There are no pathognomonic features of abdominal tuberculosis in radiological examinations and therefore,
microbiological or histological proof should always be obtained by percutaneous aspiration or biopsy.
However,
imaging studies may suggest the diagnosis,
especially in those patients whit multi-organ involvement.
The combination of multiple suggestive imaging features in the appropriate clinical context may be the clue to the diagnosis.
Imaging findings in AIDS patients are usually indistinguishable from those seen in non-AIDS patients.
Although tuberculosis can affect any organ in the abdomen,
emphasis is placed to intestinal involvement,
lymphadenopathy,
peritoneal tuberculosis and solid organ disease.
1. Lymphadenopathy
We found lymphadenopathy in 10 of our patients (Fig.
1 to 4).
It was the most common abdominal finding.
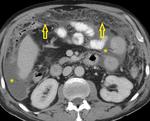
Mesenteric lymph nodes were the most commonly affected (7 patients).
In 3 patients nodes were markedly necrotic.
Lymphadenopathy is the most common manifestation of abdominal tuberculosis.
Although tuberculosis can affect any lymphatic region in the abdomen,
the distribution of the pathologic lymph nodes reflects the lymphatic drainage of the involved organs.
Mesenteric,
omental,
porta hepatis,
celiac and peripancreatic lymph nodes are most commonly involved.
The commonest route of transmition is the ingestion of infected material (sputum or milk),
with associated intestinal tuberculosis.
Haematogenous spread from a distant site of infection or direct invasion of the lymph nodes by adjacent infected organs are also possible routes of transmition.
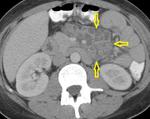
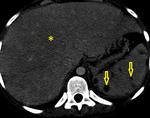
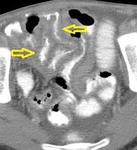
Lymphadenopathy patterns vary widely,
from increased number of normal sized nodes to large conglomerated masses (Fig.
1).
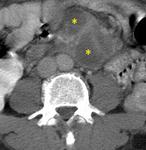
More commonly,
affected lymph nodes are multiple,
mildly enlarged circular or ovoid nodes.
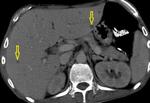
They often have central areas of necrosis (Fig.
2).
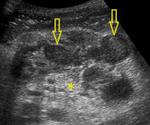
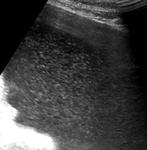
At US pathologic lymph nodes may appear as discrete nodular structures or appear as conglomerated masses (Fig.
3).
Enlarged nodes commonly have a central hypoechoic area.
At CT affected nodes may have low attenuation values or soft tissue density.
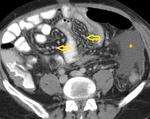
At contrast enhanced CT,
they have typical peripheral enhancement with central non-enhancing areas (Fig.
2).
This pattern reflects significant central liquefactive or caseous necrosis and perinodal highly vascular inflammatory reaction.
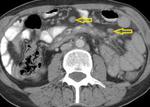
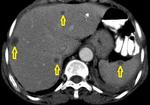
Homogeneous nodal enhancement (Fig.
4) or calcifications may also be seen.
The differential diagnosis of abdominal lymphadenopathy includes metastases,
Whipple disease,
lymphoma and mycobacterium avium-intracellulare infection.
2. Solid organ disease
At our institution 10 patients showed typical manifestations of hepatosplenic disease,
appearing as liver and splenic enlargement and multiple abscesses of variable size (Fig.
5 to 7).
Solid organ involvement may occur in association with intestinal tuberculosis,
caused by dissemination through the portal venous system.
Mycobacterium tuberculosis may also reach the liver and spleen by haematogenous or lymphatic spread.
Accordingly to the literature the prevalence of hepatosplenic disease is as high as 80-100%.
However,
the most common presentation is a nonspecific hepatosplenomegaly,
which occurs due to a fine miliary infiltration of the parenchyma (Fig.
5).
Individual lesions are often below the resolution limits of imaging methods.
Visible abscesses appear at US as round hypoechoic lesions of variable sizes.
Larger lesions may have a heterogeneous appearance.
At CT microabscesses are multiple tiny hypoenhancing focci (Fig.
6).
The macronodular form is rare,
presenting with single or multiple hypoechoic,
heterogeneous and sometimes calcified abscesses.
On CT they appear as solid,
hypodense,
heterogeneous masses with rim enhancement after contrast administration (Fig.
7).
MRI shows hypointense and slightly hyperenhancing lesions on T1-weighted images.
On T2-weighted images,
the lesions are hyperintense with a hypointense rim relative to the surrounding liver.
Tuberculous microabscesses of the liver and spleen may simulate metastases,
fungal infections,
sarcoidosis and lymphoma.
The differential diagnosis of the macronodular form includes metastases,
abscess and primary malignancy.
3. Intestinal tuberculosis
Intestinal wall thickening was found in 8 patients (Fig.
8 and 9).
All the patients with intestinal involvement showed alterations in the ileocecal region.
Three patients had concomitant jejunal disease and one patient had involvement of the ascending and transverse colon.
The ileocecal region is the most common area of involvement in the gastrointestinal tract,
due to the abundance of lymphoid tissue,
followed by the ileum,
cecum,
ascending colon,
jejunum,
the rest of the colon,
duodenum and stomach in descending order of frequency.
Mycobacterium tuberculosis bacilli infect the gastrointestinal tract after ingestion of sputum or infected milk.
The bacilli penetrate the mucosa and infect the submucosal lymphoid tissue.
Ulceration of the mucosa occurs,
which can be demonstrated by barium studies.
Disease progresses with oedema of the intestinal wall,
granuloma formation and caseous necrosis.
Dissemination to abdominal viscera can also occur by haematogenous and lymphatic routs from a distant source of infection.
Intestinal involvement is present in in 80-90% of patients,
however,
radiologic alterations are seen only in 50% of cases.
The number of cases found in our institution supports this prevalence.
Barium studies may show mucosal ulcerations,
thickening of the ileocecal valve and a wide gapping between the valve and the narrowed terminal ileum (Fleischner sign).
In advanced disease the cecum appears conical and shrunken.
US may reveal regular and concentric bowel wall thickening.
At CT,
the most common findings are circumferential wall thickening of the cecum and terminal ileum and asymmetric thinking of the ileocecal valve (Fig.
8 and 9).
The differential diagnosis for ileocecal tuberculosis includes Crohn disease,
amebiasis,
lymphoma and colon carcinoma.
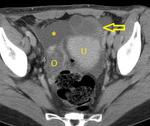
4. Peritoneal tuberculosis
Peritoneal tuberculosis was also common among our patients (Fig.
10 to 13).
Ascites was found in 8 cases and peritoneal thickening in 5 patients.
Three of those 5 patients had multiple peritoneal nodules.
One patient had omental involvement.
Peritoneal disease is usually associated with widespread abdominal tuberculosis involving lymph nodes or intestine.
Tuberculous involvement limited to the peritoneum is rare.
Indeed,
all the patients with peritoneal tuberculosis diagnosed in our hospital had concomitant involvement of other abdominal organs.
Peritoneal involvement is most commonly caused by rupture of an infected lymph node into the peritoneal cavity.
Haematogenous or lymphatic seeding may also occur.
Other possible routes of transmition are direct invasion of the peritoneal layers from adjacent infected structures or the discharge of caseous material from the fallopian tubes.
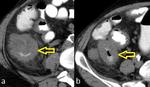
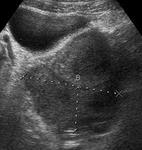
US shows the presence of free or loculated fluid,
often with multiple mobile strands of fibrin and echogenic debris (Fig.
10).
Echogenic thickened mesentery with or without enlarged mesenteric lymph nodes is also characteristic (Fig.
3).
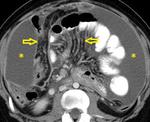
At CT,
ascites has high attenuation values due to the high protein content of the fluid (Fig.
11).
Chylous ascites is rare and when present,
a fat-fluid level is seen.
In rare cases,
ascites may have low attenuation values,
close to those of water.
This probably reflects a transudative phase of the disease,
due to immune reaction without infectious peritonitis.
CT may also show regular or nodular peritoneal and mesenteric thickening,
with loss of normal mesenteric architecture and increased mesenteric vascularity (Fig.
12).
Thickened peritoneum usually shows contrast enhancement.
Omental involvement may appear as omental nodules,
diffuse infiltration and thickening.
Omental cake may be seen (Fig.
13)
Peritoneal tuberculosis is traditionally described in three different types.
The wet-ascitic type is the most common and is associated with large amounts of free or loculated ascitic fluid.
The fibrotic-fixed type is less common and is characterized by omental involvement,
matted bowel loops and mesentery and occasionally loculated ascites.
The dry-plastic type is uncommon and is characterized by fibrous peritoneal reaction,
peritoneal nodules and dense adhesions.
However this classification is not accurate enough to describe all combinations of imaging features.
The differential diagnosis of peritoneal tuberculosis includes peritoneal carcinomatosis,
malignant mesothelioma and nontuberculous peritonitis.
5. Associated Findings:
5.1 Thoracic findings
On literature reports only 15% of patients with abdominal tuberculosis have evidence of pulmonary disease.
Surprisingly,
in our institution,
all the cases of abdominal tuberculosis had associated thoracic findings and lungs were normal in only two patients.
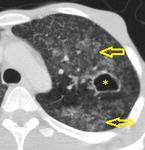
Most of the affected lungs (10 patients) showed miliary disease and 7 patients had condensation and cavitation of the pulmonary parenchyma (Fig.
14 and 15).
Pleural disease characterized by pleural effusion with or without pleural thickening was found in 8 patients.
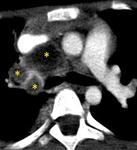
We found mediastinal or hilar lymphadenopathy in 9 cases (Fig.
16).
In post-primary tuberculosis parenchymal disease is usually characterized by parenchymal condensation and cavitation with predilection for the apical or posterior segment of the upper lobes.
Multiple segments are involved in most cases and bilateral disease may be present.
Cavitation usually occurs within areas of consolidation and indicates activity.
Endobronchial spread is also common in active disease appearing as small,
poorly defined centrilobular nodules (“tree-in-bud” appearance) (Fig.
14).
Pleural effusion is usually small and associated with parenchymal disease.
Tuberculous empyema and bronchopleural fistulas may also occur.
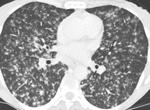
Miliary disease reflects haematogenous dissemination of the Mycobacterium tuberculosis and appears in lungs as multiple,
well defined micronodules with a random distribution (Fig.
15).
Miliary disease is usually associated with multiple organ involvement.
The presence of suspicious features in thoracic imaging,
such as parenchymal cavitation and miliary disease,
although not pathognomonic,
should raise the possibility of pulmonary tuberculosis with concomitant abdominal disease.
5.2 Genitourinary tuberculosis
Although genitourinary tuberculosis is the most common manifestation of extra-pulmonary tuberculosis,
in our institution genitourinary involvement was found in only 1 male and 2 female patients,
involving bladder and fallopian tubes respectively (Fig.
17 and 18).
The kidneys are often primary sites for genitourinary tuberculosis,
being achieved by haematogenous route.
Ureters and bladder may be involved by descent infection.
Female genital tuberculosis involves fallopian tubes in 94% of cases (Fig.
17).
Tubo-ovarian abscesses may form (Fig.
18).
Prostate is the most affected organ of the male genitals.
Prostatitis or prostatic abscesses are common.
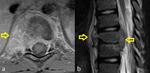
5.3 Musculoskeletal tuberculosis
Among patients with abdominal tuberculosis,
we found 2 cases of concomitant musculoskeletal disease,
both affecting thoracic spine (Fig.
19).
Tuberculous spondylitis typically affects more than one vertebra,
with predilection for the anterior half of vertebral body.
Infection involves disc spaces which may collapse.
Paravertebral abscesses are also common (Fig.
19).
Other forms of musculoskeletal involvement include extraspinal osteomyelitis,
most commonly seen in extremities and tuberculous arthritis mainly affecting large weight-bearing joints.
5.4 Other findings
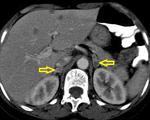
In our study we also found 1 patient with adrenal involvement and another patient with orbital tuberculosis.
Adrenal involvement in tuberculosis is rare.
It may manifest as unilateral or bilateral adrenal masses with central areas of necrosis (Fig.
20).
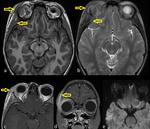
Orbital tuberculosis (Fig.
21) is extremely rare.
Although any patient in our study had central nervous system disease,
it should also be mentioned due to its prevalence and clinical relevance.
Tuberculous meningitis is the most common manifestation of neurotuberculosis.
Parenchymal disease can occur with or without meningitis and usually manifests as either solitary or multiple tuberculomas.