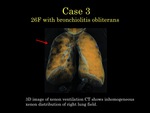
For all subjects,
we could successfully undergo xenon ventilation CT and obtained xenon enhanced images calculated with three-material-decomposition method.
No significant complications were noted with 35% xenon gas inhalation in all cases.
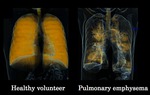
In all healthy volunteers,
xenon distribution in the lung fields were homogeneous and showed no distribution defect.
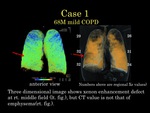
In case of COPD,
total decrease of xenon enhancement values and inhomogeneous distribution of xenon gas in the lung fields were well demonstrated in two and three dimensional images in all twenty cases(Figure1).
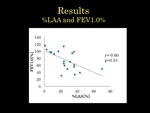
Mean xenon enhancement values in patients with COPD were significantly lower than those in healthy volunteers (19.45±6.9 vs 32.3±3.5 HU; p<0.01)(Figure 2).
In COPD cases,
mean xenon enhancement values showed significant positive correlations with forced expiratory volume [FEV1,
(r=0.55,
p<0.05)],
FEV1/forced vital capacity [FEV/FVC,
(r=0.53,
p<0.05)],
and peak flow rate [PEF,
(r=0.64,
p<0.01)](Figure 3,
4,
5).
%LAA scores showed significant negative correlations with FEV1/FVC (r=-0.60,
p<0.01),
FVC (r=-0.73,
p<0.01),
and PEF (r=0.64,
p<0.01)(Figure 6,
7,
8).
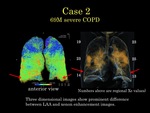
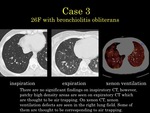
Some areas have severe discrepancies between LAA image and xenon inhalaion image,
where demonstrated as normal density area on LAA image although have no xenon distribution.
Those areas are thought to have small air way desease,
which were demonstrated as air trapping on expiration CT.
These air trapped areas tend to have small Xe value and have inhomogeneous xenon distribution at damaged lung field.
Xenon distribution and mean xenon value mesurement may have the possibility to evaluate those air way type COPD properly(Figure 9-12).