmonary veins fail to incorporate into the left atrium.
At the classical form, there is a separation of the left atrium into one anterior (true left atrium) and one posterior (accessory) chambers located above the level of left atrial appendage. The posterior chamber receives blood from the pulmonary veins whereas the anterior drains into the left ventricle through the mitral valve. Communication between the chambers occurs through a fenestration with various degrees of stenosis. Fig 6
There are many variations of the classical form. Also, subtotal cor triatum may occur when the unilateral pulmonary veins drain at both the true left atrium, while the contralateral pulmonary veins drain to a systemic vein.
At the classical form, patients present with failure to thrive and symptoms of congestive heart failure, frequent pulmonary infections and hemoptysis.