Type:
Educational Exhibit
Keywords:
Neoplasia, Efficacy studies, Diagnostic procedure, Decision analysis, Conventional radiography, MR, CT, Paediatric, Oncology, Neuroradiology peripheral nerve, Education and training
Authors:
F. Goncalves Menegotto, D. Mitchell , D. Toffoli , S. Emil, C. Saint-Martin ; Montreal, QC/CA
DOI:
10.1594/ecr2013/C-1355
Background
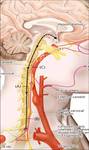
Horner’s syndrome classically corresponds to the clinical triad of miosis,
mild upper eyelid ptosis,
facial anhidrosis and/ or hyperemia.
Iris heterochromia,
apparent enophthalmos,
conjunctival congestion and ocular defective accommodation may also be observed.
These symptoms are related to injury of the oculo- sympathetic chain,
wether the lesion is central,
pre- or post-ganglionic in location.
(fig 1).
In children,
the etiologies of Horner syndrome should be subdivided into acquired and congenital causes (tab.1),
latest ones diagnosed during the first 4 weeks of life.
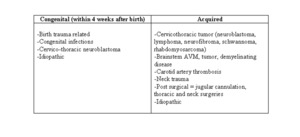
Table 1: Pediatric Horner Syndrome causes
Although benign processes are the commonest causes of interruption of the oculosympathetic pathway in children,
tumors such as neuroblastoma are not uncommon.
Overall,
lesions leading to Horner’s syndrome regardless the level of injury of the oculo-sympathetic chain,
are located in between the orbits and the upper chest cavity:
- Central Horner’s syndrome is mainly due to lesions involving the hypothalamus,
brainstem and medulla.
- Pre-ganglionic Horner’s syndrome is related to lesions of the neck and thoracic apex.
- Post-ganglionic Horner’s syndrome is usually related to lesions of the vascular chains of the neck,
base of skull,
orbital apex and cavernous sinus.
Partly due to rarity of the acquired pediatric Horner’s syndrome,
imaging recommendations in this clinical context are not well established.
However,
knowledge of its physiopathology and anatomy of the oculo-sympathetic chain will help to suggest a simplified and efficient radiological approach.