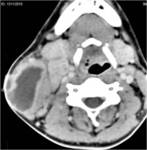
A- Pulmonary tuberculosis
- 1. Primary tuberculosis:
Most common form of pulmonary tuberculosis.
Asymptomatic.
Typically manifests radiologically as:
- Parenchymal disease (atelectasis)
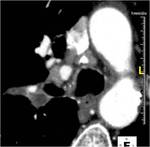
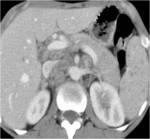
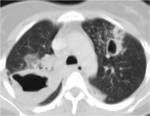
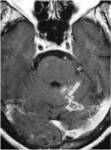
- Lymphadenopathy (fig.1)
- Pleural effusion
- Miliary disease
The chest radiographs may be normal.
CT is more sensitive for parenchymal diseases++
- Sequelae of PT are more see as:
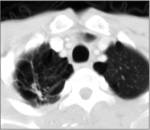
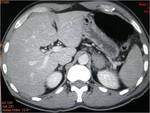
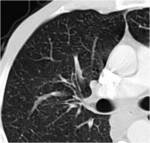
- Retractile opacity (+/- calcif) (fig.2)
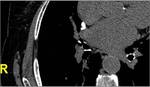
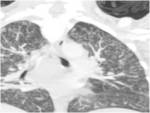
- Calcified hilar lymph nodes (fig.3)
- 2. Post primary tuberculosis:
Reactivation of a previously primary infection.
Rarely a continuation of the primary disease.
Lesions predominated in apical segments (O2).
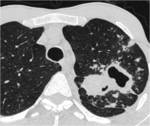
Parenchymal Disease with Cavitation
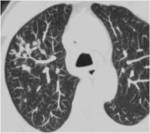
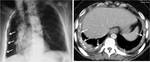
Airway Involvement : Centrilobular nodules connected to linear branching opacities (tree-in-bud).
(fig.4)
Pleural Extension
Chest Wall Tuberculosis: fistulization to skin ++
Parenchymal Disease with Cavitation (fig.5)
ü The cavities are most often multiple,
they may be isolated or develop in a alveolar condensation (fig.6)
ü The wall has a variable appearance: regular or thick and nodular
ü Content: aeric or air-fluid
ü Often Associated with a micronodular infiltration highly suggestive of the diagnosis
- 3. Miliary tuberculosis: (fig.7 and 8)
Hematogenous spread
Usually seen in the elderly,
infants,
and immunocompromised persons.
It can occur after a primary infection or after a post-primary tuberculosis.
Numerous,
fine,
clear limits micronodules with bilateral,
diffuse and uniform distribution
- 4. Pleural tuberculosis (fig.9)
Pleural effusions in PP tuberculosis are usually small.
Associated with subpleural parenchymal cavitation.
Tuberculous effusions are rich in protein and often contain filaments and fibrin partitions visible by US.
CT can reveal pleural effusion and parenchymal lesions very often associated.
Residual pleural thickening and calcification may be seen following therapy.
B- Tuberculosis involving the central nervous system
The central nervous system (CNS) localisation is one of the most severe expressions of tuberculosis.
2-5% of patients have a CNS lesion
Intracranial tuberculosis results in two related pathologic processes:
- Tuberculous meningitis
- Intracranial tuberculomas
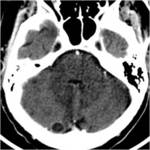
- Meningeal involvement (fig.10)
Tuberculous meningitis is more frequent manifestation of neurotuberculosis than is brain tuberculoma
CT \ MRI: intense,
often homogeneous enhancement after contrast materiel administration ,this enhancement extends into hemispheric fissures and over the cortical surfaces of the brain
Sequelae of meningeal involvement include hydrocephalus and infarcts in the middle cerebral artery distribution
2.
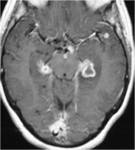
Parenchymal involvement (fig.11)
Cranial tuberculomas ++
Tuberculomas may be single or multiple
Can occur whith or wihout meningitis
CT findings:
- Rounded or lobulated masses that demonstrate ring enhancement
- Usually associated with moderate edema
- Calcification is uncommon
- Hypointense on T1,
Hyperintense on T2,
Homogenous enhancement.
- Caseating tuberculomas: Rim enhancement at contrast enhanced T1
3.
Spinal Tuberculous Meningitis: (fig.13)
Imaging finding:
Obliteration of the spinal subarachnoid space
Thick and linear intradural enhancement
C- Lymph node tuberculosis
The most common form of extrapulmonary tuberculosis
Cervical involvement + + Rarely axillary or inguinal
Indurate and fluctuating
Fistula in 10% of cases
D- Genitourinary Tuberculosis
It is as serious latent disease
- Renal Tuberculosis
Imaging finding:
- Renal calcification
- Moth-eaten calix due to erosions
- Cavitations of renal parenchyma (fig.15)
- Collecting system: Ulceration,
wall thickening,
and fibrosis characterize
2.
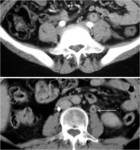
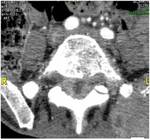
Ureteric Tuberculosis: (fig.16)
Seen in 50% of patients with genitourinary tuberculosis
CT may demonstrate thickening of the ureteral wall and periureteral inflammatory changes
This type of lesion occur hydronephrosis and hydroureter of varying degrees
E- Abdominal tuberculosis
- 1. Tuberculous Peritonitis:
Most common clinical manifestation of abdominal tuberculosis
Secondary to:
- Hematogenous spread
- Rupture of lymph node
- Gastrointestinal deposit or fallopian tube involvement
Nonspecific imaging:
- Ascites
- Thickening of the peritoneal layers
- Densification or nodular infiltration of mesenteric fat and omentum
- 2. Gastrointestinal tuberculosis:
CT is the best modality for evaluation of the parietal involvement and digestive complications (fistulas,
collections) (fig.18)
The ileocecal region is the most common area of involvement in the gastrointestinal tract due to the abundance of lymphoid tissue.
CT may show circumferential wall thickening of the cecum and terminal ileum associated with adjacent mesenteric lymphadenopathy (fig.20).
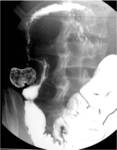
Barium studies demonstrate ulceration,
stenosis,
obstruction,
conical and retracted coecum (fig.19).
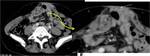
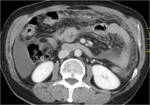
- 3. Lymphadenopathy (fig.21)
The most common manifestation of abdominal tuberculosis
Enlarged nodes with hypoattenuating centers and hyperattenuating enhancing rims at CT
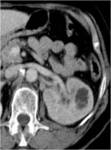
- 4. Hepatosplenic Tuberculosis (fig.22)
Common in patients with disseminated disease
Micronodular-miliary or macronodular,
Tendance to calcify
CT: lesions are hypo attenuating,
nonspecific and are similar to multiple metastases or abscesses.
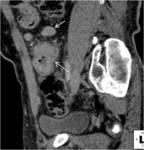
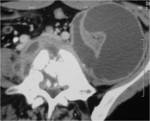
- 5. Adrenal Tuberculosis (fig.23)
Enlarged glands
Hypoattenuating necrotic areas with or without calcification
Fat infiltaration arround
F- Skeletal tuberculosis
- 1. Tuberculous Spondylitis (Pott Disease)
The spine is the most frequent site of skeletal tuberculosis
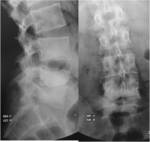
Radiography : (fig.24)
- Demineralization of the end plates
- Erosion of the anterior margin of the vertebral body
- Gap with sclerosis
- Progressive vertebral collapse
- Obliteration of the disk space
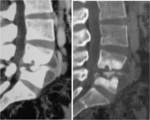
- CT is of great value in demonstrating a small focus of vertebral involvement and small parts abscess.
(fig.25 and 26)
- MR typical findings include a focal area of decreased signal intensity on T1-weighted images and increased signal intensity on T2-weighted images
- The most important differential diagnosis is pyogenic vertebral osteomyelitis.
- 2. Tuberculous Arthritis
The disease is typically monoarticular and primarily involves the large weight-bearing joints such as the hip and knee
Rradiologic abnormalities :Phemister triad,
consisting of periarticular osteoporosis,
peripherally located osseous erosion and gradual diminution of the joint space
Later : complete joint obliteration with fibrous ankylosis
CT and MR imaging (fig.27) are helpful in the depiction ++