Peroneal tendon
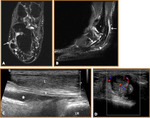
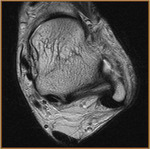
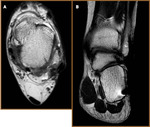
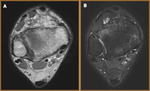
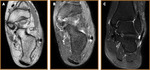
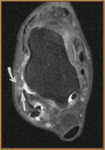
- Peroneal tendinosis (Fig 13)
- Non-inflammatory degenerative process within the peroneal tendons
- Athletes (m/c),
elderly individuals,
diabetics,
patients with inflammatory arthritis,
and individuals with displaced Fx of the lateral malleolus and calcaneus
-
Peroneal Tenosynovitis
- Inflammation of the tendon or tendon sheath
- m/c tendon disorders of the lateral ankle
- Etiology
- Trauma,
repetitive local stress,
systemic joint disorders
-
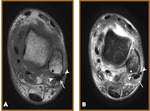
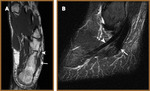
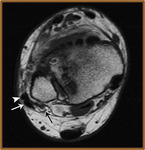
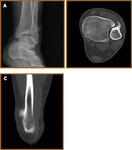
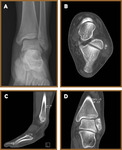
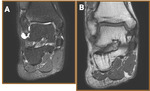
Peroneus Brevis Tears (Fig 14,
15,
16)
- Young athletes,
elderly
- Associated conditions
- ligamentous injuries
- insufficiency of the SPR
- thickening of the calcaneofibular ligament
- overcrowding of the retromalleolar groove
- Susceptible to degenerative tears
-
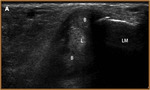
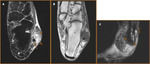
Peroneus Longus Tears (Fig 17)
- Isolated peroneus longus tendon tears
- Uncommon
- Level of the cuboid tunnel
- Associated with peroneus brevis tendon tears
: retromalleolar groove
- m/c condition of acute tears
- Direct trauma or sports-related injury
- Avulsion fracture of the os peroneum
: Os peroneum fragment separation (≥ 6mm)
- Degenerative chronic tears
- Mechanical friction
- Cuboid tunnel or a hypertrophic peroneal tubercle
Peroneal Retinaculum
- Dislocation and SPR Injuries
- Peroneal tendon subluxation
- Uncommon but not rare
- 0.3–0.5% of traumatic events to the ankle
- Peroneal tendon dislocation
- One or both tendons displace from the retromalleolar groove during ankle movement or muscle contractions
- Commonly a/w SPR injury
-
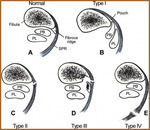
SPR injury (Fig 18,
19,
20)
- Acute inversion injury to the dorsiflexed ankle or during forced dorsiflexion of the everted foot
- Skiing,
skating,
soccer,
or football
- Congenital foot deformities
- Shallow or convex fibular groove
- Overcrowding of retromalleolar groove by the anatomic variants
- Fx of the distal fibula & calcaneus
- US and MRI
- Peroneal tendon dislocation and SPR injuries
- Dynamic US with a dorsiflexion-eversion maneuver
: more helpful for detection of intermittent dislocation
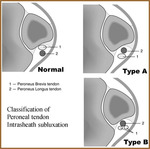
- Intrasheath Subluxation (Fig 21,
22,
23)
- Reverse anatomic locations of brevis and longus tendons within the peroneal groove
- Intact retinaculum
- Two subtypes (by Raikin)
- Dynamic ultrasound
- Subluxation of peroneus brevis and longus tendons over each other within the peroneal groove
: peroneus longus lie deep to the peroneus brevis tendon
- Intact superior peroneal retinaculum while dorsiflexion and eversion maneuver
Intartendinous Ganglion in PB (Fig 24)
Ligment Injuries (Fig 25,
26,
27,
28)
- Lateral ankle sprain
- 16-21% of all sports-related traumatic lesions
- Anterior talofibular ligament
- weakest ligament
- most frequently torn
- Anatomic classification (No.
of affected ligaments)
- 1st degree : partial or complete tear of ant.
talofibular lig.
- 2nd degree : partially or complete tear of ant.
talofibular &calcaneofibular lig.
- 3rd degree : injuries to ant.
talofibular,
calcaneofibular & posterior talofibular lig.
-
Acute rupture of the lateral collateral ligament
- Discontinuity,
detachment,
thickening,
thinning,
or irregularity of the ligament
- Heterogeneity with increased intraligamentous SI (fat-suppressed or T2WI)
- intrasubstance edema or hemorrhage
- Obliteration of the fat planes around the ligament
- Extravasation of joint fluid into adjacent soft tissues
- Talar contusions
-
Chronic tear
- Thickening,
thinning,
elongation,
and wavy or irregular contour of the ligament
- Residual marrow or soft tissue edema (-)
- Hemorrhage (-)
- Decreased SI in the fat abutting the ligaments (scarring/synovial proliferation)
Impingement syndrome
- Anterolateral impingement syndrome (Fig 29)
- Entrapment of abnormal soft tissue in the anterolateral gutter of the ankle
- Chronic lateral ankle pain
- Injuries to ATF & AITF ligaments,
accessory fascicle of AITF ligament
- Chronic lateral instability
- Repetitive synovial inflammation
- Soft tissue “mass” (hypertrophic synovial tissue,
fibrosis)
- MRI
- Abnormal soft-tissue mass or fibrous band in the anterolateral ankle gutter
- Low SI on T1WI, Low-,
intermediate SI on T2WI
Osseous Lesions
- Osteochondroma (Fig 30)
- Cartilage-covered osseous excrescences
- Solitary/multiple
- Long tubular bone
- Lower extremity > upper extremity
- Metaphyseal location
- Radiologic finding
- Osseous protuberance arising from external surface of long tubular bone
-
Fracture of Os subfibulare (Fig 31)
- Os subfibulare
- Accessory bone located under the tip of lateral malleollus
- 2.1% of individuals
- Persistence of an accessory ossification center
- Old non-united avulsion fractures
: swelling,
tenderness,
painful weight bearing,
painful range of motion and ankle effusion,
ankle instability
Ganglion Cysts (Fig 32)
- m/c soft tissue mass in the foot and ankle
- Origin sites
- tendon sheath
- joint
- bone (periosteal or intraosseous)
- soft tissue
- Intratendinous ganglion cysts of the ankle
- uncommon
- Etiology
- not completely understood
- recurrent injury to the tendon with subsequent cystic degeneration
- MR imaging
- Well-defined,
lobulated mass located adjacent to a joint or tendon sheath
- Simple or complex fluid-like signal
- Rim enhancement
- Fluid-filled tail that connects to the adjacent joint or tendon sheath (reliable sign)