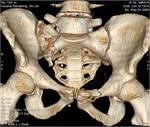
Pelvic fractures are found in 3-8% of patients with major trauma and accounted for 3.4% of all skeletal fractures.
Pelvic trauma is correlated with a significant level of morbidity and mortality and constitutes an important diagnostic problem and often damage of vascular structures is more clinically significant than skeletal (1).
These fracture are frequently associated with vascular,
visceral,
nerve and soft tissue lesions,
causing major complications.
Pelvic fractures,
which are associated with pelvic bleeding are therefore the most important cause of hemodynamic instability in patients with major trauma.
Complications can be classified according to the time factor in early,
intermediate and late.
When bleeding represents an early complication could lead an hypovolemic shock and an increase of morbidity and mortality can be observed.
Pelvic trauma is associated with bleeding and high early mortality in 5-18% of severe trauma,
with a mortality of 18-34% within the first 24 hours.
Bleeding can be venous from bone fractures,
from the venous or arterial plexus,
muscle or visceral,
often combinated.
Laceration of muscle or small-calibre veins can cause a self limiting hematoma characterized by low flow and developing within muscular or retroperitoneal fascia.
On the other hand arterial vessels and large caliber veins lacerations drive to active bleeding,
not self limiting,
requiring early diagnosis and prompt treatment,
as a condition rapidly leading to hipovolemic shock and death(2).
So depending of the source of bleeding,
arterial or venous,
pelvic hematoma can be not rilevant or rapidly progressive,
and for the same reason the treatment is deeply different.
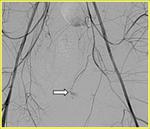
A rapidly expanding hematoma supported by an arterial bleeding needs angiographic embolization,
while a slow growing hematoma rising from a venous bleeding or from bone stumps,
has indication for a more conservative treatment as external fixator or pelvic packing.
Pelvic bleeding is strictly linked to the pelvic volume and restabilish the correct volume (closing the pelvic ring),
means bleeding reduction.
Several investigators have tried to define clinical or radiologic predictors to determine wich patients whit pelvic fractures are at high risk of arterial hemorrhage.
These predictor includes the response to initial resuscitation (3),
pelvic fracture pattern according to radiography results (1,4),
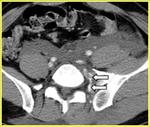
the volume and the location of pelvic hematoma according to the results of CT (5,6),
the extravasation of injected contrast material according to the results of CT and the presence of hypovolemia.
Therefore,
the contrast enhanced CT,
performed in urgency,
plays a fundamental role in identifying the presence of an active bleeding and in defining the origin,
thus directing the management of the patient.
Our purpose is to establish the role of CT in the detection of active hemorrhage after major pelvic trauma compared to angiography.