The final histological diagnosis of the 27 lesions identified was:
- IDC (invasive ductal carcinoma) for 21 lesions (77,78 %)
- ILC (invasive lobular carcinoma) for 4 lesions (14,81 %)
- DCIS (ductal carcinoma in situ) for 2 lesions (7,41%)
ACR BI-RADS density score in the 23 patients was as follows:
1 = 5 patients (21,74%)
2 = 7 patients (30,43%)
3 = 10 patients (43,48%)
4 = 1 patient (4.35%)
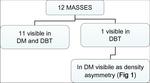
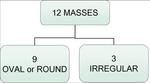
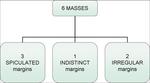
Of the 27 lesions: 12 (44.4%) presented as simple masses,
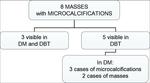
8 as masses and microcalcifications (29.6%) and 7 as microcalcifications (26.0%),
considering both DM and DBT.
Overall:
- 19 lesions (70.4%) were detect by both imaging modalities,
with similar appearance;
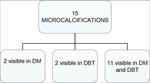
- 2 on 27 lesions (7.4%) were recognized only with DM (in both case they were interspersed calcification and just few of them was present per-slice at DBT,
thus the appearance was non-suspicious.
Histological diagnosis was DCIS);
- 1 lesions (3.7%) was clearly identified as a mass only by DBT,
while DM showed density asymmetry.
These results are summarized in table A.
Table A
|
|
DM
n°
|
DBT
n°
|
DM and DBT
n°
|
Total
n° (%)
|
|
Masses
|
0
|
1
|
11
|
12 (44,4%)
|
|
Microcalcifications
|
2
|
0
|
5
|
7 (25,9%)
|
|
Mass+microcalcifications
|
0
|
5
|
3
|
8 (29,6%)
|
Of the 5 cases in which only DBT identified microcalcifications associated with a mass,
the lesions were visible in Mammography as:
- only microcalcifications (3 cases);
- only masses (2 cases).
None of the lesions presented with both the modalities as architectural distorsion or density asymmetry exclusively.
Masses and masses with microcalcifications
Table 1 and Table 2 summarize the cases presenting as masses or masses with microcalcifications.
We considered the appearance of the masses recognized by both DM and DBT (14 out of 20 cases,
70.0%),
evaluating also the appearance of masses associated with microcalcifications.
We excluded the cases in which in DM only microcalcifications or only a density asymmetry was identified.
Regarding shape,
the appearance of the lesion was the same for both modalities in 12 on 14 cases (85.7%) (Table 3).
The other 2 cases visible with both modalities:
- 1 case: lesion oval in DM while lobulated in DBT;
- 1 case: lesion oval in DM while irregular in DBT.
Regarding margins,
the appearance of the tumors was the same for both modalities in 6 in 14 (42.9%) cases (Table 4).
The other 8 cases visible with both modalities presented:
|
|
DM-MARGINS
|
DBT-MARGINS
|
|
7 CASES
|
Indistinct
|
spiculated
|
|
1 CASE
|
Irregular
|
spiculated
|
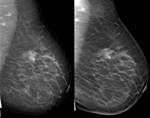
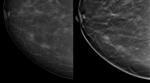
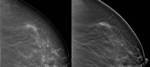
- Lesion morphology was comparable in cases with masses visible both at DM and DBT,
but DBT helped in 8 out of 14 of these cases (57.1%) to better define margins (Fig.
2).
In half of these cases (4 out of 8),
breast density was high (BI-RADS density 3 or 4).
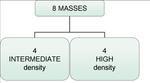
Regarding density,
the appearance of the tumors was the same for both modalities in 8 on 14 cases (57.1%)(Table 5).
The other 6 cases visible with both modalities all presented intermediate density in DM while high in DBT.
None of the lesions presented with low density.
- Lesion density compared to breast parenchyma appears more often higher in DBT,
so the lesions result more conspicuous.
Microcalcifications
Table 6 summarizes the cases presenting as microcalcifications.
Considering all 15 cases presenting with microcalcifications,
8 had an associated mass (5 cases only in DBT and 3 cases also in DM).
We considered the appearance of microcalcifications only.
Regarding type,
the appearance of microcalcifications was the same for both techniques in 5 on 11 cases (45.4%):
- 2 were amorphous;
- 3 were punctate.
The other 6 cases visible with both modalities:
|
|
DM-type
|
DBT-type
|
|
2 CASES
|
Punctuate
|
Pleomorphous
|
|
2 CASES
|
Amorphous
|
Pleomorphous
|
|
1 CASE
|
Punctuate
|
Linear-branching
|
|
1 CASE
|
Pleomorphous
|
Amorphous
|
Regarding distribution,
the appearance was the same for both techniques in 10 out of 11 cases (90.9%) (Table 7).
The other 1 case was described as a cluster in DM while linear in DBT.
- Almost no difference was found in the 2 methods regarding the assessment of distribution of microcalcifications,
while some discordance was evident regarding their morphology.
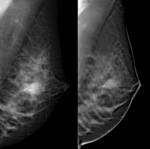
- DBT identified a mass associated with microcalcification in 3 out of 13 cases of microcalcification visible at DBT (23.1%) (Fig 3).
Architectural distortion was also identified,
alone or in association with a mass and/or microcalcifications in 7 lesions in DBT.
None was visible in DM.
In 2 cases,
architectural distortion was instead only visible in DM.
In DBT,
dense malignant lesions and spiculations presented with a lucent halo that helped the identification (Fig 4).
Also,
the scrolling proved to be useful in the identification of circumscribed areas.
Our results are in agreement with some articles already published that underline the equivalence of DBT to DM in the identification of breast lesions [4,5].
However,
it has been postulated that although higher conspicuity may provide radiologists with more confidence in making clinical decisions,
this could not allow an effective improvement in diagnostic performance [6].
Regarding clinical microcalcifications assessment by DBT in terms of detection and characterization,
there are only few data from literature.
Some studies report a decreased sensitivity of DBT in detecting microcalcifications: this could be explained by the fact that interspersed calcification are well represented on superimposed 2D-images,
while just few of them can be seen per slice at 3D-imaging.
To solve the drawback of poor visibility of microcalcification at DBT,
some manufactures are suggesting the use of maximum intensty projections (MIP) images [5].