Type:
Educational Exhibit
Keywords:
Lung, Thorax, Respiratory system, CT, CT-High Resolution, Conventional radiography, Drugs / Reactions, Infection
Authors:
Y. Song, C. M. Park; Seoul/KR
DOI:
10.1594/ecr2011/C-0855
Imaging findings OR Procedure details
Imaging review of pulmonary tuberculosis
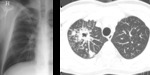
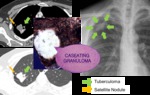
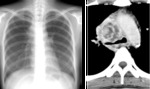
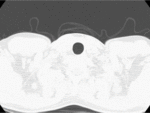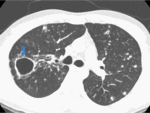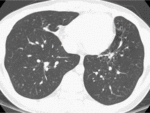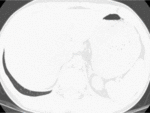
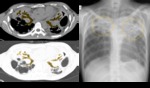
- Cavity(20-45%): The radiologic hallmark of reactivation TB and begins from the oldest portion of the lesions,
which are centrilobular in location.
Cavity occurs when an area of caseous necrosis liquefies and communicates with the bronchial tree.
The presence of a cavity is an important sign that indicates active disease.
(Fig.1,2)
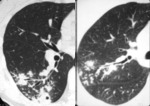
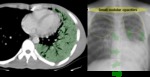
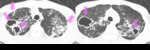
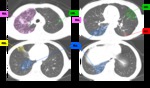
- Bronchogenic spread: The centrilobular small nodules and
tree-in-bud sign(branching linear structure 2 to 4 mm in diameter) reflect the presence of endobronchial spread and are due to the presence of caseous necrosis and granulomatous inflammation filling and surrounding terminal
and respiratory bronchioles and alveolar ducts.
These tree-in-bud signs are considered a reliable marker of the activity of the process.
(Fig.3,4)
- Tuberculoma(5%): A sharply marginated round or oval lesion measuring 0.5–4.0 cm in diameter. Most of these lesions remain stable for a long time,
and many calcify.
Enlargement
of a nodule,
or the development of a new one,
suggests either reactivation of TB or a new process,
such as carcinoma.
Satellite nodules around the tuberculoma may be present in as many as 80% of cases.
(Fig.5)
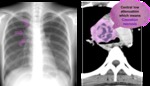
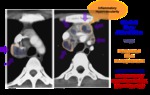
- Lymphadenopathy: The radiologic hallmark of primary TB.
Lymph node enlargement is the most common abnormality in children(90–95% of cases).
The prevalence of lymphadenopathy decreases with increasing age.
The lymphadenopathy is usually unilateral and located in the hilum or the paratracheal region.
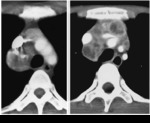
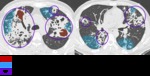
On CT,
the enlarged nodes typically show central low attenuation,
which represents caseous necrosis,
and peripheral rim enhancement,
which represents the vascular rim of the granulomatous inflammatory tissue.
(Fig.6-9)
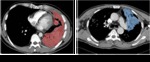
- Consolidation: Dense,
homogeneous air-space consolidations are typical CT findings of primary TB. Consolidation,
related to parenchymal granulomatous inflammation and usually unilateral, shows no predilection for any particular lung zone.
(Fig.10)
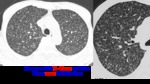
- Miliary nodules: Widespread dissemination of TB by hematogenous spread.
Miliary TB occurs in 2–6% of primary TB and also occurs somewhat more frequently in reactivation TB.
The characteristic CT findings of miliary TB consist of innumerable,
1- to 3-mm nodules scattered throughout both lungs.
(Fig.11)
Imaging features of MDR-TB compared with Drug-sensitive TB
Imaging findings of MDR TB do not basically differ from those of drug-sensitive TB.
However,
there are some differences reported on previous studies.
- The most characteristic CT finding of MDR-TB is the presence of multiple cavities in several studies (Fig.12,13).
The presence of a cavity itself does not mean multidrugresistant tuberculosis,
because 34% of patients with drugsensitive tuberculosis also showed a cavity on CT scanning.
Multiple cavities,
however,
strongly suggest the possibility of multidrug-resistant tuberculosis.
Limited drug penetration into the cavities that harbor large numbers of mycobacteria is believed to contribute to the drug resistance.
-
Findings of chronicity,
such as bronchiectasis (Fig.14) and calcified granulomas,
are more common in patients with MDR TB.
-
Bilateral involvements of parenchymal lesions such as nodules, tree-in-buds and consolidations were significant CT findings associated with primary MDR TB (Fig.15)
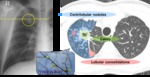
Imaging features of XDR-TB compared with non XDR-TB MDR-TB
-
Computed tomography findings of XDR-TB are basically similar to those of non-XDR MDR-TB.
Consolidations,
cavities,
bronchiectasis,
and lobular consolidations are frequent findings in XDR-TB patients (Fig.16).
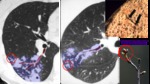
-
XDR-TB tends to have more extensive consolidation and
tree-in-bud appearance (Fig.17,18)