Population
During a 7 months period (from November 2011 to may 2012) we retrospectively obtained 51 surgical specimens (44 mastectomies and 7 quadrants) from 51 patients with an age range 40-86 (mean age 60.5 years).
We chose only specimens with thickness of at least 2 cm,
that was the less thickness required to perform DBT.
For this reason the number of mastectomy in our study population was higher than the one of quadrantectomy. All patients referred to surgery for a histological proved breast cancer obtained from preoperative US core needle biopsy or stereotactic vacuum assisted biopsy performed in our Institution.
Approval of the institutional review board was obtained before the collection of the data. A total of 67 breast cancer were at the pathologic examination of the specimen,
used as the standard of reference.
Surgical procedures were performed in our Hospital and consist in BCS (breast conservative surgery) or mastectectomy,
concomitantly with sentinel lymph node mapping in all patients.
The pectoral fascia was included in all patients with lesions close to the chest wall.
An ellipse of overlying skin was included when lesions were very close to the skin.
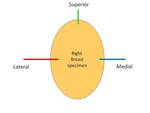
The surgeon marked the margins of the specimen with a short suture for the superior margin,
a long suture for the lateral margin and a middle suture for the medial ones.
In this way it was possible to orient each specimen (Fig. 1 ).
Imaging protocol
After orienting the specimen we sequentially performed DM and DBT by using the same digital system (Giotto TOMO,
IMS,
Bologna,
Italy),
which implements: (i) a W-target x-ray source,
combined with Rh-filter or Ag-filter depending on breast thickness; (ii) an a-Se digital detector (ANRAD LMAM),
with a sensitive area of 24×30 cm2 and a squared pixel pitch of 0.085 mm.
Surgical specimens were positioned in the system and anteroposterior view were performed DM and after 90° rotation of the specimen another perpendicular view were performed.
The DM position corresponding to the largest thickness of the specimen was used to perform one single DBT view.
For DBT,
the movable x-ray source spanned an overall angular range of ±20°,
acquiring 13 projections at the requested position.
Exposure parameters were determined by Automatic Exposure Control (AEC).
AEC for DBT in one view was defined so as to deliver a radiation dose approximately 1.4 times that for digital mammography in one view.
Image reconstruction was based on an iterative method that used Total Variation (TV) regularisation,
and by default reconstructed voxel size of 0.085 mm×0.085 mm×1.0 mm.
Image analysis
Images were reviewed in separate sessions on a dedicated workstation (Raffaello,
IMS,
Bologna,
Italy) by two radiologists with more than 10 years of experience in breast imaging.
Both readers were blinded to lesions dimension and pre- and post-surgical histopathological results.
DM and DBT images of the same patients were presented in independent reading sessions separated by a 4 week interval in order to avoid recall bias.
In each reading session,
DM and DBT cases were showed randomly.
All discordant results were resolved by consensus.
For each specimen,
readers recorded – both on DM or DBT images - the number of malignant lesions they detected,
together with the lesion type according to the following categories:
- mass;
- microcalcifications cluster;
- mixed lesions (in the case of a combination of the two former types).
They also recorded their subjective impression of lesion detectability,
defined as lesions visibility against the background of fibro-glandular tissue (detectability score).
For this analysis a 1-5 score was used as follows: 1=very low; 2=low; 3=mild; 4=good; 5=very good.
Moreover,
for the lesions seen with both imaging techniques (excluding lesions classified as microcalcifications),
the readers give a subjective impression of the visibility of lesions.
Margins visibility was expressed as a dichotomic value as follows: 1 when ≥50% of lesion margins were visible (fully visible) and 0 when <50% of margins were visible.
Data Analysis
Analysis was performed on a per-lesion basis.
We estimated the diagnostic yield (DY) of DM and DBT as the ratio between the number of correctly detected lesions over the total number of lesions found at histopathological examination ( Fig. 2 ).
Binomial exact 95% C.I.
were calculated.
For the lesions seen with both technique we compared the image detectability scores of the two techniques by using the Wilcoxon signed-rank.
Statistical significance was assumed for an alfa value less than 0.5.
The concordance in the visualization of margins between DBT and DM was evaluated with weighted-Kappa.