INTRODUCTION:
An intraspinal tumour is an abnormal mass of tissue within or surrounding the spinal cord and spinal column.
Intraspinal tumours may originate from the spinal cord,
filum terminale,
nerve roots,
meninges,
intraspinal vessels,
sympathetic chain,
or vertebrae.
They can be benign or malignant,
primary or secondary,
and may result in serious morbidity.
Intraspinal tumours are relatively uncommon lesions accounting for approximately 15% of craniospinal tumours.
However,
these lesions can cause significant morbidity and can be associated with mortality as well.
In establishing the differential diagnosis for a spinal lesion,
location is the most important feature.
Spinal tumours may be referred to by the area of the spine in which they occur.
The basic areas are cervical,
thoracic,
lumbar,
and sacral.
Additionally,
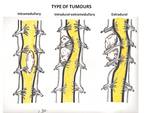
they are also classified into 3 main categories according to the their location with respect to the dural sac and spinal cord: extradural; intradural-extramedullary; or intramedullary (Fig. 1).
Lesions can occasionally compromise more than one compartment.
Extradural (55%-60% of all spinal tumours): They originate outside the dural sac.
They may derive from the cells covering the nerve roots,
from the vertebrae (most extradural lesions),
or from the epidural tissues.
Occasionally,
an extradural tumour extends through the intervertebral foramina,
lying partially inside and partially outside the spinal canal.
Metastases are the most frequent extradural lesions.
Intradural-extramedullary (30%-40%): These tumours develop in the spinal cord’s arachnoid membrane (meningiomas),
in the nerve roots that extend out from the spinal cord (schwannomas and neurofibromas),
or at the base of the spinal cord (filum terminale ependymomas).
Most of these lesions are primary.
Drop metastases can be also observed at this location.
Intramedullary (5%-10%): These tumours grow inside the spinal cord,
most frequently in the cervical region.
They typically derive from glial or ependymal cells that are found throughout the interstitium of the cord.
Most (90%-95%) are malignant.
Ependymomas and astrocytomas are the two most common types.
Ependymomas are the most frequent in adults and astrocytomas are the most frequent in children.
ETIOLOGY:
The cause of most primary spinal tumours is unknown.
Some may be attributed to exposure to cancer-causing agents.
Spinal lymphomas are more common in people with compromised immune systems.
Some are related to a genetic component.
In a small number of cases,
primary tumours may result from these genetic diseases: Neurofibromatosis (type 1 or 2) and Von Hippel-Lindau (VHL) disease.
- NF2>NF1
- NF2: Ependymomas,
schwannomas,
meningiomas
- NF1: Astrocytomas,
neurofibromas
- VHL: Hemangioblastomas
SYMPTOMS:
Intraspinal tumours often present with nonspecific symptoms.
Non-mechanical back pain is the most frequent symptom.
Pain may spread beyond the back to the hips,
legs,
feet,
or arms,
and it may worsen over time.
Depending on the location and type of tumour,
other signs and symptoms can develop,
especially as a tumour grows and compresses on the spinal cord,
the nerve roots,
blood vessels,
or bone of the spine.
Impingement of the tumour on the spinal cord can be life-threatening in itself.
Additional symptoms can include:
-Loss of sensation or muscle weakness in the legs,
arms,
or chest.
-Difficulty walking,
which may cause falls.
-Loss of bowel or bladder function.
-Paralysis in different parts of the body,
depending on which nerves are compressed.
-Scoliosis or other spinal deformity resulting from a large but benign tumour.
DIAGNOSIS:
Magnetic resonance imaging (MRI) is the most important diagnostic tool for intraspinal tumours,
playing an integral role in their evaluation and improving their anatomic delineation and early diagnosis.
MRI can show the spinal cord,
nerve roots,
and surrounding areas.
One should always obtain sagittal and axial unenhanced T1- and T2-weighted images and contrast-enhanced T1-weighted images.
Contrast-enhanced images can be important for tumour detection,
delineation,
characterization,
and grading.
They help differentiate the tumour from the spinal cord,
nerve roots,
or thecal sac as well as from peritumour edema or cysts.
They are also crucial to ensure correct staging and treatment planning.
MRI also plays an important role in follow-up.
Computed tomography remains the best modality to assess the osseous structures.
Sometimes CT shows typical patterns of bone destruction,
sclerosis,
and/or remodeling.
CT is especially important in planning instrumentation,
although this is usually not required for intradural tumours,
as the vertebral bodies are nearly always essentially unaffected.
Plain Film Radiography provide information about osseous anatomy: alignement,
bone matrix,
bone destruction,
sclerosis and demineralization.
Bone scintigraphy is useful in detecting multiple spinal bone lesions and distant metastases.
Angiography is useful in a select group of patients who have vascular lesions (both vascular malformations and vascular tumours),
and in some instances endovascular treatment may also be useful.
Ultrasound,
except in infants,
does not have a role,
as it is unable to image the intradural compartment due to the overlying posterior spinal elements.
After radiological confirmation of the tumour,
the only way to determine whether the tumor is benign or malignant is to examine a small tissue sample (Biopsy).
TREATMENT:
Surgery is the most common treatment,
and in most cases the neurological symptoms improve postoperatively.
Primary spinal tumours may be removed through complete en bloc resection for a possible cure.
In patients with metastatic tumours,
surgical treatment is primarily palliative,
with the goal of restoring or preserving neurological function,
stabilizing the spine,
and alleviating pain.
Indications for surgery include intractable pain,
spinal cord compression,
and the need for stabilization of pathological fractures.
Nonsurgical treatment options include observation,
chemotherapy,
and radiation therapy.
Watchful waiting with regular MRI monitoring can be an option in tumours that are asymptomatic or mildly symptomatic and do not appear to be changing/progressing.
OUTCOME:
Outcome depends greatly on whether the spinal tumour is benign or malignant,
primary or metastatic,
on the histologic grade of tumour and on the age and overall health of the patient.
The extent of surgical resection is also a predictor of outcome.
In the case of primary tumours,
the goal is to remove the tumour completely,
leading to potential cure.
In the case of metastatic tumours,
the goal is almost always palliative. At best,
palliative treatment may provide the patient with an improved quality of life and prolonged life expectancy.