Patients.
Between October 2004 and November 2011,
a total of 183 consecutive patients with HCC underwent LT at our hospital.
Of them,
8 patients were excluded because of a short follow up period (≤2 months),
as a result of perioperative mortality.
The remaining 175 patients (151 men,
24 women),
who had a follow-up period longer than 2 months and had undergone dymanic-imaging evaluation at least 3 months before transplantation,
were included.
Previous treatment,
including surgical resection and loco-regional therapies had been undertaken in 119 patients.
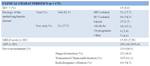
Table 1 summarizes clinical characteristics of the included patients.
Pretransplantation Imaging.
The preoperative dynamic-imaging examination performed closest to the time of transplant and within 3 months prior to LT was contrast-enhanced multiphase MDCT in 138 patients and contrast-enhanced MRI in 37 patients.
The mean interval between the last imaging examination and LT was 42 days with a range of 1-75 days.
MDCT examinations were performed using a 64-slice CT scanner (GE Medical Systems,
Milwaukee,
Wisconsin,
USA) with contrast enhancement and bolus-tracking technique to obtain a multiphase (arterial,
portal and hepatic venous phases) examination after an unenhanced scan. Dynamic MRI studies were conducted on a 1.5-T high field magnet (Achieva,
Philips Medical System,
Best,
The Netherlands) with a Phased Array coil.
The protocol included axial T1- and T2-weighted sequences with and without fat suppression and axial dynamic three-dimensional T1-weighted GRE sequences with fat suppression obtained before and after a bolus injection of gadopentetate dimeglumine (Gd-DOTA) in arterial,
portal and hepatic venous phases.
Pretransplantation imaging examinations were retrospectively reviewed by consensus by two experienced radiologists blinded to the results of the pathologic reports,
collecting data about the following features: presence of viable tumor,
number of viable hepatic lesions,
overall size of viable tumor,
diameter of the largest viable lesion,
lobar distribution of the tumor.
Histopathology of the explanted liver.
A pathologist experienced with liver pathologies reviewed all pathologic reports of the explanted livers.
The same features examined on imaging studies were evaluated on pathologic reports.
Moreover,
other collected pathologic data were: presence of microsatellitosis,
contact between tumor and hepatic capsule,
macrovascular and microvascular invasion,
histological subtype (HCC or combined hepatocellular-cholangiocarcinoma) and differentiation degree,
scored from grade 1 to 4 (10).
Recurrence analysis.
All available postoperative imaging examinations were retrospectively reviewed for evidence of recurrent HCC.
Proof of recurrence was made on the basis of biopsy or growth of new lesions with appropriate radiologic features,
combined with rising AFP levels or with negative work-up for another primary malignancy.
Statistical analysis.
The association between pretransplantation imaging features and explanted liver pathological features was evaluated by using the χ2 test.
Measure of association between imaging and pathology in the detection of viable tumor was also estimated separately for MDCT and MRI and for patients who had undergone pretransplantation treatment.
Accuracy,
sensitivity and specificity were calculated for imaging,
MDCT and MRI and compared using the McNemar test and Fisher exact test to estimate their diagnostic performance in the detection of viable tumor.
Incidence of recurrence was calculated and the Kaplan-Meier curve of disease-free survival rate was estimated.
The above-mentioned imaging and pathological variables were evaluated as potential predictive factors for HCC recurrence after LT by means of univariate analysis (χ2 test for categorical data and median test for continuous data).
For all statistical analyses,
a p<0.05 was considered to indicate a statistically significant difference.