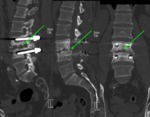
There must be adequate fixation to immobilize the spine while the bone graft heals to the vertebral segments.
The purpose of the spine instrumentation is to provide stability and reduce deformity and pain during the fusion process,
and should be keep in mind that is not designed to replace the bony elements of the spine.
Spinal instrumentation may eventually fail unless bone fusion takes place.
Over the past decades,
spinal instrumentation techniques have significantly increased.
Various diagnostic imaging techniques play an important role in the assessment of pre-operative and post-operative patients.
After spinal surgery,
imaging studies are performed to:
•Ensure the progression of bony fusion.
•Confirm the proper position and integrity of the instrumentation.
•Identify complications.
•Detect new disease or disease progression.
Fusion between bone graft and the intersomatic cage or osteosynthesis material is crucial to provide additional support and stability to the spinal instrumentation.
SPINAL IMPLANTS:
Spinal implants are made of many different materials,
shapes and sizes.
It is not the objective of this paper to review all them,
so just a wide review is done.
Spinal implants can be summarized into several groups:
- Screws.
- Wires.
- Plates.
- Rods.
- Bone graft.
- Interbody Cages.
- Screws
Screws can be used as fixation directly or can provide strong anchorage points where rods can be attached.
Screws can be placed in different ways:
- Transpedicular screws.
Fig.3.
In a study (1),
915 patients with 4790 transpedicular screws were reviewed,
finding:
- Complications related to screws: 2.4%
- Contact with the anterior cortex: 2.8%
- Exceed the cortex: 1.4%
- Pedicle fracture: 0.6 to 2.7%
- Dural Tear: 1%
- Nerve root irritation: 1% (medial or inferior position)
- Broken screw: 0.5 to 2.2%;
- Pseudoarthrosis incidence: 65%
- Late onset pain secondary to pseudarthrosis or screw placement,
which requires removal of the instrumentation.
-Translaminar screws.
- The screws are placed through the facet joints.
- The end of the screw should ideally be positioned within the lateral masses of C1.
-Transarticular screws.
- Typically used in odontoid fracture.
- Only the distal portion has notches for thread,
so that a rigid fixation occurs when force is applied between the screw head and the threaded end region.
-Fixation screws.
Fig.4.
- They are used in odontoid fracture.
Just the distal part of the screw is threaded; so a rigid fixation is achieved between the head of the screw and the lag distal part when tighten.
2.
Wires.
Fig.5.
Wires are placed as a tension band,
converting the tensile forces in compression forces.
They can be used alone,
mostly used in cervical spine to stabilize posterior vertebral elements and support bone graft,
or in combination with other devices to provide stability.
3.
Plates.
Fig.6.
Often used in the cervical spine.
Plates are manufactured to conform to the contour of the spine and are held in place by screws set into adjacent vertebrae.
- ANTERIOR: They are used in the cervical spine,
and should have a low profile.
Plates are fixed with screws,
which must be at least 2 mm from the plates
- POSTERIOR: Generally used in trauma.
4.
Rods.
Fig.7.
Rods are used,
along with hooks and screws,
to immobilize and to contour the spine into correct alignment.
There are different types:
- Posterior fixation with screws
- Harrington rod
- Growth rods: expansible
- Luque rods: usually attached with sublaminar wires
5.
Bone graft.
Fig.
8.
Typically used in conjunction with other instrumentation techniques.
The solid fusion of the bone graft can be radiologically identifiable usually after 6-9 months.
The complete stabilization is not achieved until bone fusion occurs.
CT is the technique of choice to assess graft fusion.
Different types of graft may be used:
- Autologous.
- Allogeneic.
- Demineralized bone matrix.
- Bone morphogenetic proteins (BMP).
6.
Interbody Cages.
Fig.9.
Most often placed between two vertebral bodies.
They are openwork structures filled with bone graft material to promote bone growth between the adjacent vertebrae.
Cages are used to restore lost disc height resulting from a collapsed disc and to relieve pressure on nerve roots.
INTERSOMATIC FUSION TECHNIQUES Fig.10.
All the mentioned techniques are intended to:
- Restore and maintain the disc space height.
- Maintain normal sagittal alignment.
- Increase the stability of the operated segment.
When intersomatic space height decreases,
results in:
- Narrowing of the conjunction foramen.
- Root compression.
- Loss the stability of the posterior longitudinal ligament (PLL).
When intervertebral fusion occurs Fig.11.:
- Intersomatic space increases.
- Decompress the foramina.
Correct fusion is achieved when:
- Lateral plain film in flexion and extensión demostrates:
-
- Absence of movement or
- Less than 3° change at intersegmental position.
- Absence of radiolucent area surrounding the implant.
- Minimum loss of disc space height.
- No implant,
graft or vertebra fracture.
- No sclerosis affecting the graft or the adjacent vertebra.
- Bone formation is visible in the cage or around it (2).
FAILED BACK SURGERY SYNDROME
Failed back surgery syndrome (FBSS) is a persistent low back pain following spine surgery.
The etiology of failed back surgery can be a failure to recognize adequately the initial focus of pain,
incorrect diagnosis,
suboptimal selection of surgery,
poor technique,
failure to achieve surgical goals (pseudarthrosis),
and/or recurrent pathology.
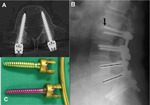
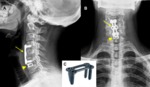
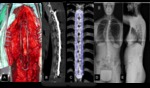
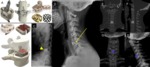
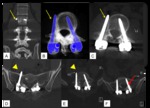
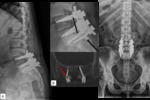
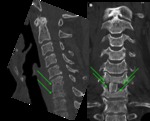
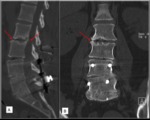
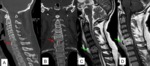
Fig. 1: Failed Back Surgery Syndrome
SIMPTOMATIC PSEUDOARTHROSIS
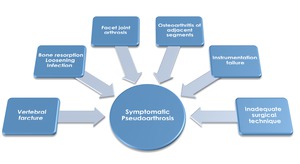
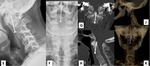
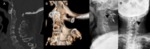
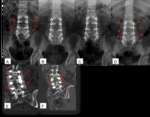
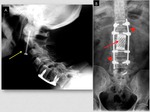
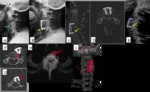
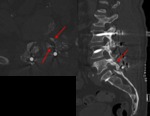
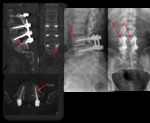
Fig. 2: Symptomatic pseudoarthosis
1. Inadequate surgical technique:
-Lumbar spine Fig.12:
Implant malposition has an estimated incidence of 5-41% in lumbar spine.
Screws can scroll:
- Medially → Invade the spinal canal
- Laterally → Invade conjunction foramina
- Anterior or laterally→ Invasion of the retroperitoneum
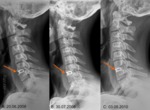
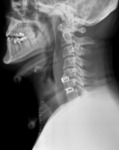
-Cervical spine Fig.13.:
Screws should be close to the cortex but not beyond it.
When placing an anterior plate,
screws can:
- Withdraw and protrude on soft tissues (eg.
great vessels,
trachea or esophagus)
- Completely surpass posterior cortical and protrude on the spinal cord.
2. Instrumentation failure:
-Migration of the osteosynthesis material Fig.
14,
15:
The posterior margin of the cage must be placed ≥ 2 mm from the posterior margin of the vertebra
Multiple causes:
- Osteosynthesis material is overdimensioned.
- Material placed too anterior →Rule out aortoiliac invasion.
-Fractures: Fig.
16,17,18
Usually due to fatigue and repetitive stress occasioned by spinal movements.
The fracture does not always indicate instability,
but is associated with greater mobility,
instability and pseudoarthrosis.
The prominence of the instrumentation can lead chronic tissue irritation,
causing pain,
formation of a bursa and even pressure pain and tissue necrosis.
Could be an indication of removing the osteosynthesis material.
Some intersomatic spacers require,
for their insertion,
to perform one groove in the vertebral bodies.
Fractures associated with the insertion of these devices have been described,
probably due to weakness in the edplate where the keel of these devices is positioned.
-Metallosis: Metallosis occurs when abrasion of metal components produces metallic debris which builds up in the periprosthetic soft tissues. Fig.19.
3.
Bone resorption:
-Collapse of implant Fig.
20:
Vertebral fractures usually affect the cranial endplate because it is thinner and supported by less-dense trabecular bone.
The concave central portion of the endplate is weaker than the peripheral zone.
Therefore,
there is higher risk of collapse if the implant is not large enough to anchor the stronger peripheral ring.
It is called migration when the cage sinks ≥ 3 mm in the adjacent vertebra
There’s no a well-known correlation between the implant sinking and clinical symptoms.
If collapse is too large may bulge:
- Posteriorly → on the thecal sac and roots.
- Anteriorly → on the great vessels.
David reported a collapse rate of 9%.
(4)
Van Ooij et al (5) reported collapse in 18 of 27 patients,
with underestimation of the size of osteosynthesis material in 10 of the 18.
-Osteolysis: Bone resorption around the screw or implants which are in close contact with bone. Fig.21,
24.
- Bone weakness
- Predispose to fracture
- Leads to hardware failure.
4. Facet joint arthrosis.
- Dooris et al (6) found that the location of the prosthesis in the disc space contributes to the development of osteoarthritis.
- Especially,
when the material is placed too anterior,
facet joints support a load 2.5 times greater than if the material was well placed.
- In 2005 Lemaire et al (7) described osteoarthritis facet 11 of 107 patients in which,
on sagittal images,
the osteosynthesis material was placed too anterior.
5. Adjacent segments arthrosis.
Fig.
22.
- Huang et al (8) demonstrated a correlation between the range of mobility of treated levels and the rate of degeneration of adjacent segments.
- 42 patients were evaluated:
The development of facetary arthrosis is influenced by the location of the prosthesis in the disc space.
HETEROTOPIC OSSIFICATION:
- No correlation with clinical symptoms.
- Lemaire et al.
(4) showed that ossification in the lateral face of the osteosynthesis material leads to fusion,
whereas lateral ossification produces continuous mobility.
- They thought that ossification occurs after the 5th year after implant placement.
- Ossification of the anterior longitudinal ligament occurs most frequently when the anterior plate is placed closely to nonfused disc space.
- It can be avoided by placing a plate whose length exceeds the vertebral margin ≥ 5mm.
COMPLICATIONS:
- EARLY: Hematoma,
Seroma,
CSF leakage,
CSF leakage,
Infection,
Malposition.
- LATE: Migration,
Loss of instrumentation,
Loss of instrumentation,
Fractured or failed instrumentation.
|
COMPLICATION
|
INCIDENCE RATES
|
|
Pseudoarthrosis
|
5- 32%
|
|
Instrument failure
|
2- 15%
|
|
Neurologic
|
3- 11%
|
|
Implant removal
|
7- 25%
|
|
Removal for pain
|
2- 3%
|
|
Iatrogenic flat back syndrome
|
2- 3%
|
|
Infection
|
1- 2,4%
|
Cervical spine:
Fountas et al.
(5)in a retrospective study of 1015 patients with anterior cervical discectomy,
described as most frequent complications:
- Dysphagia (9.5%)
- Postoperative hematoma (5.6%)
- Recurrent laryngeal nerve palsy (3.1%)
Infection. Fig.
23,25:
- Incidence: 0.6 to 2%.
- Staphylococcus epidermidis and Propionibacterium acnes (4)
- During surgery
- During the immediate postoperative period
- During the late postoperative period.
The instrumentation should be removed if infection occurs after the first year since surgery and fusion is already well established.
IMAGING TECHNIQUES:
Different imaging techniques may be used in the evaluation of the spinal instrumentation
-Plain films:
- It is essential to perform preoperative and immediatly postoperative plain films which are used as starting point for comparison in later controls.
- Instrumentation failure or migration can be easily evaluated with serial plain films.
-Nuclear medicine techniques:
- Useful for the evaluation the surgical site for a year or even more.
-Ultrasound:
- Rarely used,
especially for evaluation of superficial collection or abscess.
-RM:
- Less used due to metal artifacts (use titanium reduces metal artifacts)
-CT:
- Very useful.
It is able to demonstrate the position of the instrumentation,
the alignment,
the spinal canal and possible complications such as pseudoarthrosis.
- CT is the gold standard,
however,
the occurrence of metal artifacts is its main handicap.
- In order to reduce artefacts caused by instrumentation and improve image quality,
various strategies have been developed:
- Optimize technique:
- Lower pitch.
- Higher current tuve(230-350 mAs)
- Higher peak kilovoltage(140 Kv).
- Optimize reconstruction algorithms:
- Using soft tissue reconstruction filters rather edge-enhancing algorithms.
- Dual energy images Fig.26:
- Dual energy techniques also can improve image quality reducing metal artifacts.
- Images are obtained at different kilovoltage (80 and 140 kV).
- High kilovoltage images (140Kv) better depict soft tissues and show lower metal artifact than coventional images,
so a better assessment of the hardware can be done.