Patient characteristics
Between May 2012 and January 2013,
24 patients (14 women,
10 men; age range,
19 - 84 years; median,
39 years) referred for endovascular treatment were prospectively enrolled for this study performed according to the guidelines of our institution,
informed consent was obtained for each procedure.
Perfusion study was acquired in the angiographic suite during 10 brain arteriovenous malformation endovascular treatments and 14 intracranial aneurysm flow-diverter stent-assisted treatments.
FPCT CBV measurement
Both endovascular treatment and perfusion study were performed on a biplan angiographic system (Allura Xper,
Philips Healthcare,
Best,
the Netherlands) under general anesthesia.
FPCT CBV was assessed before embolization for brain AVM and after stent delivery for aneurysms.
Perfusion protocol consisted first in a test acquisition in order to obtain time intensity curves of tissue enhancement in brain parenchyma.
It corresponded to a 3 images per second subtracted postero-anterior fluoroscopic acquisition during 30 seconds.
It was initiated after an 8 second delay for central injections and 12 second delay for peripheral injections,
in order to minimize the X-ray dose.
Secondly FPCT CBV measurement was performed as previously reported (9),
but with a 5 second rotation time and a tailored acquisition delay from injection calculated from test acquisition.
Injection protocols
Injection protocols were the same for test acquisition and for CBV measurement.
Contrast media injections were performed either through a 4F pigtail intra-atrial venous catheter for 20 patients or through a peripheral cubital acces for 4 patients.
We used 72 mL of iodixanol (Visipaque 270,
GE Healthcare,
Mississauga,
Canada) at an injection rate of 4 mL/s,
followed by a 20 or 72 mL saline flush at the same rate.
Initially,
we used a literature inspired protocol (6),
consisting in the injection of the same amount of contrast media than saline flush (72/72 protocol).
From preliminary results this protocol was adjusted by decreasing saline flush volume to 20 mL for the following patients (72/20 protocol).
Post processing
Data were analyzed by using commercially available software,
2D Perfusion (Philips Healthcare,
Best,
the Netherlands) and exported to Excel software (Microsoft,
Redmond,
Washington,
USA).
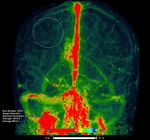
From a large region of interest drawn in the non-pathological hemisphere and avoiding major vessels we have determined time attenuation curves with a 0.33 second time resolution (Fig 3).
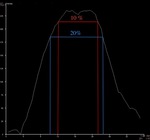
As steady state required strictness for the FPCT CBV measurement has not been previously evaluated in the literature we have arbitrarily chosen a 15% tolerance threshold from peak attenuation value (fig 4).
From this was measured the steady state length and the delay from injection to the steady state’s beginning.
Raw data from test injections (i.e.
digital subtraction angiography) were secondarily analyzed by two neuroradiologists (20 and 5 years of experience).
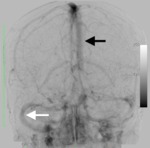
They determined delay from injection to full opacification of venous sinuses,
this is called “bolus watching” technique and it would be related the steady state’s beginning according to some authors (6,
7,
10)(fig 5).
When using “bolus watching” technique,
the rotational acquisition is manually initiated after contrast agent injection when the superior sagittal sinus is opacified.
Statistical analysis
Statistical analysis was performed using commercial statistical software SPSS (version 12.0,
Statistical Package for the Social Science,
Chicago,
IL).
Correlations between readers using “bolus watching” technique and the measured steady state delay from time density curves were performed using Spearman correlation coefficient.
Steady state’s average delay from “bolus watching” and from time density curves were compared using Wilcoxon rank sum test.
Average steady state’s length from different injection protcols were compared using Mann-Whitney U test.