Technique
We used a digital system to obtain both mammography and tomosynthesis images (Giotto TOMO,
IMS,
Bologna,
Italy; Fig.
1).
The unit acquires 13 projections with a low dose protocol on a ±20° angular range; detector is stationary.
Other technical aspects are:
- W-target X-ray source;
- a-Se digital detector (ANRAD,
LMAM) with a sensitive area 24x30 cm2 and squared pixel pitch0.085 mm;
- Iterative reconstruction algorythm
- Reconstructed voxel size: 0.085 mm×0.085 mm×1.0 mm
Exposure parameters are determined by Automatic Exposure Control (AEC).
AEC for DBT in one view was defined so as to deliver a radiation dose approximately 1.4 times that for digital mammography in one view.
Breast compression applied for DBT was less than for DM.
All patients underwent DBT both in cranio-caudal and in medio-lateral oblique view.
Patients
Between May 2012 and November 2012,
26 women with 31 malignant lesions identified by Digital Mammography or US and characterized with percutaneous needle-biopsy underwent DBT before surgery.
Mean age was 60.6 years (range 40-80 years).
Breast density according to ACR classification system was:
BIRADS 1: 6 patients
BIRADS 2: 6 patients
BIRADS 3: 12 patients
BIRADS 4: 2 patients
The 31 malignant lesions were:
- 2 high grade DCIS;
- 2 microinvasive ductal carcinoma,
1 with DCIS;
- 5 IDC grade 1; 2 with DCIS;
- 13 IDC grade 2,
2 with DCIS;
- 5 IDC grade 3,
1 with DCIS;
- 3 ILC grade 2;
- 1 ILC grade 2 with DCIS.
Lesion characterization
Findings suspicious for malignancy are usually classified as BIRADS 4 or 5.
They can be masses or microcalcifications.
Malignant masses are generally characterized by:
- Shape: oval,
round,
lobular or irregular;
- Margins: well defined,
indistinct,
spiculated;
- Density: high,
equal or low compared to parenchyma.
Suspicious microcalcifications are identified by:
- Appearance: amorphous,
pleomorphic or linear-branching;
- Distribution: cluster,
linear or segmental.
Table 1 summarizes lesion appearance.
Lesions margins could be clearly delineated in all cases:
|
Margins
|
|
|
Well defined
|
1
|
|
Indistinct
|
6
|
|
Spiculated
|
9
|
Density was higher than surrounding tissue for almost all lesions:
|
Density
|
|
|
High
|
11
|
|
Equal
|
5
|
|
Low
|
0
|
Thus,
the shape of the lesion could be clearly identified:
|
Shape
|
|
|
Oval/Round
|
5
|
|
Lobular
|
2
|
|
Irregular
|
9
|
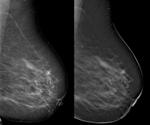
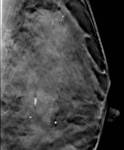
The high contrast between normal breast tissue and tumour can easily be recognized due to less tissue overlapping (Fig 2).
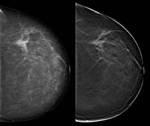
Often this difference in density creates a translucent halo around the lesion that makes both mass margins and spicules easier to identify (Fig 3).
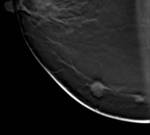
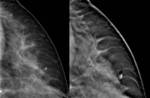
Spicules and architectural distortions can be easily distinguished from normal breast (Fig 4).
As in 2D-Mammography,
malignant masses present more often microlobulated or spiculated margins.
At the same time,
morphology of microcalcifications (usually linear or heterogeneous when malignant) can appear more evident (Fig 5).
The artefacts associated with calcifications are more often encountered for macrocalcifications,
usually benign,
and seem to be partially solved with the use of specific reconstruction algorithms [6].
We didn’t detect significant artefacts associated with microcalcifications (Fig 6).
Tomosynthesis shows some limits in the evaluation of their distribution: sometimes,
only one or two microcalcifications may be seen on a slice and so the perception of a cluster can become difficult.
Overcome this limitation could be possible with the use of Maximum Intensity Projection (MIP) reconstructions [7] or with use of devices developped by various vendors,
such as synthetic reconstruction of 2D-images or the acquisition of low-dose mammography in the central projections during DBT acquisition.
Scrolling the multiple images could also help recognizing normal anatomy,
microcalcifications distribution and evaluating the presence of a circumscribed lesion.
The possibility of a quasi-3D imaging can help in the visualization of normal breast anatomy,
both of the glandular tissue and of the vessels.
It must be considered that the appearance of this structure is quite different from that of Digital Mammography,
and so even radiologists already experienced in breast imaging and 2D-Mammography need an adequate training period.