Aetiology
FAI is characterized by an abnormal contact of the bony components of the hip,
particularly during flexion and intra-rotation,
when the anterior aspect of the femoral head-neck junction hits the acetabulum,
thus reducing hip range of movement [1].
In this setting,
normal movements performed when an abnormal anatomic is present lead to an abnormal contact between articular surfaces,
then leading to relevant degenerative abnormalities [3].
The cause of this pathologic condition is mainly congenital [4].
FAI can be considered as one of the most frequent causes of early hip osteoarthritis,
especially in young active subjects [4].
In these subjects,
the repetition of movements,
typical of sport activities,
cause a repetition of conflict,
thus making symptomatic a condition that would have never been manifest in sedentary subjects [5].
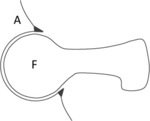
Classification
On the basis of different morphologic alterations that can be found in the hip,
two different kinds of FAI can be encountered (Fig.
1) [1].
There is also a third type of FAI,
in which morphostructural alterations of both types can be seen concurrently [1].
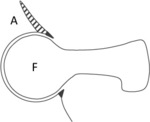
In cam type FAI,
the main finding is a difference in the curvature of acetabulum and femoral head,
not perfectly spherical in normal conditions,
in which a large irregularity (bump) of the femoral head-neck junction can be seen,
causing the typical pistol grip deformity (see Fig.
1b) [6].
This finding is responsible for cartilage tears of the anterior superior aspect of the acetabulum,
that may lead to labral avulsion at later stages [6].
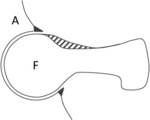
In pincer type FAI,
the main cause is represented by an overcovering acetabulum – sometimes also associated to pelvis retroversion [7] – that covers almost completely the femoral head,
thus limiting its movements (see Fig.
1c).
This overcoverage may also be secondary to FAI,
as degenerative capsular thickening caused by repetitive microtraumas may be associated to osteophytes occurrence [8].
Hence,
some authors described a fourth type of FAI,
typical of subjects performing sport activities in which the hip is highly involved – e.g.
dance or martial arts.
In these activities,
normal hip is heavily solicited by unfavourable transversal forces,
that may lead to develop the abovementioned lesions [3,8].
Finally,
cam type FAI may be also associated to an acetabular undercoverage,
that represents a residual of a dysplasia and may have different grades of severity.
This condition makes loads concentrating over a tiny area of cartilage,
thus favoring early damage and early instability,
in turn leading to typical morphostructural alterations [9].
Symptoms
FAI has generally a subtle onset.
Patients usually report groin pain,
rarely posterior or lateral,
and difficult to perform movements in hyperflexion [10].
Symptoms are increased when standing up after long time seated.
Sometimes,
hip may snap or partially block due to labral tears [10].
Clinical tests
Clinical examination of a patient with suspect FAI includes three tests.
a.
anterior conflict test (flexion,
adduction,
intrarotation = FADIR),
it is considered the most sensitive and specific test.
With the patient lying supine on the table,
the physician flexes 90° patient’s knee and rotates it internally,
then adding an adduction movement.
When positive,
the test elicits groin pain.
b.
Drehmann’s test (flexion,
abduction,
extrarotation = FABER).
With the patient lying on the table,
the physician moves patient’s foot of the affected side on the contralateral knee,
then applying a medial-lateral pressure on the knee of the affected side.
When positive,
the test elicits hip pain.
c.
posterior impingement test.
With the patient lying supine and hip positioned on the edge of the bed,
the physician forcely extends and extrarotates patient’s affected limb.
When positive,
the test elicits posterior-lateral gluteal pain.
Imaging
X-ray evaluation
Patients with clinical suspicion of FAI generally undergo X-ray evaluation first.
This examination is very important in the diagnosis of FAI,
as it allows for detecting the anatomic and scheletric abnormalities that are typical of this condition,
both on the femur and the acetabulum.
At the beginning of the disease,
subtle FAI findings can be seen,
while characteristic signs of hip osteoarthritis are not already visible [2].
Anterior-posterior (preferably performed with patient standing) and axial 45° flexion femoral (also known as 45° Dunn’s projection) projections should be always performed.
Further projections can be performed,
such as Lequesne’s false profile and lateral pelvis projection to evaluate sagittal tilting.
Radiographic evaluation must be always performed on both hips [2,12].
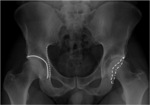
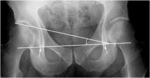
a.
anterior-posterior projection: patient is standing,
with lower limbs 15° intrarotated.
The symmetry of ischiatic foramina and the alignment of sacrum-coccyx axis with pubic symphisis must be carefully achieved (Fig.
2) [13].
b.
axial 45° flexion femoral projection: patient is supine with the affected hip 45° flexed and 20° abducted.
The greater trochanter should not be projected over the neck or the femoral head [12].
c.
Lequesne’s false profile: patient is standing with pelvis 65° rotated and affected hip placed in contact to the radiographic plate.
The foot of the affected side must be parallel to the plate and x-ray beam must be centered on the femoral head [13].
The radiographic evaluation allows for detecting both direct signs of FAI (e.g.,
abnormal femoral head sphericity,
acetabular over- or undercoverage,
and acetabular retroversion) and lesions that are subsequently caused on articular structures [12].
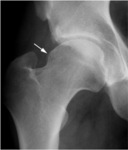
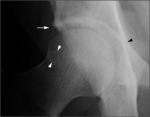
Cam type FAI can be detected as an abnormal femoral head sphericity,
with convex appearance of the head-neck junction for the presence of a typical anterior bump (Fig.
3).
This finding causes a conflict between the femur and the acetabulum during hip flexion and internal rotation.
The anterior bump can be detected only in the anterior-posterior projection when located on the superior-lateral head-neck junction; only in the axial projection when located anterior to the head-neck junction; or in both projections when bump has a wider extension.
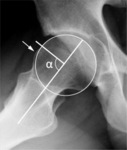
Such abnormality can be quantified calculating the angle between the major axis of the femoral neck and the base of femoral head-neck junction abnormality [1].
That angle,
also known as α angle,
is regarded as abnormal when greater than 55° (see Fig.
3b).
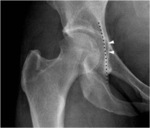
Pincer type FAI is caused by an overcoverage (coxa profunda and protrusio acetabuli) or a retroversion of the acetabulum.
Acetabular depth is normal when the bottom of the acetabulum is projected laterally to the ilio-ischiatic line on the anterior-posterior projection (Fig.
4).
When the acetabular bottom is in contact or crosses the ilio-ischiatic line on the medial side,
a coxa profunda can be diagnosed.
When the femoral head is projected medially to the ilio-ischiatic line,
a protrusion acetabuli can be diagnosed.
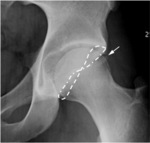
The relationship between the margin of the anterior and posterior acetabular profiles on the anterior-posterior projection allows for assessing the physiological acetabular antiversion or retroversion.
When the acetabulum is antiverse,
the anterior acetabular profile is located medially to the posterior profile,
that remains lateral.
When acetabulum is retroverse,
the anterior acetabular profile crosses the posterior profile,
thus creating the typical “8-shaped” cross-over sign (Fig.
5).
If the radiographic projection is not correctly performed,
the cross-over sign cannot be correctly evaluated [7].
Moreover,
a lateral pelvic projection is useful to assess the anterior-posterior tilt (normal value approximately 60°) [14].
The radiographic evaluation has also the role of establishing the conditions that can be potentially responsible of FAI as a consequence of coxo-femoral instability,
related to an acetabular undercoverage (i.e.,
residual hip dysplasia).
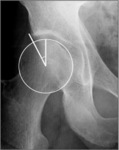
This condition can be quantified measuring the Wiberg angle (Fig.
6) and the acetabular index (Fig.
7) on the anterior-posterior projection.
The Lequesne index,
calculated on the homonym projection,
can be also useful to quantify an anterior acetabular undercoverage.
A number of studies demonstrated that the abovementioned findings can be associated together,
thus generating mixed conditions of FAI cam+pincer (see Fig.
5),
and that both cam and pincer conditions can be associated to hip instability [1,14].
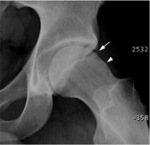
Radiographic evaluation can also detect indirect signs of FAI.
The detection of subcortical cysts at the site of conflict,
particularly at the anterior femoral head-neck junction,
is a typical sign of FAI in the most advanced cases (Fig.
8).
What once was defined as herniation pit,
it is now considered as a fibro-osteitis on the site of impact with acetabulum in cam-type FAI [15].
The detection of an os acetabuli (see Fig.
5,
Fig.
9) is another finding that is frequently associated to FAI [16].
Thin calcifications around the acetabulum represent labral ossification,
secondary to degeneration,
that can be seen especially in pincer-type FAI (see Figg.
8,9) [24].
As already reported,
it is important to note that radiographic findings must be tightly correlated to clinical evaluation and patient’s age.
For example,
an anterior bony bump can be frequently seen in elderly patients affected by simple hip osteoarthritis.
Diagnostic performance of radiographic evaluation in FAI demonstrated variable results according to the considered projection.
For anterior-posterior projection,
sensitivity was reported to be 60% and specificity 81%.
For axial hip projection,
the same data were 70-74% and 63%,
respectively,
while Dunn’s projection reaches values of 91-69% and 88%,
respectively [17,18].
A recent paper on acetabular retroversion reported that the evaluation of such parameter is burdened by a relevant interobserver reproducibility,
that progressively reduces as observer’s experience increases [19].
Ultrasonography
Relevance of ultrasonography in the diagnosis of FAI is limited.
If this imaging modality is fundamental in the evaluation of neonatal hip [20],
in adults it is limited to the detection of intra-articular effusion,
evaluation of inflammatory,
degenerative or post-traumatic conditions,
or to the guidance of diagnostic or therapeutic intra-articular injections [21].
Being a deep joint,
hip ultrasonography is commonly performed using a low-frequency convex probe.
Some authors reported that ultrasonography is able to detect most acetabular degenerative tears [22].
However,
to date,
the only study that proposed an ultrasonographic evaluation of FAI was performed by Buck et al.
[23],
who proposed three qualitative criteria to evaluate the anterior and anterior-superior profiles of the femoral head-neck junction,
and to quantify α angle in cam-type FAI.
The features of ultrasonography (low cost,
wide availability and lack of ionizing radiations) would make it the ideal imaging modality for preliminary cam-type FAI screening.
However,
results [23] do not agree with such an hypothesis,
particularly because the evaluation of α angle only seems to be not enough to diagnose FAI [23].
Finally,
being not useful to evaluate intra-articular abnormalities,
ultrasonography has a limited value in the assessment of patients with painful hip.
However,
in the hands of an expert operator,
the detection of secondary signs of FAI may be useful to suggest a correct diagnosis and then a further workup with other modalities.
Computed tomography (CT) and MR
The radiographic evaluation of FAI is limited by the lack of visibility of non-osseous structural abnormalities of the hip joint: the labrum,
sinovitis,
and the early chondral damage.
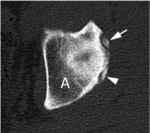
CT allows for a more accurate evaluation of the bone structures (see Fig.
9),
with limitations that are similar to radiographic evaluation [15].
The morphologic evaluation of femoral head-neck junction with modern CT systems can be obtained using multiplanar reconstructions oriented along neck axis,
with submillimetric slice thickness.
CT allows for an accurate evaluation of calcific metaplasia of labrum,
scarcely detectable using MR.
Conversely,
MR allows for a more precise evaluation of subcortical bone sufferance,
represented with low signal on T1-weighted sequences and high signal on T2-weighted sequences.
However,
the simple MR evaluation allows for a limited analysis of labrum and of the cartilage-labrum complex,
that are of paramount importance when a surgical approach is foreseen [24,25].
In this setting,
MR arthrography (MRA) is considered the standard of reference [25,26].
This technique implies the intra-articular injection of about 20 mL of a 1:250 solution of gadolinium-based contrast agent.
The capsular distension caused by the injection allows for evaluating with improved detail the anatomic structures and their damages.
It is advisable that intra-articular injection is performed using an imaging guidance,
as it has been demonstrated that hip injection without guidance is burdened by 40% insuccess [27].
Contrast agent injection must be performed very slowly,
explaining to the patient that the procedure can be variably painful and can be associated to lameness lasting from few minutes to seven days.
Within the magnet,
the patient is positioned in supine position,
and the feet should be bound together with a tape in 15° intrarotation,
thus allowing for muscle relaxation.
MRA examination starts with axial and coronal T1- and T2-weighted fat-saturated and non fat-saturated sequences,
including the iliac wings and the lesser femoral trochanter.
Then,
T1-weighted or proton density sequences should be performed,
with axial and coronal oblique orientation centered on the femoral neck and with double oblique sagittal orientation centered on the labrum.
The examination can be completed with radial sequences oriented along the major axis of the femoral neck: these sequences can be included in the standard package provided with MR system,
or isotropic volumetric T1-weighted sequences can be reformatted on radial planes.
These sequences have the greater advantage of sections that are always perpendicular to the labrum,
with a low occurrence of artifacts,
thus allowing a 360° evaluation of femoral head-neck junction [28].
Using fat saturation helps to obtain better images but may limit the detection of important signs for FAI diagnosis,
such as subcortical sclerosis,
labrum calcifications,
and labral myxoid degeneration [29].
In the diagnostic setting of FAI,
several aspects should be considered.
a) evaluation of skeletal morphology: presence of pistol grip-like head-neck complex deformity and bump-like irregularity of the femoral head-neck junction (Figg.
10).
These conditions cause an increase over 55° of α angle,
typical of cam type FAI.
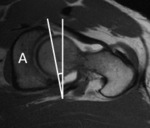
On standard non-oblique axial scans,
also when performed for non-contrast examinations,
the acetabular anti- or retroversion degree can be measured (Fig.
11) (to be evaluated together with anterior-posterior pelvis projection) and the degree of femoral coverage (in association to Lequesne’s projection),
responsible for pincer type FAI.
The presence of femoral head structural failure should be carefully evaluated and a precise quantification should be given.
Such parameter can be also evaluated on routine non-contrast sequences.
b) evaluation of chondral erosion and damage of femoral head and acetabular surface: it is important to describe the articular rim (wideness and symmetry) [29] and calculate the extension of the chondral damage (in percentual or in centimeters).
These parameters cannot be adequately evaluated using standard MR,
except for advanced chondropathy associated to subchondral edema (hyperintense on T2-weighted sequences),
that extremely important for surgical planning.
Regarding the site,
chondral damage occurs more frequently on the anterior superior portion of the acetabulum in cam type FAI,
while posterior inferior localization is more frequent in pincer type FAI (countercoup lesion) [29].
Previous studies demonstrated that MRA has extremely variable sensitivity (50-77%) and specificity (79-84%) in the detection of cartilage tears [24,26].
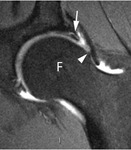
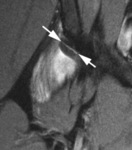
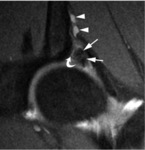
c) cartilage-labrum complex: it is important to differentiate advanced labral degeneration and a labrum that is morphologically normal but detached from the acetabulum or affected by longitudinal tears (see Fig 10,
Figg.
12,13) [30].
Czerny et all [24,26] classified labral tears in traumatic and degenerative.
Lage et al.
defined an arthroscopic classification subdividing abnormalities in four classes [30].
However,
these classifications are not completely accepted.
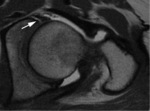
Labral damage can occur with tears having horizontal (Fig.
10) or radial course (see Fig.
12) or degenerative tears (see Fig.
13),
frequently associated to para-labral cysts (see Fig.
13) or geods [29-32].
Labrum may occasionally have a hypertrophic appearance,
often due to calcific metaplasia (more easily detectable using computed tomography),
typical of cam type FAI,
associated to an unstable joint [9].
Similarly to what happens for shoulder,
conventional MR is able to detect large abnormalities of the labrum,
especially when associated to joint effusion that may mimic arthrographic effect.
Previous studies demonstrated that conventional MR has 30% sensitivity and 36% accuracy in the detection of labral tears,
in comparison to 90% and 91%,
respectively,
of MRA.
Therapeutic options
In literature,
the use of drugs and physiotherapy in FAI patients has low consensus.
However,
it is a diffuse opinion that conservative treatment,
being not able to modify the morphologic aspects that are involved in this pathologic condition,
cannot represent a real solution [33].
Patients with hip pain lasting over 6 months,
unresponsive to conservative treatment,
in which radiographic signs of FAI are present should undergo surgical treatment [34].
Three surgical techniques allows for treating morphologic abnormalities on which FAI is based and the associated lesions:
a.
open surgery: described first by Ganz et al.,
implies surgical luxation of hip and subsequent correction of femoral and acetabular bone abnormalities after labrum resection [35].
Some orthopedic surgeons perform also cartilage repair using microperforations or chondroplasty [36].
b.
arthroscopy: it represent a less invasive technique but it is more difficult to perform.
In the articular space,
cartilage tears can be treated and acetabulum can be reduced,
detaching and re-inserting the labrum; outside the joint space,
femoral bump can be reduced,
checking the disappearance of conflict using dynamic manoeuvers [37].
c.
mini-open technique: it represent a mixed technique,
in which femoral neck osteoplasty is performed in open surgery without luxation through a small anterior incision,
while intra-articular abnormalities are treated using arthroscopy [38].
At similar rate of post-surgical short- and long-term success,
arthroscopy has the lower complication rate [39].
In open surgery,
possible complications are trochanter pseudoarthrosis and trochanteric bursitis,
eterotopic calcifications,
and capsular fibrosis,
while in mini-open surgery lateral femorocutaneous nerve lesion is the most frequent complication (17-45%),
followed by transitory neuroapraxis of pudendal and femoral nerve [39].
In patients in whom FAI led to advanced osteoarthritis,
conservative surgery are contraindicated and hip prosthesis represents the only solution.
The role of general radiologist
Given what reported up to now,
it is clear how FAI diagnosis is extremely complex and involves a series of different parameters that cannot be summarized by a single radiological examination.
Also,
after initial enthusiasm about FAI description and abundant literature published in few years,
scientific community is now dealing with overdiagnosis.
Indeed,
abnormalities that are found in FAI are present in a number of asymptomatic subjects and can lead to a misleading diagnosis if not strictly correlated to clinical symptoms [2].
In this setting,
the general radiologist has a crucial role.
On the one side,
some subtle diagnostic signs are not clearly visible on routine radiologic examinations.
However,
on the other hand,
some radiologic findings,
correlated to young age of patient and to a specific clinical condition,
may suggest the presence of FAI.
The detection of such signs may provide useful signs to clinicians to address a further diagnostic workup on targeted examination to reach an early diagnosis of FAI.
This is particularly important,
as it is thought that an early conservative treatment is able to slow the progression of osteoarthritis process,
although long-term studies on this topic are still missing [2,7].