Chest X-Ray is performed as the first level investigation,
but it result always nonspecific.
May be normal or more frequently can show an acute pulmonary embolism-like pattern,
with increase of pulmonary arteries diameter,
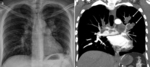
regional oligemia and parenchymal opacities suggestive of pulmonary infarcts (Figure 1a) [7].The main role of chest X-ray is to exclude other diseases that may present with similar symptoms and to make suggestions for the next work-up.
Scintigraphy is used in the diagnostic work-up of suspected pulmonary embolism,
it detects the consequences of filling defect on pulmonary ventilation and perfusion (mismatch).
It appear of limited value in the differential diagnosis,
because it does not allow direct visualization of the filling defects and does not allow to evaluate their precise nature,
location and extent.
Trans-esophageal echocardiography is also used in the diagnostic work-up of PAS,
because provides real-time details about valvular and ventricular function,
the physiological significance of the lesions and their effect on other cardiac structures [8].
Pulmonary angiography is rarely used in the diagnostic phase,
for best results of CT,
PET and MRI.
The angiographic signs are the presence of intraluminal opacification defects,
abrupt termination of an arterial branch and parenchymal perfusion defects.
PAS can also be present as polypoid filling defect,
moving during the cardiac cycle [8].
Computed Tomography (CT) allows to perform the first step in the differential diagnosis between PAS and pulmonary embolism.
The characteristics of CT for diagnosis of PAS compared to acute or chronic pulmonary embolism include:
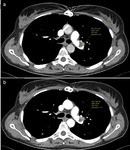
-Pulmonary artery filling defects iso-hypodense on scans acquired without contrast medium (30 HU on average,
hardly distinguishable from superimposed thrombotic formations),
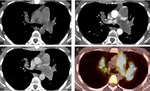
with subsequent patchy and delayed contrast enhancement in the Angio-CT,
even more evident during the venous phase,
with 25 -30 HU densitometric increasement,
on average (Figures 2 and 3).
- Pulmonary arteries increased in diameter,
with swollen and "padded" appearance of more involved traits; an extraluminal extension of the tumor in the mediastinum or in the lung parenchyma can be observed in some cases (Figure 1b).
- Pulmonary nodules with a possible "halo sign" expression of parenchymal metastases.
- Signs of right ventricular pressure overload,
as dilatation of the right cardiac chambers and tricuspid regurgitation of contrast medium.
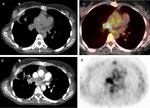
FDG-PET is used to differentiate between PAS and pulmonary embolism on the basis of the intensity of increased radiopharmaceutical uptake (Figure 2d,
4) [9,10].In fact FDG-PET shows increased radiopharmaceutical uptake at the level of tumor filling defects with values of standardized uptake value (SUV) suggestive of malignancy.
The thrombi,
instead,
generally do not exhibit increased activity but may have a slight increased activity in case of chronic embolism.
MRI is a second level imaging technique,
that allows a better characterization of the lesions on the basis of tissue characteristics and to better differentiate the thrombotic component from that neoplastic.
The main disadvantages of MRI are represented by the spatial resolution still lower than TC and the necessity of a greater duration of apnea,
considering that the majority of the patients examined for this condition are strongly dyspnoeic.
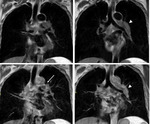
In black-blood T1 weighted sequences after administration of paramagnetic contrast agents,
typically PAS have significant contrast enhancement whereas thrombi are not,
but the possible association of PAS and thrombosis may further complicate the picture (Figure 5) [11].
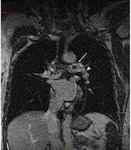
In order to differentiate between thrombosis and PAS it is possible to use FGRE IR sequences with inversion time of 600 ms,
that show the thrombotic material signal annulment (Figure 6),
while PAS usually appear isodense to muscle tissue.
The intensity of contrast enhancement after contrast medium is correlated with the degree of tumor differentiation [12] and can be also used in post-intervention follow-up and monitoring,
to evaluate residual or recurrent tumor.