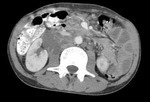
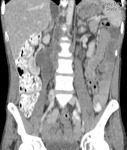
TUBERCULOUS LYMPHADENOPATHY
PATHOPHYSIOLOGY
Most common manifestation of abdominal TB, seen in around 60% of patients and usually associated with GI tuberculosis.
Routes of transmission include:
- Ingestion of infected material
- Haematogenous spread
- Direct spread from adjacent infected organs
The usual pattern is peripancreatic and mesenteric lymph node group involvement with multiple groups involved at anyone time.
IMAGING FEATURES
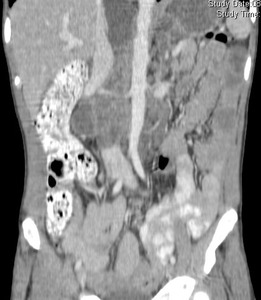
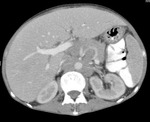
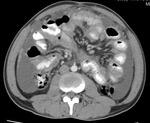
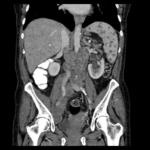
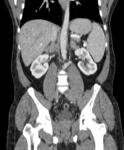
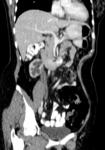
Fig.: Coronal reformat to illustrate grossly enlarged and low attenuation retroperitoneal nodes. This patient also had a tuberculous psoas abscess and chylous ascites (See Figs 2, 7, 37 & 38).
References: R Filobbos; Radiology, North Manchester General Hospital
Lymphadenopathy can be the only sign of disease especially in the periportal region.
Around 50% have enlarged nodes with hypoattenuating centres. This is highly suggestive of, but not pathognomonic of tuberculous necrosis.
Other patterns include increased number of normal sized nodes, scattered mildly enlarged nodes, clusters/masses of enlarged nodes.
Nodes can be circular/ovoid and measure between 12-40mm.
Lymph node masses do not tend to cause obstruction.
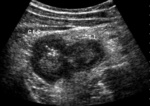
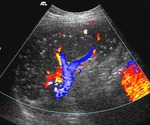
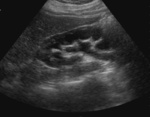
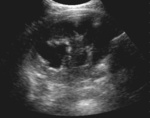
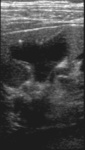
US may show discrete or conglomerate mass with central hypoechoic areas.
CT may demonstrate central non-enhancing caseating tissue 28-84HU, peripheral enhancement, and less commonly homogenous or mixed attenuation. Involved lymph nodes occasionally demonstrate calcification.
DIFFERENTIAL DIAGNOSIS
Peripheral enhancement and central necrosis is not pathognomonic and may be seen in lymphoma, metastasis, pyogenic infection, whipples disease, however its presence is highly suggestive of TB.
Other ancillary findings may suggest the diagnosis.
TUBERCULOUS PERITONITIS
PATHOPHYSIOLOGY
Tuberculosis peritonitis is the most common clinical manifestation of abdominal TB affecting upto 1/3 of all patients.
Rare in isolation and is usually associated with widespread intra-abdominal disease.
Spread is usually haemotogenous however may be due to ruptured lymph node, gastro-intestinal deposit or fallopian tube infection.
Present with abdominal pain, distension or fever.
IMAGING FEATURES
Three forms described:
Wet- Most common (90%). Features copious diffuse or loculated viscous fluid which is slightly hyperattenuating on CT due to high protein and water content.
Fibrotic/fixed- 60% cases. Characterised by large omental cake-like masses, tethered bowel and mesentery, occasional ascites
Dry/plastic- 10% of cases. Characterised by fibrous peritoneal reaction, dense adhesions, mesenteric thickening, caseous nodules (rare)
There can be considerable overlap between between the three types.
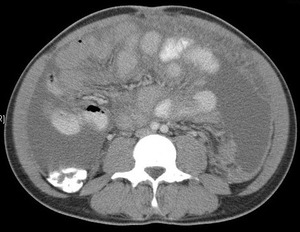
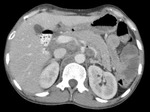
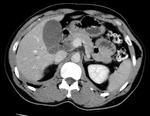
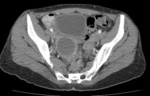
Fig.: Contrast enhanced CT scan shows dense ascites, thickened enhancing peritoneum and omental caking.
References: R Filobbos; Radiology, North Manchester General Hospital
Seen in 30-100% peritoneal disease.
May be free or loculated and can rarely have a fat/fluid level if chylous (rare).
US detects small volumes, loculations and septations.
CT detects typical high attenuation values (25-45HU) secondary to high protein content but can be near water density in the early transudative stage.
Rarely patients can develop chylous collections of fat density.
Micro (<5mm) or macro (>5mm) nodular lesions
Thickened mesenteric leaves with loss of normal architecture.
- OMENTAL AND PERITONEAL INVOLVEMENT
CT has greater sensitivity demonstrating enhancement and thickening.
Can be regular/irregular and appears caked, thickened or rarely nodular.
US shows diffuse, regular, echo-poor thickening of 2-6mm, or irregular thickening with tiny nodules.
Involvement well seen on contrast enhanced CT.
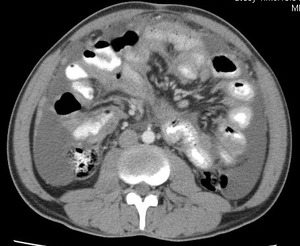
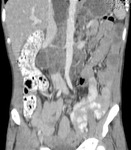
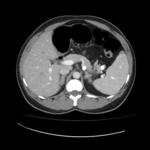
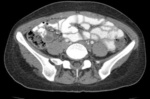
Fig.: Contrast enhanced CT scan shows dense ascites, thickened enhancing peritoneum and mesenteric leaves with lymphadenopathy and omental thickening. Also note thickening of the small bowel loops.
References: R Filobbos; Radiology, North Manchester General Hospital
GASTROINTESTINAL TUBERCULOSIS
PATHOPHYSIOLOGY
Rare manifestation of TB but common form of abdominal TB.
Usually caused by ingestion of bacilli in infected sputum or contaminated food.
Most frequently involves ileocaecal region, followed by ileum, caecum, ascending colon, jejunum, rectum, duodenum and stomach.
Three recognised forms:
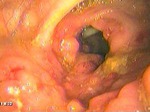
Ulcerative: Bacilli penetrate the mucosa and infect submucosal lymphoid tissue. Leads to mucosal sloughing and small, multiple irregular ulcers. Progresses to granuloma, caseous necrosis and cicatrisation.
Hypertrophic: Multinodular mucosal pattern or neoplasm like mass with abundant inflammatory response.
Disseminated: Via haematogenous and lymphatic route from distant source of infection.
IMAGING FEATURES
Normal CXR 50-60%
Barium examinations depict mucosal changes and ultrasound (US) and computed tomography (CT) demonstrate extramucosal changes.
CT demonstrates extent of disease and complications which include obstruction, perforation, abscess, fistulae, intusussception, vascular abnormality/ischaemia.
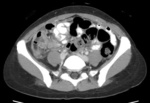
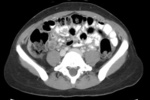
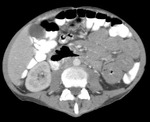
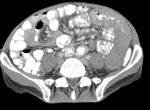
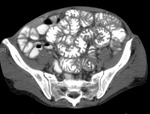
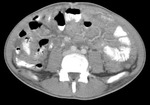
Gastrointestinal TB almost always involves the ileocaecal region and adjacent terminal ileum and caecum (90%).
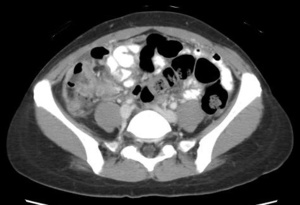
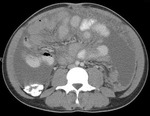
Fig.: Contrast enhanced axial CT shows thickening and enhancement of the medial caecal wall with thickening of the terminal ileum (See also Figs 9 & 10).
References: R Filobbos; Radiology, North Manchester General Hospital
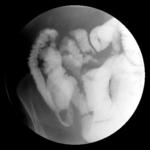
Barium may demonstrate thickening and or gaping of the ileocaecal valve with a narrowed terminal ileum which is thought to be characteristic (Fleischner sign). Usually non specific terminal ileal / caecal inflammation.
Double contrast enema reveals shallow ulceration with elevated margins.
Chronic changes lead to conical shrunken caecum and widely open ileocaecal valve and narrowed fibrotic terminal ileum (Stierlins sign) and short napkin ring stenoses.
US demonstrates uniform wall thickening, matted bowel loops, ascites and lymphadenopathy.
CT may show the characteristic appearance of asymetric thickening of ileocaecal valve and medial caecum and large heterogenous lymph node mass with adherent bowel loops and mesentery.
Low density centre caseating nodes may be seen with minimal/no change in pericaecal/mesenteric fat.
MR is becoming increasingly used to image the small bowel and shows the characteristic ileo-caecal thickening and hyperenhancement.
DIFFERENTIAL DIAGNOSIS
Crohn's disease- difficult differential in early stages
Lymphoma-again difficult in early stages
Amoebiasis-no small bowel involvement
Caecal carcinoma- limited by ileocaecal valve
| TUBERCULOSIS | CROHNS |
Chest radiograph | Positive chest film (50%) | Negative chest film |
Barium appearance | Fleischner sign | Cobblestone mucosa |
CT appearance | No creeping fat | Creeping fat |
Omental and peritoneal thickening | Normal omentum and peritoneum |
Enlarged low density nodes | Enlarged soft tissue density nodes |
Spread from adjacent lymph nodes or adjacent infected structures.
Symptoms are often due to extrinsic compression from lymphadenopathy.
Can manifest as ulceration and fistula formation.
Chronic change results in fibrosis, strictures and diverticulae.
Barium and CT useful for features and extent.
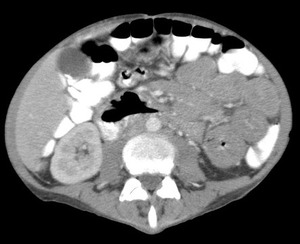
Fig.: Contrast enhanced CT shows gross circumferential wall thickening of the jejunum in a patient with gastrointestinal dissmeninated mycobacterium avium intracellulare whom also had lung involvement. The patient had HIV infection and was severely immunocompromised with a very low CD4 count and unfortunately succumbed to his infection shortly after this scan (see also Figs 18 & 19).
References: R Filobbos; Radiology, North Manchester General Hospital
Involvement usually associated with peritonitis and is rare.
Mucosal ulcers and fold thickening seen on Barium and CT, and bowel wall thickening seen on CT.
Only involved in isolation in 9%.
Long segment usually associated with ileocaecal involvement, short segment can occur in the hepatic flexure.
SOLID VISCERAL TB
PATHOPHYSIOLOGY
Prevalence of 80-100% at autopsy in patients with disseminated TB.
Can occur from pulmonary or miliary TB or via the portal vein from a GI primary.
IMAGING FEATURES
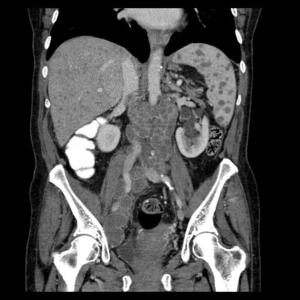
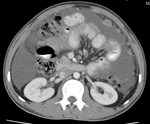
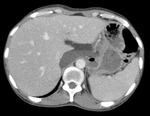
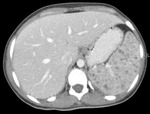
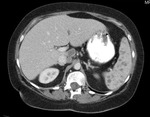
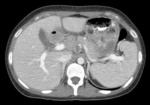
Fig.: Contrast enhanced coronal reformat shows multiple low attenuation foci in both the liver (miliary) and spleen (micronodular) and multiple enlarged low attenuation necrotic retroperitoneal nodes.
References: R Filobbos; Radiology, North Manchester General Hospital
Commonest appearance is hepato-splenomagaly.
Focal involvement is usually miliary, micronodular or macronodular.
Micronodular usually occurs in patient with miliary pulmonary TB and comprises multiple 0.5-2mm nodules.
CT may not detect the tiny nodules however US may reveal diffuse hyperechogenicity.
Macronodular is uncommon and appears as diffuse organomegaly with multiple hypoechoic/hypoattenuating massess 1-3cm, or a single tumour like mass. There is peripheral enhancement. On MR the lesions are of low signal on T1 and high signal on T2 weighted sequences.
The early appearances mimic abscess, however the tuberculous lesions calcify with time.
DIFFERENTIAL DIAGNOSIS
Metastases
Abscesses
Primary malignancy
IMAGING FEATURES
Tuberculous involvement of the pancreas is rare.
US demonstrates a hypoechoic lesion.
CT may reveal a focal hypodense necrotic lesion with enlargement of the pancreatic head.
DIFFERENTIAL DIAGNOSIS
Malignancy
Abscess
Chronic pancreatitis
IMAGING FEATURES
Seen in upto 6% of patients with active tuberculosis presenting as bilateral adrenal involvement with an Addisonian type picture.
On CT, active TB appears as bilateral enlargement with large hypoattenuating necrotic masses with or without calcification.
Over time, adrenal lesions calcify.
DIFFERENTIAL DIAGNOSIS
Metastases
Old haemorrhage and other causes of adrenal calfication.
TUBERCULOSIS OF THE GENITOURINARY TRACT
PATHOPHYSIOLOGY
Genitourinary TB is the most common clinical manifestation of extra-pulmonary tuberculosis.
4%– 8% of patients with pulmonary tuberculosis will develop clinically significant genitourinary infection.
25% of patients will have a known history of prior pulmonary tuberculosis and an additional 25%–50% of patients will have radiographic evidence of prior subclinical pulmonary infection
Infection is spread haematogenously or by direct extension.
URINARY TRACT
Haematogenous seeding results in small bilateral renal cortical granulomas which may lie dormant in the cortex of immunocompetent patients.
When immune defences are challenged the granulomas reactivate, enlarge and coalesce then rupture, delivering the organisms into the capillaries of the tubules and loop of Henle. Enlarging caseating granulomas and papillary necrosis result.
Progression occurs with granuloma formation, caseous necrosis, and cavitation which can eventually destroy the kidney.
Communication of the resulting granulomas with the collecting system leads to involvement of the pelvis, ureter and bladder and accessory genital organs.
Healing response results in fibrosis, calcium deposition, and stricture formation, which may result in obstruction and progressive renal dysfunction.
IMAGING FINDINGS
75% renal disease is unilateral and there is a long latency period between infection and presentation (5-40 years).
Calcifications are common occurring in up to 50% of patients. These may be amorphous, granular, curvilinear or focal and globular. Triangular ring-like calcifications within the collecting system are characteristic of papillary necrosis.
At intravenous urogram (IVU) papillary necrosis is the earliest sign of TB.
Papillary cavitation can be seen as pools of contrast and results in the spread of infection to the draining calyx. Fibrosis results and causes stenosis and strictures of the caliceal infundibula.
Infundibular strictures can lead to localized caliectasis seen on urogram and US, or an incomplete opacification of the calyx, phantom calyx, may be seen on urogram.
10%–15% of patients with active renal tuberculosis will have normal urographic findings.
Parenchymal scars occur in >50% of patients.
Scarring can cause sharp angulation of the renal pelvis known as the Kerr kink which may cause hydronephrosis.
End-stage tuberculosis results in autonephrectomy and extensive parenchymal calcification.
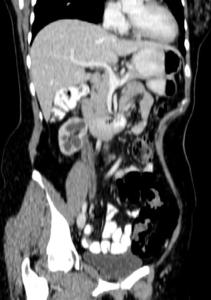
Fig.: Contrast enhanced oblique coronal CT in same patient as Fig 30. Shows chronically hydronephrotic kidney. The ureter is dilated with a thickened enhancing wall (same patient as in Fig 27).
References: R Filobbos; Radiology, North Manchester General Hospital
Ureteral involvement occurs due to the passage of infected urine and occurs in 50% cases or renal TB.
This is characterised by thickened ureteric wall and strictures and usually involves the distal 1/3.
Appearances that can result include sawtooth ureter due to dilatation and irregular mucosa, pipe-stem ureter due to the formation of strictures and ureteral shortening, and a beaded or corkscrew ureter due to several non-confluent strictures.
Generalised hydronephronephrosis may result.
Reduced bladder capacity is the most common finding in tuberculous cystitis and may be seen with wall thickening, ulceration and granulomatous filling defects.
A small irregular calcified bladder results in end-stage disease.
DIFFERENTIAL DIAGNOSIS
Chronic pyelonephritis
Papillary necrosis
Medullary sponge kidney
Caliceal diverticulum
Renal cell carcinoma
Transitional cell carcinoma
Xanthogranulomatous pyelonephritis
The most reliable radiologic feature in the diagnosis of genitourinary tuberculosis is the combination and multiplicity of features together with those ancillary findings noted on the different imaging modalities used.
GENITAL TRACT TUBERCULOSIS
PATHOPHYSIOLOGY
Genital tract TB detected in 1.3% female patients with tuberculosis.
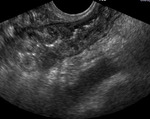
Almost always involves fallopian tubes causing bilateral salpingitis in females.
Affects salpinx & endometrium > ovary > cervix.
Usually haematogenous or lymphatic spread and occasionally peritoneal dissemination.
Mimics ovarian cancer in presentation and appearances and diagnosis is usually post-operative.
IMAGING FEATURES
Hysterosalpingogram reveals deformity and adhesions of the endometrial cavity and multiple constrictions and obstruction of the endometrial cavity.
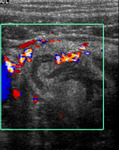
- Tubo-ovarian abscess (TOA)
Can result from TB salpingitis.
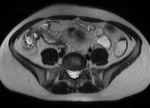
Seen as large complex adnexal masses on ultrasound with co-existing ascites.
On CT bilateral cystic or solid and cystic masses are accompanied by ascites, peritoneal thickening and infiltration of mesentery/omentum, with enlarged nodes.
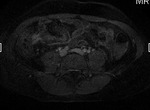
On MR tuberculous TOA’s have irregular low signal walls on T2 and may have a nodular inner wall which may help differentiate from usual TOA’s.
Late stage disease may reveal dense adhesions and loculated fluid collections.
In generalised peritoneal TB tubo-ovarian lesions may be inconspicuous and MR is recommended.
The findings may mimic peritoneal carcinomatosis. TB suggested by smoother peritoneal thickening or regular small nodules.
Laparoscopy and, in advanced cases, mini-laparotomy with tissue biopsy for histopathological examination is often recommended for final diagnosis.
DIFFERENTIAL DIAGNOSIS
Malignancy
Findings resemble ovarian carcinomatosis however the presence of calcifications and necrotic nodes are more suggestive of TB.
Atypical infection i.e.actinomycoses
PATHOPHYSIOLOGY
Usually involves seminal vesicles and prostate.
Spread is haematogenous and self limiting.
Involvement of testes and epididymis are rare.
IMAGING FEATURES
Occasional calcification (10%).
Contrast enhanced CT may reveal multiple hypoattenuating foci in the prostate.
Testicular and epididymal involvement reveals non-specific focal or diffuse hypoechogenicity on ultrasound.
DIFFERENTIAL DIAGNOSIS
Pyogenic infection
TUBERCULOSIS OF THE INTRA-ABDOMINAL SOFT TISSUES
PATHOPHYSIOLOGY
Tuberculosis can also involve the intra-abdominal soft tissues and abscess formation is a well recognised complication and presentation of intra-abdominal TB.
This can occur due to haematogenous spread of disease however tuberculous abscesses are most often the result of direct spread of micro-organisms from adjacent infection.
This often occurs in the psoas muscle as a result of tuberculous osteomyelitis of the vertebra or involvement of adjacent bowel.
IMAGING FEATURES
Imaging features on CT and US are similar to those of any other abscess including cystic/complex heterogenous mass.
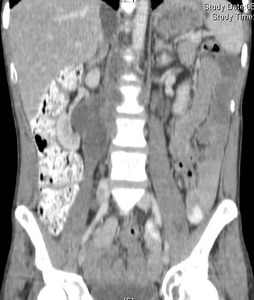
Fig.: Contrast enhanced coronal reformat (same patient as Fig 2, 3, 7 & 37) shows right tuberculous psoas abscess and enlarged necrotic retroperitoneal nodes.
References: R Filobbos; Radiology, North Manchester General Hospital
Ancillary findings of TB may be seen particularly abnormality/destruction of vertebral body, paraspinal abscess, ileocaecalor adjacent bowel involvement, low attenuation nodes, and ascites.
Diagnosis is confirmed with microbiology.
DIFFERENTIAL DIAGNOSIS
Pyogenic abscess resulting from another inflammatory/infective process for example in those with Crohns’ disease