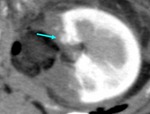
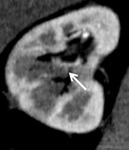
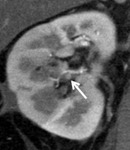
1.
The prevalence of the early vascular complications in perioperative 3D-CT
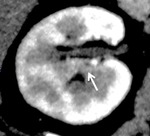
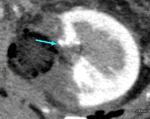
In axial CT image with a 1-mm thickness,
a total of 54 RAPs were found in 40 out of 78 cases (51.3%): the number of RAP was 0 to 3 in each patient,
and the diameter of the RAP was 2.0-16.6 mm with an average of 3.6 ± 3.3 mm.
The contrast extravasation was found in 6 out of 78 cases (7.7%).
The irregularity of the renal arterial branch (i.e.,
angiospasm or minor injury) was found in 45 out of 78 cases (57.7%): all of them were located in the second or more distal portion of renal artery branch.
There was no abnormality in the main renal artery.
The irregularity of the renal arterial branch was associated in cases with a RAP in 29 of 38 patients (76.1%) whereas the irregularity of the renal arterial branch was associated in cases without a RAP in 25 of 40 patients (62.5%),
however,
there was no statistical difference between them (P = 0.141,
Fisher's exact test).
In the 40 patients with a RAP,
the surgery had been undergone by LPN (n = 19) and OPN (n = 21); RAPs were located at upper pole (n = 14),
central part (n = 13) or lower pole (n = 13) in the right (n = 21) or left (n = 19) kidney.
2.
Clinical outcomes in cases with RAP detected in perioperative 3D-CT
There was a RAP in 40 of 78 patients (51.3%) in perioperative 3D-CT.
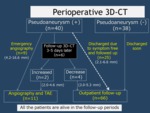
The clinical outcomes in cases with a RAP was shown in Fig. 1 .
Fig.1 Diagram of post-operative course in patients after partial nephrectomy
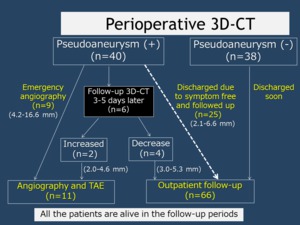
Fig. 1: Diagram of post-operative course in patients after partial nephrectomy
Of these patients,
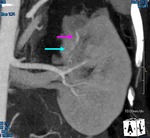
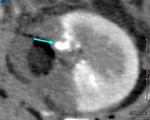
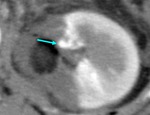
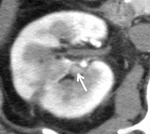
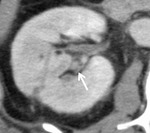
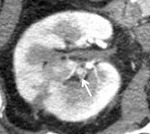
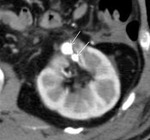
six patients (7.7%) were followed up by serial CT because of lack of clinical symptoms (See Case 1 (Fig. 2 Fig. 3 Fig. 4 Fig. 5 Fig. 6 Fig. 7 Fig. 8 Fig. 9).
The diameter of the RAP was 2.0-5.3 mm.
3D-CT was reexamined in all cases 3-5 days later.
As a result,
the RAP increased in two cases (diameter of the RAP,
2.0-4.6 mm: average,
3.3 mm) and disappeared or shrunk in four (diameter of the RAP,
3.0-5.3 mm: average,
4.3 mm).
Transcatheter arterial embolization (TAE) was performed for the former cases.
There was no relationship between the diameter of the RAP and short-term clinical outcomes.
3.
Clinical symptoms of patients with RAP
There was a RAP in 24 of 78 patients (30.8%) in perioperative 3D-CT who discharged and were followed up because of lack of clinical symptoms (anemia,
massive hematuria or unstable vital signs) and its small size (diameter,
2.1-6.6 mm).
On the day of initial follow-up after the discharge,
macroscopic hematuria was found in 1 of 24 (4.2%) and microhematuria was found in 16 of 24 (66.7%): there were no serious symptoms.
In all patients,
routine CT of 5-mm thickness was performed three weeks after discharge,
and the RAP was detected in none.
4.
Angiographic findings of RAPs
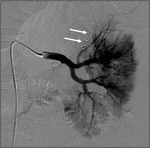
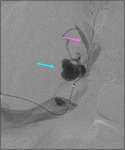
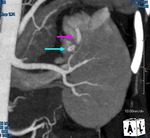
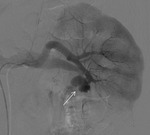
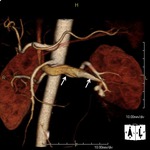
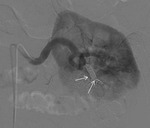
Angiography was subsequently performed in 9 of 78 patients (11.5%) in whom a RAP was detected perioperative 3D-CT (See Case 1 (Fig. 2 Fig. 3 Fig. 4 Fig. 5 Fig. 6 Fig. 7 Fig. 8 Fig. 9 and Case 3 (Fig. 16 Fig. 17 Fig. 18 Fig. 19)).
Also,
two patients (2/78: 2.6%) whose RAP increased in 3D-CT examinations 3-4 days later immediately underwent angiography.
As a clinical symptom,
macroscopic hematuria (7/11: 63.6%) (See Case 2 (Fig. 10 Fig. 11 Fig. 12 Fig. 13 Fig. 14 Fig. 15) Figures.
10-15),
decrease in hemoglobin level (8/11: 72.7%) (See Case 1 (Fig. 2 Fig. 3 Fig. 4 Fig. 5 Fig. 6 Fig. 7 Fig. 8 Fig. 9 and Case 3 (Fig. 16 Fig. 17 Fig. 18 Fig. 19)),
and hypotension or shock state (0/11: 0%) was noted.
Selective renal arteriography demonstrated a RAP in ten out of eleven patients (90.9%) and TAE using gelatin sponge,
microcoils,
or mixture of iodized oil and NBCA was performed in all cases (See Case 1 (Fig. 2 Fig. 3 Fig. 4 Fig. 5 Fig. 6 Fig. 7 Fig. 8 Fig. 9 and Case 3 (Fig. 16 Fig. 17 Fig. 18 Fig. 19)).
There was no major complications related to TAE,
the clinical symptom disappeared,
and the patients discharged soon.
However,
selective renal arteriography did not demonstrated an aneurysm in one case (1/22: 9.1%) in whom the a RAP increased in size from 2 mm to 3 mm in follow-up 3D-CT reexamination.
In that case,
angiospasm or thrombosis of the RAP might be concerned to the poor visualization of the RAP.
5.Difference in detection rate of early vascular complications among reconstruction methods
The detection rate of the early vascular complications in perioperative 3D-CT was shown in Table 2.
Table 2.
Difference in detection rate of early vascular complications among reconstruction methods
| Reconstruction methods |
RAP |
Irregularity of renal arterial branch |
Extravasation |
| 0.5-mm MPR image |
37/39 (94.9) |
53/53 (100.0) |
6/6 (100.0) |
| 1-mm axial image |
39/39 (100.0) |
45/53 (84.9) |
6/6 (100.0) |
| 5-mm axial image |
19/39 (48.7) |
22/53 (41.5) |
2/6 (33.3) |
| 50-mm slab MIP image |
24/39 (61.5) |
43/53 (81.1) |
1/6 (16.7) |
Notes: Numbers mean the number of cases,
and the numbers in parentheses indicate the percentages of the cases.
The detection rate of the RAP was good in the following order: 1-mm axial,
0.5-mm MPR,
50-mm MIP and 5-mm axial image.
In contrast,
the detection rate of the irregularity of renal arterial branch was good in the following order: 0.5-mm MPR,
1-mm axial,
50-mm MIP and 5-mm axial image.
The extravasation was seen in only 6 cases: 1-mm axial and 0.5-mm MPR image had a good imaging quality in visualization.
In addition,
there were two cases that a RAP was detected by 1-mm axial image but was not detected by MPR image and a case that a RAP was detected by 0.5-mm MPR image but was not detected by 1-mm axial image.