Study population
44 patients (age 82.5 range: 69-92; 50% females) with severe aortic valve stenosis were examined with contrast enhanced ECG-gated 128-slice dual source CT (gantry rot.
0.28s) prior to transcatheter aortic valve implantation (TAVI) for procedure planning.
CT examination
Image acquisition was performed using 128-slice dual source CT (SomatomDefinitionTM Flash,
Siemens Healthcare,
Forchheim,
Germany)
For contrast enhancement 70 to 110ml of iopromide (Ultravist 370™,
Bayer Schering Pharma,
Berlin,
Germany) were injected via a cubital vein using an automatic injector at a flow rate between 4,5ml/sec and 5,5ml/sec followed by a saline chaser (40 ml).
The CT scan was triggered into the ascending aorta using a ‘bolus tracking technique’,
after a CT-attenuation of 100 Hounsfield Units [HU].
Scan delay was 10 seconds after the threshold was reached.
The ECG was recorded simultaneously during scan and retrospective ECG-gating was performed.
Images were reconstructed in 5% intervals over the cardiac cycle (5-45%) at 0.75mm width,
increment 0.5 and a medium smooth convolution kernel [B 26 f].
Echographic examinations
TTE measurements were performed by experienced Cardiologists (Department of Internal medicine III: Cardiology; University hospital Innsbruck) using a standard ultrasound system (Acuson Sequoia 256,
Acuson-Siemens Medical Systems,
Malvern,
Pennsylvania) equipped with a 3.5/1.75-MHz transducer.
Especially Doppler flow rates from the left ventricular outflow tract (LVOT),
peak transvalvular velocity and AV-gradients were measured.
AVA was calculated using continuity equation approach.
CT image analysis
CT-Datasets were analyzed retrospectively using a syngo.via workstation (Siemens healthcare,
Forchheim,
Germany).
Image quality was scored in a 4-point scale (1= excellent,
no artifacts; 2=good,
minor artifacts such as motion blurring,
double contouring,
stair-steps; 3= moderate,
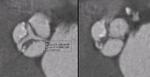
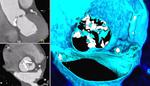
moderate artifacts still being diagnostic 4= poor/non-diagnostic) for each phase. AVA was measured during all phases from a multiplanar reformation (MPR) in the cross-sectional aortic valve plane.
Statistical analysis
The maximal AVA (AVAmax) and minimal AVA (AVAmin) of all systolic phases were selected.
The mean (AVAmean) was calculated from all phases over 10-35%.
AVA by CT was compared to values from transthoracic echocardiography (TTE) calculated by Doppler continuity equation (VTI- integral).
The AVAbestcorrel was defined.
Statistical data analysis was performed using PASW statistics V 18 [SPSS Inc,
Chicago,
USA].
The correlations between AVA measured by CT and TTE were determined using linear regression analysis and the Pearson’s correlation coefficient.
A two-tailed probability value of less than 0.05 was considered statistically significant.