Keywords:
Trauma, Infection, Computer Applications-Detection, diagnosis, CT, Thorax, Emergency
Authors:
V. Miele1, V. Di Giacomo1, I. Di Giampietro1, S. Ianniello1, G. Menichini2, B. sessa2, M. Trinci3; 1Rome/IT, 2Roma/IT, 3Roma, ITALY/IT
DOI:
10.1594/ecr2013/C-0589
Conclusion
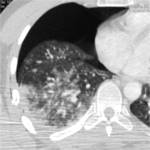
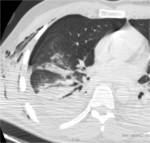
Ground glass and micronodular may be considered early development pattern evolving towards lobar parenchymal consolidation or disomogeneous consolidation,
which together account for approximately 44% of pulmonary complications in patients with polytrauma.
The EOP develops in about 7 days after the event of major trauma,
but the "ground glass" and "centrolobular nodules" patterns can be considered the precursors of this important involvement.
On the basis of these results the pattern of early appearance can be considered as the new "risk factor" for the development of a bronchus pneumonic process.
The ICU anesthesiologist can and should use these data to decide early medical therapy feasible at least 3-4 days before the full-blown pneumonia appear.
This leads into an important reduction of the risk of multi-organ failure and late mortality and in a lesser time of hospitalization of the polytraumatized patient for lung causes.
Particular attention should be paid to patients with chest drainage,
which can be considered a predisposing factor but is not essential for the occurrence of an infectious complication.
All 45 patients with infectious pulmonary complications were intubated during hospitalization.
Several authors consider intubation and mechanical ventilation in the first hour an important risk factor for the development of the EOP (2,6).
Our future perspective is to deepen this study applying this further distinction.